Case Report
Massive Acetabular Bone Loss Reconstructed with a Custom Triflange Acetabular Component during Revision Hip Arthroplasty
Thomas R Sperring1, Elke Wintermeyer1,2, Michael J DeRogatis1, Paul E Di Cesare1 and Paul S
Issack1*
1Department of Orthopedic Surgery, New York - Presbyterian Hospital, USA
2Department of Trauma and Reconstructive Surgery, BG Trauma Center, Germany
*Corresponding author: Paul S Issack, Department of Orthopaedic Surgery, New York - Presbyterian Hospital, 170 William Street, New York, NY 10038, USA
Published: 05 Nov, 2018
Cite this article as: Sperring TR, Wintermeyer E, DeRogatis
MJ, Di Cesare PE, Issack PS. Massive
Acetabular Bone Loss Reconstructed
with a Custom Triflange Acetabular
Component during Revision Hip
Arthroplasty. World J Surg Surgical
Res. 2018; 1: 1073.
Abstract
Reconstruction of the failed acetabular component in the setting of massive bone loss and acetabular
fracture is one of the most difficult technical challenges in orthopedic surgery. Custom Triflange
Acetabular Components (CTAC) has been shown to be useful for managing massive bone loss with
pelvic discontinuity. Here we present a case of a patient with massive bone loss stemming from
a history of a complex acetabulum fracture and periprosthetic infection which was successfully
reconstructed using a CTAC.
Keywords: Arthroplasty; Reconstruction; Triflange acetabular
Introduction
Massive acetabular bone loss in the setting of revision total hip arthroplasty poses severe reconstructive challenges. The loss of bony anatomy limits areas for implant in-growth and screw fixation, thus compromise in the durability of the prosthesis. For severe, Paprosky type 3B bone loss, the custom triflanged acetabular component has been shown to be a useful approach to managing catastrophic bone loss [1-5]. Here we present the case of a construction worker who required revision of the acetabular component in the setting of massive acetabular bone loss. His bone loss stemmed from a history of major pelvic trauma, including a right acetabular fracture and posterior hip dislocation requiring anterior and posterior acetabular plating. He subsequently developed femoral head avascular necrosis which required conversion to a total hip replacement. Seven years later he developed a deep periprosthetic infection which further complicated his course requiring two stage revision hip replacement surgeries with reconstruction using highly porous augments. This resulted in the present situation: gross aseptic loosening of the acetabular component with massive bone loss. The patient was informed that data concerning the case would be submitted for publication, and the patient agreed.
Case Presentation
A 45-year-old construction worker was injured when a lamp post fell on him, 10 years prior
to the present admission. He sustained an associated both columns right acetabulum fracture with
a posterior right hip dislocation, as well a left-sided sacroiliac joint diastases. He underwent left
iliosacral screw fixation, and right acetabular fixation using anterior and posterior column plating.
Approximately six months after surgery the patient went on to develop symptomatic avascular
necrosis of the right femoral head with posttraumatic arthritis. This required conversion to a right
total hip replacement after removal of the posterior column plate. The patient did very well after
his hip replacement for approximately seven years. He then began to develop significant pain in
his right hip with difficulty ambulating. An infection work-up demonstrated an elevated serum
C-reactive protein and erythrocyte sedimentation rate and positive hip aspiration (Staphylococcus
aureus), which were consistent with chronic periprosthetic infection. The patient underwent
removal of the prosthesis and placement of an antibiotic spacer. He then received six weeks of IV
antibiotics followed by followed by a six week antibiotic holiday. After it was clear that the infection
was eradicated based on normal CRP and ESR and normal intraoperative frozen section, a new
total hip prosthesis was implanted. Because of the significant superior bone loss a highly porous
augment was placed in the posterior-superior acetabulum and a standard hydroxyapatite coated acetabular shell was used (Stryker, Mahwah, NJ, USA). The femur was
reconstructed with a modular fluted titanium stem (19 mm + 20 cone
body, 155 mm × 15 mm conical stem; Restoration Modular, Stryker).
The patient functioned very well for the next 2 1/2 years. However
over the past two months the patient has had activity-related pain
with increasing difficulty walking and shortening of his right leg.
