Research Article
Comparative Study of Standard Fundoplication (Nissen and Toupet) vs. Modified Toupet Fundoplication for GERD Repair
Mihael Sok1,2*, Boris Greif,1, Tomaž Štupnik1,2 and Matevž Srpčič1
1Department of Thoracic Surgery, University Medical Centre Ljubljana, Slovenia
2Department of Medicine, University of Ljubljana, Slovenia
*Corresponding author: Mihael Sok, Department of Thoracic Surgery, University Medical Center Ljubljana, Zaloškacesta 7, 1000 Ljubljana, Slovenia
Published: 17 Sep, 2018
Cite this article as: Sok M, Greif B, Štupnik T, Srpčič
M. Comparative Study of Standard
Fundoplication (Nissen and Toupet)
vs. Modified Toupet Fundoplication for
GERD Repair. World J Surg Surgical
Res. 2018; 1: 1056.
Abstract
Introduction: Failure following anti reflux surgery for GERD is reported from 3% to 30%,
predominantly from reflux recurrence. Modified Fundoplication follows the principles of standard
Nissen or Toupet Fundoplication. The difference is in the fixation of esophagogastric junction
intraabdominally, technically with two retro esophageal Fundo-crural muscle stitches and a
retroesophageal fundo- right crus stich. No stitches in the esophagus are used.
Aim: A comparative study of modified fundoplication vs. standard (Toupet or Nissen) fundoplication
was carried out.
Material and Methods: Patients with documented gastroesophageal reflux entered a prospective
nonrandomized, feasibility study. Patients who underwent a different type of operation were
comparable for age, gender, BMI, functional esophageal test before operation, number of hiatal
stitches, and hiatal hernia presence at operation and hospitalization time.
Aim: To compare modified Toupet with standard Fundoplication with respect to functional
postoperative results.
Results: A total of 70 patients, 42 female and 28 male patients, were operated on laparoscopically for
GERD. Standard Fundoplication was carried out in 61 patients and modified Toupet in 9 patients.
After 2-5 years of follow up 4(6%) patients from the standard Fundoplication group underwent re
operation, among them one for reflux recurrence. No patients from the modified Toupet group
needed repeat surgery. In the same postoperative period 37(69%) patients were without PPI from
the standard group in comparison to 6(75%) patients from the modified Toupet group.
Conclusion: The modified Toupet Fundoplication is technically simpler to perform, is not inferior
to standard Fundoplication and is feasible with promising results. The importance of GEJ fixation
to crural muscles and plastics of Gastroesophageal flap valve is discussed.
Keywords: Gastroesophageal reflux; Antireflux surgery; Reflux recurrence; Modified
Fundoplication
Introduction
In surgical therapy, despite clear operative principles, short and long-term failures following
Fundoplication for GERD still remain a serious problem. Failure following Antireflux surgery for
GERD is reported from 3% to 30%, predominantly from persistent or recurrent symptoms [1,2].
This variability may be explained by differences in the definition of failure from center to center.
Over the past 15 years, arrays of innovative surgical and endoscopic techniques have been
developed for the treatment of Gastroesophageal Reflux Disease (GERD) [3]. The basic operative
principles in GERD or Hiatus Hernia (HH) repair is Retro-esophageal cruroplasty and fixation of
the stomach within the abdomen, namely posterior attachment of the Esophagogastric Junction
(EGJ) [4-7]. The predominant operative approach for fixation at present appears to be laparoscopic
circumferential Fundoplication, such as the Nissen or Toupet procedures [8].
Some years ago at the demanding operation of a patient with recurrent HH an improvisation of
the Fundoplication was carried out as an exit from force. Only firm stitches of the Retroesophageal
gastric fundus to the crural muscles were made without fundus –esophagus stitches. After a good outcome, this simplified Fundoplication was taken into consideration.
This is 180° fundoplication and follows Toupet principles with some
modifications. Two big bite stitches are done posteriorly between the
gastric fundus in the retroesophageal position and crural muscles
medially as caudally as possible followed by one stitch between
the retroesophageal gastric fundus and right crus. No Esophagofundoplicate
stitches are made. The aim is solid fixation of the EGJ
and gastric fundus intra abdominally and reinforcement of potential
weak crural muscles with alive, vascularized tissue, namely the gastric
fundus. Simple modification was later recognized as a potential
and good approach for better laparoscopic fixation of EGJ intra
abdominally with anti-reflux power in patients with GERD and HH.
