Mini Review
Tips in Pancreatic Neuroendocrine Tumors (P-Nets)
Danilo Coco1* and Silvana Leanza2
1Department of General Surgery and Surgical Pathology, Augusto Murri Hospital, Italy
2Department of Surgery, Carlo Urbani Hospital, Italy
*Corresponding author: Danilo Coco, Department of General Surgery and Surgical Pathology, Augusto Murri Hospital, Italy
Published: 17 Sep,2018
Cite this article as: Coco D, Leanza S. Tips in Pancreatic
Neuroendocrine Tumors (P-Nets).
World J Surg Surgical Res. 2018; 1:
1059.
Abstract
A neuroendocrine tumor seems to arise from neural and endocrine cells. The most common are
carcinoid rumors and neuroendocrine tumors of the pancreas (P-NETs). Most pancreatic tumors
are sporadic but they also can arise from genetic syndrome such as MEN 1, MEN 2, VHL syndromes.
They account for approximately 1% of pancreatic cancer in a range of age between 30-60 years. They
can divide in Functional (F-PNETs) and non Functional tumors (NF-PNETs). Approximately 10%
to 20% is functional. Functuctional P-NET may or may not have hormonal syndrome based on
the hormone secretion: gastrin, insulin, glucagone, VIP, somatostatin. About 70% are insulinomas,
15% glucagonomas, 10% gastrinomas and somatostatinomas, which have a risk of metastases of
80% to 90%. Very rare is Vipomas, ACTHoma, GRFoma. Non functional PNET may have not
any kind of symptoms and they are discovered in advanced stage. Appropriate diagnosis requires
multidisciplinary team evaluating biochemical, radiological, endocrinological and surgical findings.
Pathogenesis
P-NETs have two probable origins of pancreatic NET: mature endocrine cells in the pancreas and multipotent stem cells. Ki-67 index, mitotic count and differentiation are the major components of P-NETs grading system (WHO) (Table 1)[1-4].
Biochemical, Clinical and Diagnostic Features
Insulinoma
It’s the most common P-NET. Betha cells. Hormon secretion: Insulin. It’s a benign type in
almost 80%. Hepatic metastases inferior of 5%. Clinical symptoms: hypoglycemic symptoms,
Whipple triad. Biochemical findings: Insulin level more than 3 mcLU/ml, C-peptide >0.6 ng/ml,
pro-insulin >5 pmol/L. Dinamic tests: Calcium injection (Imamura test).
Gastrinoma
G cells. Hormone: gastrin. Associated with MEN 1 in 70% of cases. Malignant. 80% risk of
distant metastases. Clinical symptoms: gastro-duodenal ulcers, dyspepsia, diarrhea (Zollinger-
Ellison syndrome). Diagnosis: EGDS with biopsy. Biochemical: gastrin levels. A combination of
fasting serum gastrin levels 10 times and gastric PH less 2 are diagnostic of gastrinoma. Dynamic
tests: secretin stimulation.M
Glucagonoma
Rare Malignant. 80% risk of metastase. Clinical signs: Recent-onset diabetes, cachexia, necrolytic
erythematous skin rush. Biochemical findings: elevated glucagone in blood.
VIPoma
D1 cells. Hormone: VIP.Very rare. Malignant 40% to 70%. WHDA syndrome o Verner-
Morrison syndrome. Clinical: watery diarrhea, Hypokaliemia, Dehydratation, Achlorhydria.
Biochemical: elevated VIP.
Somatostatinoma
Rare D cells. Hormone: somatostatin. Malignancy 70%. Clinically: diabetes mellitus,
cholelithiasis, diarrhea.
Diagnostic Evaluations
CT/MRI are the most common techniques for the diagnosis of pancreatic NET with a sensitivity and specificity >90%. CT/MRI can also be used for preoperative staging, follow-up and evaluation of treatment efficacy. EUS is a highly sensitive for small lesions with diameters from 0.3 cm to 0.5 cm. Somatostatin Recptors Scanner (SRS) can detect tiny primary lesions and distant metastases.PET may be suitable for the detection of poorly differentiated tumors. The role of serum tumor markers in diagnosing pancreatic NET is limited Tumor markers: Chromoganin A (CgA), synaptophysin and/or neuron-specific enolase (NSE).
Table 1
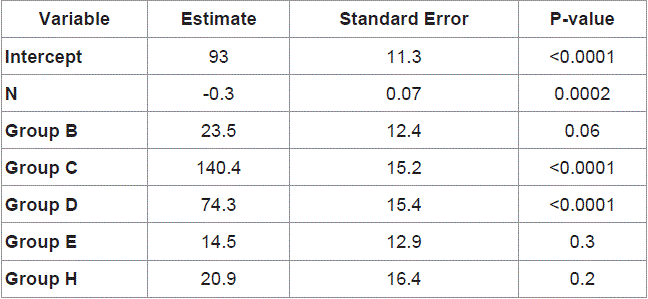
Table 2
Treatment
Surgical resection is the only curative strategy for pancreatic NET. 6 Furthermore, cytoreductive surgery can control the secretion of activated hormones and improve the survival for patients with advanced pancreatic NET and can be an optional strategy for physically fit patients with metastatic, well-differentiated pancreatic NET with an overall survival (OS) of 60 months versus 30 months in non cytoreductive or not fit patients. Somatostatin analogues or CHT are the first or second line approach in advanced diseases.
Conclusion
Pancreatic NET are a group with high heterogeneity and a
better prognosis than exocrine pancreatic cancer. The incidence of
pNETs is increasing and the majority of pNETs are nonfunctional.
The prognosis worsens in patients with metastatic tumors or
poorly differentiated pancreatic NET. Surgical treatment is the first choice treatment. Somatostatin analogue or cytotoxic CHT are the
alternative. The efficacy of sunitinib and everolimus support the
role of targeted agents as a new option in the first- or second-line
treatment of pancreatic NET.
Summary
Evaluate CgA, NSE, hormone features (Table 2), symptoms and signs, radiologic findings (CT, MRI, SRS, PET, EUS), decide after a multidisciplinary team planning, analyze histopathological findings (Ki-67, mitotic count, differentiation).
References
- NCCN. Neuroendocrine tumors. 2017.
- Öberg K, Knigge U, Kwekkeboom D, Perren A. Neuroendocrine gastro-entero-pancreatic tumors: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann of Oncol. 2012;23 Suppl 7:vii124-30.
- Zhou C, Zhang J, Zheng Y, Zhu Z. Pancreatic neuroendocrine tumors: a comprehensive review. Int J Cancer. 2012;131(5):1013-22.
- Jian Sun. Pancreatic neuroendocrine tumors. Intractable Rare Dis Res. 2017;6(1):21-8.