Radiographs of the pelvis at this time demonstrated gross loosening
of the acetabular component (Figure 1A). The augment was wellfixed.
The femoral head was articulating superiorly with the augment.
CRP and ESR were normal. Judet views of the pelvis demonstrated
massive posterior and anterior column bone loss (Figure 1B and 1C).
Computed Tomography (CT) scanning of the pelvis with 2.5 mm
axial cuts demonstrated massive acetabular bone loss with severely
deficient anterior and posterior columns. The decision was that
made to reconstruct the acetabulum using a custom triflange implant
(Zimmer-Biomet, Warsaw, IN, USA). Based on the CT scan, three
dimensional images of the pelvis were created (Figure 2A and 2B).
Based on these images, a plastic model of the pelvis and implant
were then constructed (Figure 3A and 3B). Those models were the
template for construction of the actual custom triflange acetabular
component (Figure 4).
The previous posterior approach was used to access the
acetabulum. The incision was extended further proximally just 5 cm
short of the posterior superior iliac spine. Skin and subcutaneous
tissue were divided. The lateral fascia of the thigh was divided in
line with the fibers of the gluteus maximums and retracted with a
Charnley retractor. The scarred external rotators and capsule released
from the posterior lateral aspect of the greater trochanter. Exposure
was carried posteriorly to the greater and lesser sciatic notch is to
expose the ischial tuberosity. Proximally the gluteus medially was retracted anteriorly with a Steinman pin. This allowed for exposure
of the acetabulum, the ilium just proximal to the acetabulum and
the ischial tuberosity. The hip was dislocated and the prosthetic
femoral head (36 mm + 5) and proximal modular body of the femoral
implant (19 mm + 20 cone body, Restoration Modular, Stryker) were
removed. The acetabular component, screws and augment were then
removed. A high speed burr was then used to remove areas of bone
that interfered with flush seating of the implant. Synthetic bone graft
(Vitoss, Stryker, Mahwah, NJ, USA) was then placed into the defects
within the acetabulum (Figure 5A). The custom triflange acetabular
component was then positioned into the acetabulum. Several locking
and cortical screws were then placed into the dome, the iliac flange
and the ischial flange. The polyethylene liner was then locked into
the cup (Figure 5B). The proximal body of the femoral component
(19 mm + 10) was then attached to the distal stem and locked in the
appropriate anteversion using a set screw. A 36 mm + 5 cobalt chrome
head was impacted onto the trunnion and the hip was reduced. The
hip demonstrated stability through a full range of motion. The patient
was allowed to ambulate 20 lbs. toe touch weight bearing for 8 weeks.
Antibiotics were continued for 72 hrs. Low molecular weight heparin
was used for thromboembolic prophylaxis for 6 weeks. Three months
after surgery the patient is ambulating pain-free and without assistive
devices. Radiographs demonstrate a well-fixed triflange acetabular
component (Figure 6A-6C).
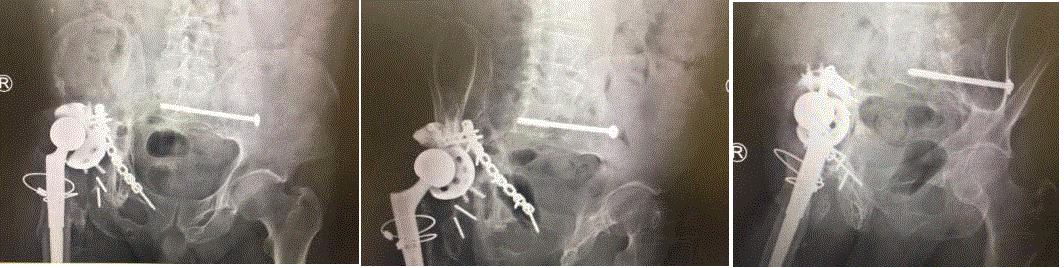
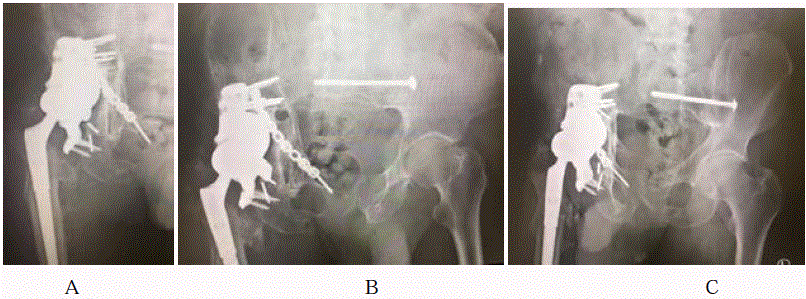
Figure 1
Figure 1
Antero Posterior (AP) (A) and Judet (B, C) views of the pelvis demonstrating gross loosening of the acetabular component. There is massive acetabular
bone loss involving the anterior and posterior columns.
