Case Report
A Very Rare Complication after Removal of Intrauterine Device: Multiple Intestinal Rupture
Özlem Kayacık Günday*
Department of Obstetrics and Gynecology, KTO Karatay University, Medicana Medical Faculty Hospital, Turkey
*Corresponding author: Özlem Kayacık Günday, Department of Obstetrics and Gynecology, KTO Karatay University, Medicana Medical Faculty Hospital, Konya, Turkey
Published: 22 Oct 2018
Cite this article as: Günday ÖK. A Very Rare Complication
after Removal of Intrauterine Device:
Multiple Intestinal Rupture. World J
Surg Surgical Res. 2018; 1: 1069.
Abstract
Intrauterine device, it may cause various Complications during and after insertion or removal. In this case report IUD.
Introduction
The use of Intrauterine Device (IUD) for birth control is increasing in women. This is because
IUD is an effective and reliable method. It is one of the most frequently used methods in our country.
Approximately 5.3% of the US is used by women [1].
IUD-induced uterine perforation is an extremely rare but very serious complication.
Asymptomatic pain, abnormal bleeding, bowel or bladder perforation, such as fistula formation can
cause a variety of complications.
In this case report, we wanted to refer to a patient who underwent intestinal perforation and
presented with acute abdomen and underwent successful surgical intervention while attempting to
remove IUD.
Case Presentation
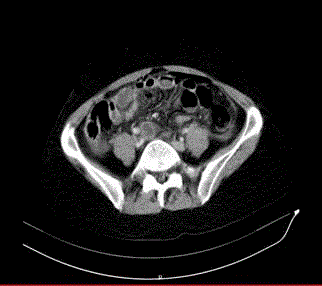
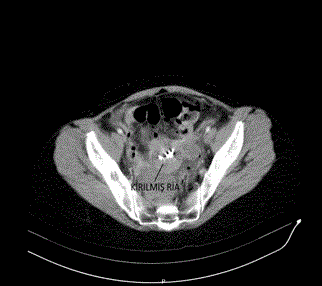
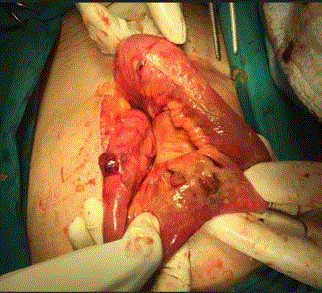
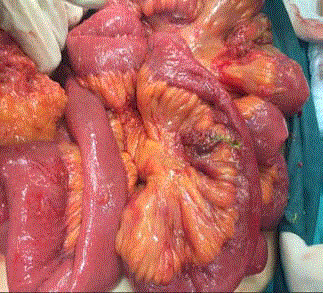
A 49-year-old female patient was admitted to our outpatient clinic with complaints of abdominal pain and nausea. The patient was informed that IUD was inserted for birth control 4 years ago and the patient was tried to remove the IUD at the external center before the procedure, but the procedure was unsuccessful. Physical examination did not show IUD. Menstrual spotting was present. There was rebaund and tenderness with deep palpation in the abdomen. Abdominal ultrasonography: 6 cm in the right ovary. Left ovary 2 cm. endometrioma was in the IUD cavity; pelvic fluid. There was a suspicion of uterine rupture. In the clinical follow-up of the patient, emergency abdominal tomography was performed because of worsening of general condition, increased pain and development of acute abdomen. Tomography; Common free air views adjacent to the anterior wall of the abdomen are monitored, free air fluid level around the liver. There are widespread free air views inside the abdomen and free fluid appearances (including air images). The free fluid appearance is more pronounced in the pelvic area, especially in the left parauterine level. In the foreground, perforation is considered. There is IUD in the endometrial cavity. Approximately 6.5 cm in the right adnexal area internal density was reported as increased cystic appearance (hemorrhagic cyst? and endometrioma?) (Figure 1,2). The patient underwent laparotomy with general surgery under emergency conditions. The abdomen was opened with six median incisions. It was seen that there was too much intestinal content in the abdomen. In the exploration, the ileocecal valve was approximately 60 cm. proximal to ileum, small intestinal wall, 2 close perforations were seen. In addition, approximately 150 cm distally from the treitzden again approximately 0.5 cm in the intestinal wall, perforation was observed (Figure 3). One piece of 0.5 cm hole in diameter (Figure 4), other bowel and colon segments were intact. Treitzden 150 cm the distal perforation was primary sutured with 3/0 silk. The perforated segment was removed from the left lower quadrant with a loop ileostomy and the perforation mouths were joined and the mouth was cut to the skin. After bleeding control, the floors were closed properly. The patient was transferred to general surgery for follow-up.