Aim: The aim of the study was to compare the feasibility and
late results of standard fundoplication namely Nissen or Toupet
fundoplication with the modified Toupet procedure. Postoperative
course and postoperative results 2-5 years after operation were
registered. Postoperative reflux recurrence rate and dysphagia were
the primary endpoints of the study.
Table 1
Table 2
Methods and Materials
From January 2012 to January 2014, a prospective nonrandomized
study of consecutive patients undergoing operations for GERD
was made at a single tertiary institution. The indication for surgical
treatment of GERD was documented Gastroesophageal re flux that
persisted despite maximal medical therapy, patient's preference, extra
esophageal manifestations and GERD related esophageal injury.
Patients were without previous or present dysphagia and without
esophageal stenosis. 24-hr pH monitoring was performed selectively
in patients with extraesophageal symptoms and in those without
erosive esophagitis. Manometer was also selectively carried out. BMI
of the patients was calculated. Optimal data for specific analysis was
eligible for 70 patients and these patients entered the study. The hiatus
hernia was registered at laparoscopy but the size of the hernia was not
measured in cm, but rather with the number of stitches for crural
closure as the indirect measure of the hernia size. After the procedure,
all patients were monitored in the recovery room of the operating
unit for two hours and then transferred to the intensive care unit.
On the first postoperative day contrast examination of the esophagus
was performed and patients began to consume liquids. The patients
were discharged as soon as they were able to consume mixed food,
when the postoperative pain was well controlled by oral analgesics,
and if there were no other conditions or complications requiring a
prolonged hospital stay.
Patients who underwent a different type of operation were
comparable for age, gender, BMI, functional esophageal test before
operation, number of hiatal stitches, and hiatal hernia presence at
operation and hospitalization time. Patients were followed from 2 to
5 years. PPI consumption, reflux recurrence, dysphagia and hiatus
hernia advent were registered.
Surgery
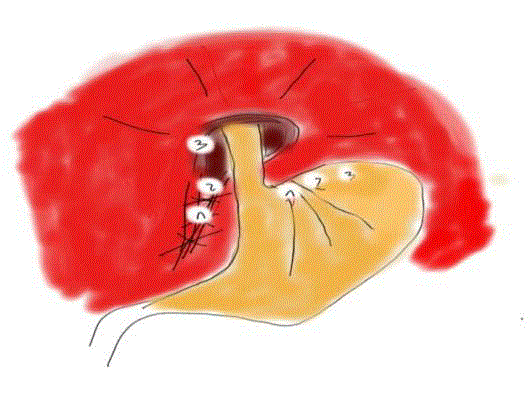
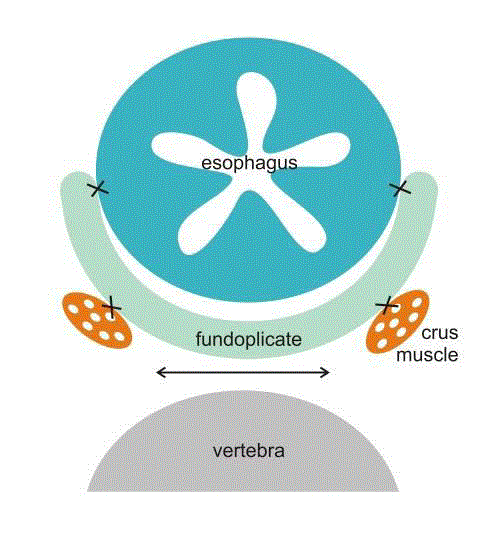
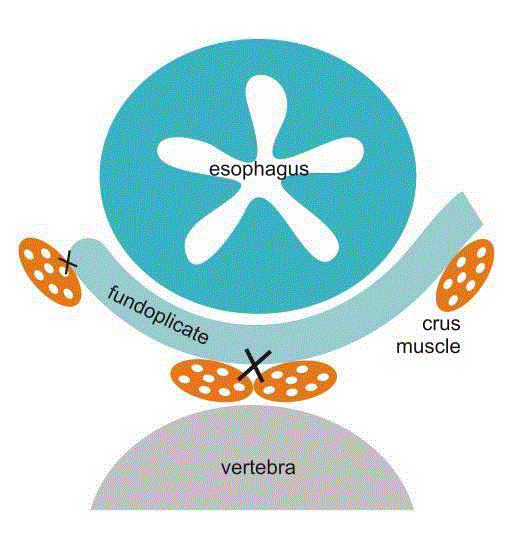
Antireflux operation was performed following the standard technique: laparoscopy, resection of the hernia sack from the mediastinum but not from the abdomen, if present, elevation of the EGJ with retroesophageal window creation and cruroplasty with Teflon pledges. Then fundoplication followed: either the Nissen or Toupet fundoplication as the standard fundoplication or modified Toupet fundoplication. Modified Toupet was carried out using two firm big bite retroesophageal fundo-crural stitches, the first approximately 1 cm from the angle of Hiss on the anterior aspect of the gastric fundus to the crural muscle medially as caudally as possible where hiatus stitches were already in place. The second retroesophageal fundo-crural stitch was made about 2 cm cranially. The distance between the first and second stitches was the size of an open standard grasper jaw. The third big bite stitch was a regular Toupet retroesophageal fundus- right diaphragmatic crus stitch (Figure 1). The logic behind this method was that these stitches would create a fundoplication-like effect to control reflux and intra abdominal EGJ fixation, obliteration of the retroesophageal or retrofundal space, stable tamponation of the hiatus region and possible adhesion formation of the crural region and reinforcement of the hiatal muscle with vital tissue, namely the gastric fundus. Figures 2 and 3 show a schematic representation of the Toupet and modified Toupet procedures. All operations were performed without bougie, without dissection of the gastric short vessels, without the Collis procedure and without mesh. All patients were operated on under the same conditions and by the same surgical team, using the same brand of laparoscopic instruments, with an abdominal CO2 in sufflation pressure of 15 mmHg. Modified fundoplication was made by one surgeon and was not selected randomly.