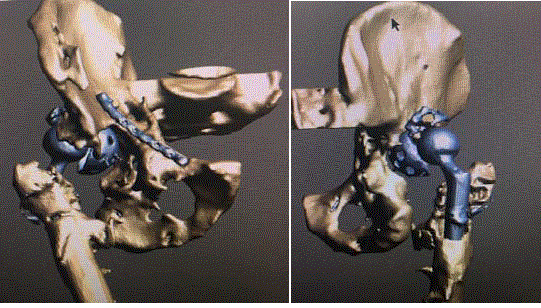
Figure 2
Figure 2
Anterior (A) and posterior (B) three-dimensional CT views of the pelvis demonstrating the loose acetabular cup and massive bone loss.
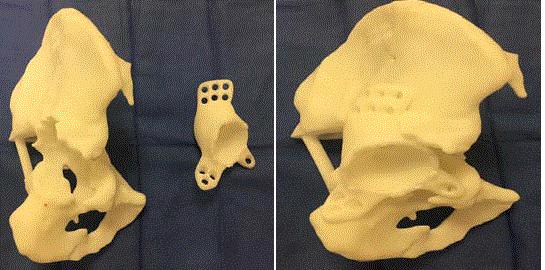
Figure 3
Figure 3
Plastic models of the patient’s pelvis and proposed Custom Triflange Acetabular Component (CTAC) based on thin cut CT scanning of the pelvis (A).
CTAC position when implanted into pelvis model.
Figure 4
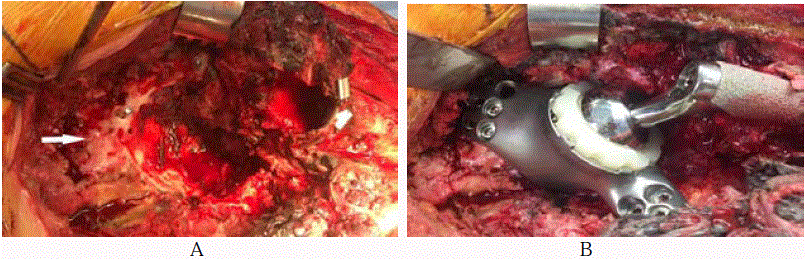
Figure 5
Figure 5
Intraoperative views demonstrating (A) preparation of the acetabulum for CTAC implantation (white arrow denotes supraacetabular bone; patient head
to the left of the image) and (B) the implanted CTAC.
Figure 6
Discussion
The case we have presented illustrates a very difficult
reconstruction challenge in revision joint replacement. Less degrees
of bone loss with intact acetabular columns may be managed with
cementless hemispheric cups and multiple screws with good results
[6,7]. However, the results of acetabular reconstruction with massive
bone loss (superior-medial hip center migration with non-supportive
anterior and posterior columns) are poor using conventional
techniques including cementless shells, augments; reinforcement
rings and cages [8-12]. For these Paprosky type IIIB hips, especially
those with a pelvic discontinuity, custom triflange acetabular
components [2-5,13-17] or cup-cage constructs [8,18-24], may
provide a more durable reconstruction.