Discussion
We did not find any uterus and then multiple intestinal perforations after failed IUD removal.
In this respect, we think our case is different.
IUD is a reversible, long-acting, cost-effective method of birth
control [2]. Copper, silver, steel, such substances are available.
Although there is no consensus on the mechanism of action, it is
thought to affect fertilization and/or implantation by inflammation.
The incidence of uterine perforation due to the intrauterine
contraceptive device is estimated to be 1/1000 [2]. Risk factors for
uterine rupture have been reported as breastfeeding, postpartum,
uterine anomaly, adenomyosis and lack of experience of the wearer
[3-5]. It is usually recommended to wear it after the 6th month after
delivery [6]. Thinning of the postpartum uterus wall is the main
reason for this. In addition, the contractions in this period should
not be forgotten.
If intestinal perforation occurs after uterine perforation, the
perforation site is most frequently the small intestine, rectum and
sigmoid column. IUD may be partially or completely embedded
in the intestinal wall [7]. Perforation may be asymptomatic, or a
catastrophic result, such as an acute abdomen, may be encountered
in our case.
Lost IUD is understood by the absence of ropes. Ultrasonography
is the first choice in diagnosis. Easy, reliable and non-invasive also
allows us to understand whether the IUD is in the endometrial
cavity. In cases where IUD is not seen in the cavity, CT can benefit
from magnetic resonance imaging. As a very simple method, it can
be understood whether it is in the abdomen by direct abdominal
radiography. In addition, hysteroscopy is a safe, non-invasive,
effective and inexpensive diagnostic method in the removal of IUDs
that are not rope and embedded in the cavity [8,9].
Diagnosis should be treated with antibiotics to prevent pelvic
inflammation and should be removed. Lost IUDs should be removed
even if they are asymptomatic. Because of obstruction in the intestines,
adhesion, inflammation, perforation and pain in the organs of the
environment may be the cause.
In the treatment, colonoscopic, laparotomic or laparoscopic
methods can be used for the diagnosis and treatment of IUD and
its possible complications. But it is not suitable for every case. The
general condition of the patient, laboratory findings, hemodynamics
should be guiding. If there is sepsis and intestinal perforation,
laparotomy should be preferred. We also performed laparotomy in
order not to lose time because of the bad condition of our patient, the
development of acute abdomen findings and the suspicion of serious
bowel perforation. And after seeing the painting, we realized how
righteous we were.
As a result, although IUD removal is seen as a simple procedure,
it is appropriate to remove non-rope and intrauterine buried IUDs
with ultrasonography or hysteroscopy. Blindness interventions
during removal may cause IUD to break, exceed the myometrium
wall and cause damage to the surrounding organs. In cases where it
cannot be removed, close clinical follow-up and hysteroscopy should
be determined if necessary.
Figure 1
Figure 2
Figure 3
Figure 4
References
- United Nations. Population Division, Department of Economic and Social Affairs. World contraceptive use 2010.
- Peterson H, Curtic K, Meirk O, D’Arcargues C. Contraception. In: Scott JR, Gibbs RS, Karlan BY, Haney AF, editors. Danforth’s Obstetrics and Gynecology. 9th ed. Philadelphia: Lippincott Williams & Wilkins, 2003:541-61.
- Andersson K, Ryde-Blomqvist E, Lindell K, Odlind V, Milsom I. Perforation with intrauterine devices. Report from a Swedish survey. Contraception. 1998;57(4):251-5.
- Harrison-Woolrych M, Ashton J, Coulter D. Uterine perforation on intrauterine device insertion: is the incidence higher than previously reported? Contraception. 2003;67(1):53-6.
- Caliskan E, Oztürk N, Dilbaz BO, Dilbaz S. Analysis of risk factors associated with uterine perforation by intrauterine devices. Eur J Contracept Reprod Health Care. 2003;8(3):150-5.
- Heartwell SF, Schlesselman S. Risk of uterine perforation among users of intrauterine devices. Obstet Gynecol. 1983;61(1):31-6.
- Gill RS, Mok D, Hudson M, Shi X, Birch DW, Karmali S. Laparoscopic removal of an intra-abdominal intrauterine device: case and systematic review. Contraception. 2012;85(1):15-8.
- Fuentes JA, Hernández MA. Of office hysteroscopy for the removal of intrauterine device. Literature review. Ginecol Obstet Mex. 2009;77(4):197-201.
- Di Spiezio Sardo A, da Cunha Vieira M, Scognamiglio M, Zizolfi B, Nappi C, de Angelis C. The Challenging Intrauterine Contraceptive: In-office Hysteroscopic Approach. J Minim Invasive Gynecol. 2016;23(4):469.