Figure 1
Figure 2
Figure 2
Schematical representation of Toupet fundoplication with potential forces (↔) from intraabdominal tissue that can spread crural muscles and place where intra abdomilal tissue can enter.
Statistics
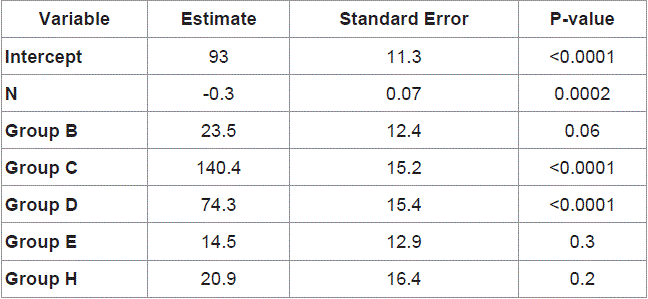
Data were analyzed using the Statistical Package for Social Sciences version 16.0 for Windows (SPSS, Chicago, IL) software. Categorical variables were tested for associations using a χ2 test. The descriptive data were expressed as a mean and range. For the normally distributed variables, at-test was used. The Sperm and Rho association test was used to measure the relationship between two variables. A p-value of < 0.05 was considered statistically significant.
Results
A total of 70 patients participated in the study, of which 42
were female and 28 were male. Standard (Toupet or Nisssen)
fundoplication was carried out in 61 patients and the modified Toupet
in 9 patients. All patients were operated upon laparoscopically. In
the standard fundoplication and modified Toupet the mean age of
patients was 48.5 and 46.7 years, mean BMI was 27.6 and 27.0 kg/m2,
mean number of stitches was 2.7 and 2.2, mean hospitalization time
was 2.1 and 2.6 days and mean DeMeester score was 25.1 and 17.3
respectively. At operation hiatal hernia or at list dilatated hiatus was
registered in 30 and 3 patients in the standard and modified Toupet
groups respectively (Table 1). The differences were not significant.
After 2-5 years of follow up problems were registered and are
shown in Table 2. Four patients from the standard group needed
reoperation: dysphagia - two patients, reflux - one patient and
symptomatic hiatus hernia - one patient. In the modified group no
patients needed reoperation. In the same period in the standard group
9 patients took a PPI regularly and 7 on demand (31%) in comparison
with 1 patient who took a PPI regularly and 1 who took a PPI on
demand (25%) in modified the Toupet group. These differences were
not significant.
Figure 3
Discussion
After the first description of the 360° esophagogastric
fundoplication in 1956, the Nissen fundoplication surgery
armamentarium has changed little until now. All is about
fundoplication to augment the Lower Esophageal Sphincter (LES).
Some modifications are described with the intention to improve
upon postoperative complications, late results, cost of the operation
and postoperative quality of life. The operation should be safe for the
patient, cost-effective and complications free [9-13].
According to the literature the failure rate of open or laparoscopic
approaches ranges from 3% to 30% [1,2]. In our study failure that
needed reoperation was registered in 4(6%) patients, two for dysphagia,
one for severe reflux and gas bloat and one for hiatus hernia. All reoperated
patients were from the standard fundoplication group (7%).
No patients in the modified Toupet group needed reoperation.