Cup-cage constructs essentially involve the use of a cage to
protect a cup while bone in-growth between the cup and acetabulum
occurs. After bone grafting of acetabular defects, a highly porous cup
(Tantalum; Zimmer-Biomet, Warsaw, IN, USA) is placed into the
defect against bleeding host bone. Implant-bone contact is maximized
and the construct stabilized with as many screws as possible. A
reconstruction cage is fixed over the cup to protect it as it achieves
in-growth into the acetabulum. A polyethylene liner is cemented
into the cage in the appropriate version [8,19,21,22]. Amenabar et al. retrospectively reviewed 68 cup-cage reconstructions performed for
massive bone loss (corresponding to Paprosky type IIIA and IIIB).
Forty one hips (61%) have pelvic discontinuity. At a mean followup
of 68 months (range, 24 to 135 months), the revision rate of the
26 cup-cages performed in the absence of pelvic discontinuity was
8% (two of 26). Revisions were done for infection and instability.
At a mean follow-up of 77 months (range, 24 to 135 months) the 45
cup-cages used performed for the treatment of major bone loss with
pelvic discontinuity had a revision rate of 9% (four of 45). All four
revisions were performed for aseptic loosening, with failure occurring
at a mean of 42 months. Survivorship was 93% at five years and 83%
at ten years [18].
For Paprosky type IIIB bone loss, with or without pelvic
discontinuity, good early to midterm results have been obtained
with the CTAC [2,5,14,15]. Gladnick and colleagues retrospectively
reviewed 73 patients who underwent reconstruction using a CTAC
for Paprosky type IIIB defects. At a mean follow-up of 7.5 years
(range 5 to 12 years), 58 hips were intact. Fifteen hips (20.5%) were
indicated for revision for reasons including instability (6 hips) and
infection (8 hips) and aseptic loosening [1,14]. Berasi and colleagues
retrospectively reviewed 24 hips with Paprosky type IIIB bone loss
reconstructed using the CTAC. At a mean follow-up of 57 months
(range, 28 to 108 months), there were two infections resulting in
prosthetic failure. The remaining acetabular components were well
fixed. There were no dislocations. Harris hip scores improved from a
mean of 42 before surgery to 65 at final follow-up (p< 0.001) [2].
Acetabular revision with massive bone loss is complex surgeries
with limited options for stable reconstructions. Complications rates
are higher and survivorship is lower than that observed in lesser
degrees of bone loss where the acetabular columns are intact. For
this more complicated cohort, CTAC and cup cage reconstructions
provide good midterm outcomes with a reasonable complication rate.
Extended follow-up of these patients is needed to determine the long
term survivorship of these reconstructions.
References
- Abdel MP, Trousdale RT, Berry DJ. Pelvic discontinuity associated with total hip arthroplasty: Evaluation and management. J Am Acad Orthop Surg. 2017;25(5):330-8.
- Berasi CC, Berend KR, Adams JB, Ruh EL, Lombardi AV Jr. Are custom triflange acetabular components effective for reconstruction of catastrophic bone loss? Clin Orthop Relat Res. 2015;473(2):528-35.
- Christie MJ, Barrington SA, Brinson MF, Ruhling ME, DeBoer DK. Bridging massive acetabular defects with the triflange cup: 2- to 9-year results. Clin Orthop Relat Res. 2001(393):216-27.
- Goodman GP, Engh CA, Jr. The custom triflange cup: build it and they will come. Bone Joint J. 2016;98-B(1 Suppl A):68-72.
- Taunton MJ, Fehring TK, Edwards P, Bernasek T, Holt GE, Christie MJ. Pelvic discontinuity treated with custom triflange component: A reliable option. Clin Orthop Relat Res. 2012;470(2):428-34.
- Della Valle CJ, Shuaipaj T, Berger RA, Rosenberg AG, Shott S, Jacobs JJ, et al. Revision of the acetabular component without cement after total hip arthroplasty. A concise follow-up, at fifteen to nineteen years, of a previous report. J Bone Joint Surg Am. 2005;87(8):1795-800.
- Park DK, Della Valle CJ, Quigley L, Moric M, Rosenberg AG, Galante JO. Revision of the acetabular component without cement. A concise follow-up, at twenty to twenty-four years, of a previous report. J Bone Joint Surg Am. 2009;91(2):350-5.