From the patients that presented for follow-up 2-5 years after
operation we found that 37(69%) patients from the standard
fundoplication group did not require antireflux medication in
comparison to 6(75%) patients in the modified Toupet group. It was
a short period as recurrences can happen later. According to some
reports more than 5 years after the surgery, only 38% of patients
were without anti-reflux medications regularly [14]. Recent reports have criticized the Toupet procedure as having a higher long-term
failure rate than the Nissen approach, especially for patients with
severe GERD forms [15]. On the other hand Toupet fundoplication
should be considered in redo interventions for patients who initially
underwent Nissen fundoplication [16].
Some positive effect on reflux control of the modified Toupet
can be speculated on the basis of the Gastroesophageal Flap Valve
(GEFV) function. The exact means by which fundoplication controls
gastroesophageal reflux is still a matter of debate. It is often assumed
that reflux is controlled by increased resting Lower Esophageal
Sphinter (LES) pressure and intra-abdominal length of the esophagus.
However, there are several studies that show that the resting pressure
does not always increase after fundoplication and that in the majority
of such cases reflux is perfectly controlled. Resting LES pressure may
even decrease as the intra-abdominal length of the esophagus [17].
GEFV was established as an important component in the anti-reflux
barrier [18]. Three distinct anatomic structures, the clasp and sling
muscle fibers, crural diaphragm and LES were identified to form
the antireflux barrier [19,20]. Miller et al. [21] report that the basic
principle of the most usual antireflux surgeries e.g. Nissen and Toupet
is retroesophageal fundus extra position. The angle of his is changed
and the gastric oblique muscle of the fundus is strained. It was shown
that Nissen fundoplication prevents reflux by artificially bolstering
the area of the defective gastric sling fiber/clasp fiber complex and
is an important factor in generating the antireflux barrier [22]. Later
on it was discovered that the gastric sling fiber/clasp fiber complex
is not present in patients with GERD, suggesting that GERD may
be a pathophysiologic defect within the gastric clasp/sling smooth
muscle fiber complex [23]. The modified Toupet technique, like the
standard technique, involves fundus retroesophageal extra position
and has the potential to influence GEFV. Hill repair is the only known
repair done on firm anchoring of EGJ within the abdominal cavity
and accentuating the flap valve [24]. We believe that fundo-crual
stitches in the modified Toupet have the same power. Further studies
are needed to confirm this statement. The angel of He was pointed to
as important objective in the WTP procedure [13].
Two patients from the standard fundoplication group required
reoperation for persistent dysphagia. The reason is likely that bougie
was not used. Sages recommend the use of an esophageal dilator but
use should be weighed against the risk of esophageal injury [25]. In
the past we perfomed bougie but after two consecutive intraoperative
perforations we decided to stop using the bouginage. We believe that
the reasons behind the problem involved the organization of the
team, as there was a high turnover of members in the team responsible
for bougie replacement in our tertiary center. We routinely used
an esophageal dilator twice, first for hiatus closure and second for
fundoplication formation with twice the risk for perforation. Today
we prefer to use the Toupet operation, short floppy Nissen and dissent
hiatus opening around the esophagus.
One patient underwent reoperation for hernia recurrence from
the standard fundoplication group. This patient had a hiatus hernia
intraoperatively and a sliding hernia on a barium study preoperatively.
Discussion
To summarize, some advantages of the modified Toupet
180° fundoplication are no esophago-fundoplicate sutures, no
intraoperative bouginage, no short gastric artery resection, no
possibility of sleep Nissen or malposition of the wrap. It is also
technically simpler to perform. The basic idea is to fix ERJ intra
abdominally, to obliterate retroesophageal and retrofundal space,
to tamponate crural region with fundus, to advance adhesion
formation in the hiatus region, to reinforce hiatal muscle by vital
tissue and to support the antireflux barrier affecting GEFV. It appears
to be a promising alternative and affair compromise to other wellestablished
antireflux operations. This study shows that the modified
Toupet fundoplication is not inferior to standard fundoplication. The
modification is safe for the patient. Further studies are needed for
objectivation of these speculations.
The limitations of the study include the small sample size
of comparable patients, non-randomized study, single surgeon
experience and short postoperative follow up.
References
- Soper NJ, Dunnegan D. Anatomic fundoplication failure after laparoscopic antireflux surgery. Ann Surg. 1999;229(5):669-76.
- Watson DI, de Beaux AC. Complications of laparoscopic antireflux surgery. Surg Endosc. 2001;15(4):344-52.
- Ganz RA. A Review of new surgical and endoscopic therapies for gastroesophageal reflux disease. Gastroenterol Hepatol (NY). 2016;12(7):424-31.