- Issack PS. Use of porous tantalum for acetabular reconstruction in revision hip arthroplasty. J Bone Joint Surg Am. 2013;95(21):1981-7.
- Issack PS, Beksac B, Helfet DL, Buly RL, Sculco TP. Reconstruction of the failed acetabular component using cemented shells and impaction grafting in revision hip arthroplasty. Am J Orthop (Belle Mead NJ). 2008;37(10):510-2.
- Issack PS, Nousiainen M, Beksac B, Helfet DL, Sculco TP, Buly RL. Acetabular component revision in total hip arthroplasty. Part II: management of major bone loss and pelvic discontinuity. Am J Orthop (Belle Mead NJ). 2009;38(11):550-6.
- Issack PS, Nousiainen M, Beksac B, Helfet DL, Sculco TP, Buly RL. Acetabular component revision in total hip arthroplasty. Part I: cementless shells. Am J Orthop (Belle Mead NJ). 2009;38(10):509-14.
- Sheth NP, Nelson CL, Springer BD, Fehring TK, Paprosky WG. Acetabular bone loss in revision total hip arthroplasty: evaluation and management. J Am Acad Orthop Surg. 2013;21(3):128-39.
- Barlow BT, Oi KK, Lee YY, Carli AV, Choi DS, Bostrom MP. Outcomes of custom flange acetabular components in revision total hip arthroplasty and predictors of failure. J Arthroplasty. 2016;31(5):1057-64.
- Gladnick BP, Fehring KA, Odum SM, Christie MJ, DeBoer DK, Fehring TK. Midterm survivorship after revision total hip arthroplasty with a custom triflange acetabular component. J Arthroplasty. 2018;33(2):500-4.
- Hogan C, Ries M. Treatment of massive acetabular bone loss and pelvic discontinuity with a custom triflange component and ilio-sacral fixation based on preoperative CT templating. A report of 2 cases. Hip Int. 2015;25(6):585-8.
- Moore KD, McClenny MD, Wills BW. Custom triflange acetabular components for large acetabular defects: Minimum 10-year follow-up. Orthopedics. 2018;41(3):e316-20.
- Wind MA, Jr, Swank ML, Sorger JI. Short-term results of a custom triflange acetabular component for massive acetabular bone loss in revision THA. Orthopedics. 2013;36(3):e260-5.
- Amenabar T, Rahman WA, Hetaimish BM, Kuzyk PR, Safir OA, Gross AE. Promising mid-term results with a cup-cage construct for large acetabular defects and pelvic discontinuity. Clin Orthop Relat Res. 2016;474(2):408-14.
- Ballester Alfaro JJ, Sueiro Fernandez J. Trabecular Metal buttress augment and the trabecular metal cup-cage construct in revision hip arthroplasty for severe acetabular bone loss and pelvic discontinuity. Hip Int. 2010;20 Suppl 7:S119-27.
- Konan S, Duncan CP, Masri BA, Garbuz DS. The cup-cage reconstruction for pelvic discontinuity has encouraging patient satisfaction and functional outcome at median 6-year follow-up. Hip Int. 2017;27(5):509-13.
- Kosashvili Y, Backstein D, Safir O, Lakstein D, Gross AE. Acetabular revision using an anti-protrusion (ilio-ischial) cage and trabecular metal acetabular component for severe acetabular bone loss associated with pelvic discontinuity. J Bone Joint Surg Br. 2009;91(7):870-6.
- Makinen TJ, Kuzyk P, Safir OA, Backstein D, Gross AE. Role of cages in revision arthroplasty of the acetabulum. J Bone Joint Surg Am. 2016;98(3):233-42.
- Malhotra R, Kancherla R, Kumar V, Soral A. Trabecular metal acetabular revision system (cup-cage construct) to address the massive acetabular defects in revision arthroplasty. Indian J Orthop. 2012;46(4):483-6.
- Sculco PK, Ledford CK, Hanssen AD, Abdel MP, Lewallen DG. The evolution of the cup-cage technique for major acetabular defects: Full and half cup-cage reconstruction. J Bone Joint Surg Am. 2017;99(13):1104-10.