- Naunheim KS, Edwards M. Paraesophageal hiatal herna. In: General thoracic surgery. Shilds TW, Locicero J III, Reed CE, editors. Lippincott Williams & Wilkins, Philadelphia, PA,USA. 2009;951-9.
- Mori T, Nagao G, Sugiyama M. Paraesophageal hernia repair. Ann Thorac Cardiovasc Surg. 2012;18:297-305.
- Morse C, Pennathur A, Luketich JD. Laparoscopic techniques in reoperation for failed antireflux repairs. In: Pearson's Thoracic and Esophageal Surgery. 3rd ed. Patterson GA, Pearson FG, Cooper JD, editors. Churchill Livingstone, Philadelphia, PA, USA. 2008;367–75.
- Huang J, Low D. Hill repair. In: Esophageal Surgery. Pearson FG, Cooper JD, Deslauriers J, editors. Churchill Livingstone, Philadelphia, PA, USA. 2008;288–97.
- Allen MS, Trastek VF, Deschamps C, Pairolero PC. Intrathoracic stomach. Presentation and results of operation. J Thorac Cardiovasc Surg. 1993;105(2):253-8.
- Castelijns PSS, van de Poll MCG, Smulders JF. A modified technique to Create a standardized floppy Nissen fundoplication without a bougie. J Laparoendosc Adv Surg Tech A. 2018;28(7):853-8.
- Lukish J, Pryor H, Rhee D, Salazar J, Goldstein S, Gause C, et al. A novel continuous stitch fundoplication utilizing knotless barbed suture in children with gastroesophageal reflux disease: a pilot study. J Pediatr Surg. 2015;50(2):272-4.
- Shapey IM, Agrawal S, Peacock A, Super P. A prospective cross-sectional study of laparoscopic subtotal Lind fundoplication for gastro-oesophagealreflux disease--a durable and effective anti-reflux procedure. Int J Surg. 2015;13:257-60.
- Smith CD, DeVault KR, Buchanan M. Introduction of mechanical sphincter augmentation for gastroesophageal reflux disease into practice: early clinical outcomes and keys to successful adoption. J Am Coll Surg. 2014;218(4):776-81.
- Wróblewski T, Kobryn K, Nowosad M. Surgical treatment of GERD. Comparative study of WTP vs. Toupet fundoplication - results of 151 consecutive cases. Video surgery Miniinv. 2016;11(2):60-6.
- Hatch KF, Daily MF, Christensen BJ, Glasgow RE. Failed fundoplications. Am J Surg. 2004;188:786-91.
- Erenoğlu C, Miller A, Schirmer B. Laparoscopic Toupet versus Nissen fundoplication for the treatment of gastroesophageal reflux disease. IntSurg. 2003;88(4):219-25.
- Al Hashmi AW, Pineton de Chambrun G, Souche R, Bertrand M, De Blasi V, Jacques E, et al. A retrospective multicenter analysis on redo-laparoscopic anti-reflux surgery: conservative or conversion fundoplication? Surg Endosc. 2018.
- Bancewicz J, Mughal M, Marples M. The lower oesophageal sphincter after floppy Nissen fundoplication.Br J Surg. 1987;74(3):162-4.
- Hill LD, Kozarek RA, Kraemer SJ, Aye RW, Mercer CD, Low DE, et al. The gastroesophageal flap valve: in vitro and in vivo observations. Gastrointest Endosc. 1996;44(5):541-7.
- Mittal RK, Balaban DH. The esophagogastric junction. N Engl J Med. 1997;336:924-32.
- Miller LS, James B, Ulerich R. A new theory to explain the pathophysiology of GERD. Gastroenterology. 2004;126:A503-T1741.
- Miller L, Clavé P, Farré R, Lecea B, Ruggieri MR, Ouyang A, et al. Physiology of the upper segment, body, and lower segment of the esophagus. Ann N Y Acad Sci. 2013;1300:261-77.
- Dai Q, Chung CY, Nowrouzzadeh F. Simultaneous ultrasound and manometry in the evaluation of Nissen fundoplication. Gastroenterology. 2003;124:A418-M2113.
- Miller L, Dai Q, Vegesna A, Korimilli A, Ulerich R, Schiffner B, et al. A missing sphincteric component of the gastro-oesophageal junction in patients with GORD. Neurogastroenterol Motil. 2009;21(18):813-e52.
- Huang J, Low D. Hill repair. In: Pearson FG, Cooper JD, Deslauriers J, editors. Esophageal Surgery. New York: Churchill Livingstone; 2007:288–97.