Research Article
Pseudomyxoma Peritonei with Metastatic Ovarian Tumor in a 28-Years-Old Patient: A Case Report with Review of the Literature
Hanane Ziadeh1*, Jessica Clerc2, Damien Brieux2, Aude Van-Nieuwenhuyse2 and Jean-Robert
Lambert2
1Department of Obstetrics and Gynecology, Holy Spirit University of Kaslik, Lebanon
2Department of Obstetrics and Gynecology, Centre Hospitalier de Bourg-en-Bresse, France
*Corresponding author: Hanane Ziadeh, Department of Obstetrics and Gynecology, Holy Spirit University of Kaslik, Lebanon
Published: 17 Sep, 2018
Cite this article as: Ziadeh H, Clerc J, Brieux D, Van-
Nieuwenhuyse A, Lambert J-R.
Pseudomyxoma Peritonei with
Metastatic Ovarian Tumor in a
28-Years-Old Patient: A Case Report
with Review of the Literature. World J
Surg Surgical Res. 2018; 1: 1055.
Abstract
Pseudo Myxoma Peritonei (PMP) or gelatinous disease of the peritoneum is a very rare tumor that
originates from a ruptured appendiceal mucocele in the abdomen. Other uncommon origins are
described in the literature like ovaries and peritoneum. Although the condition occurs in both sexes,
but it affects especially women between the age of 50 and 70. We hereby report the case of a 28
years old French woman diagnosed with a suspicious solid ovarian mass of 62.8 mm × 99.7 mm,
associated with peritoneal effusion. The patient underwent one week later a diagnostic laparoscopy
with left salpingo-oophorectomy revealing a left ovarian tumor of 10 cm associated with diffuse
gelatinous ascite. The microscopic exam of the tumour showed a low-grade metastatic ovarian
mucinous carcinoma associated with a pseudomyxoma peritonei with the appendix being the most
probable origin.
Keywords: Appendix; Pseudomyxoma peritonei; Ovarian cancer
Introduction
Pseudo Myxoma Peritonei (PMP) is a very rare neoplasm, with poor prognosis. There is only 45 cases reported in the English Literature and it is known to affect 2/1000000 persons per year [1,2]. The course of the disease is characterized by the production of mucine into the abdomen leading to a gelatinous obstructive ascite or what it is called “jelly belly’’ appearances [1]. PMP has different origins: more than 80% arises from the appendix. However, Primary ovarian mucinous carcinoma presenting as PMP has been reported too [2,3], with a low stage and low grade at time of diagnosis in the majority of women. PMP has a protracted therapeutic pathway with combined repeated cytoreductive surgeries and Intra Peritoneal Chemotherapy (IPC) [4,5]. Below, we report an extremely rare case of a 28 year-old woman who developed a Pseudomyxoma peritonei originated from the appendix with an ovarian metastasic tumor.
Case Presentation
A 28 years old nulliparous woman presented to the Emergency Room for persistent diffuse pelvic
pain Ten days after sexual intercourse. There is no previous personal medical or gynaecological
history. She noted two diarrheal episodes that day with pollakiuria. The transvaginal ultrasound
showed a left atypical solid ovarian mass of 62.8 mm × 99.7 mm, with heterogeneous peritoneal
effusion. A pelvic MRI and tumor markers were ordered showing a slight increase of CEA, normal
Ca 19-9, Ca 125 and Inhibin B with a primitive left septated ovarian mass suspicious of malignancy
with peritoneal and pelvic effusion (Figure1).
A exploratory laparoscopy was done one week later revealing a peritoneal cavity filled with 400
ml of a viscous substance similar to gelatin with a left ovarian tumor of 10 cm (Figure 2 and 3). A
left salpingo-oophorectomy was done; the appendix was not seen due to its retrocecal position and
the inflammatory magma over it. The histopathological examination of the tumour reported a lowgrade
metastatic ovarian mucinous carcinoma associated with a pseudomyxoma peritonei most
probably originating from the appendix. Later on, an immunohistochemical study revealed a strong
expression of CK20 and absence of CK7. The patient is actually undergoing a cycle of hormone
stimulation followed by a cryopreservation of her oocytes. Then in a second time, a cytoreductive
surgery and a Hyperthermic Intraperitoneal Chemotherapy (HIPEC) will be done.
Figure 1
Figure 1
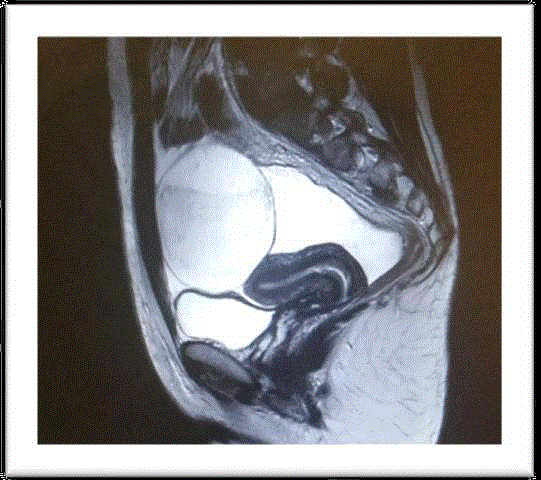
Pelvic MRI: Sagittal T2-weighted image, showing an intraperitoneal
tumor with tissular and cystic signal. The tumor is separated from the uterus
and surrounded by pelvic effusion.
Figure 2
Discussion
Pseudo Myxoma Peritonei (PMP) is a very rare entity consisting
of gelatinous ascites due to the implantation of mucine on the
peritoneal surfaces. In 1842, the disease was thought to originate
from the ovaries when Rokitansky and then Cruveilhier were the first
to describe a gelatinous degeneration in the peritoneal cavity [6]. In
1871, the disease was qualified by Pean as “gelatinous disease of the
peritoneum” [6]. Then, in 1884, Werth described the rupture of an
ovarian cyst with a gelatinous product [6], followed by Frankel on
1901 who mentioned a rupture of an appendicular tumor [6].
Pseudo Myxoma Peritonei (PMP) has an incidence of 2/1000000/
year. Usually, the main cause is an appendicular mucocele with other
rare primary sites have been also reported in the literature like the
ovaries, uterus, urachus, colon, stomach, pancreas and common bile
duct [1,7]. The disease is found more frequently in women than man
(male: female ratio=9:11) and affects the female in general after age of
50 [7]. There are no reported cases of PMP during twenties, making
our case the first in the literature to describe the occurrence of the
disease at this age [1].
The path physiology of the disease is explained by the
hypersecretion of mucine that leads to an overdistention of the
appendix followed by a rupture and dissemination of the mucus to
the whole abdominal cavity [8].
Furthermore, studies have shown that multiple enteric bacteria
play an important role in the progression of the disease (MUC2 and
MUC5AC expression in disseminated peritoneal adenomucinosis
and peritoneal mucinous carcinomatosis) [9,10]. The gelatin adheres
to all the organs covered by the parietal peritoneum especially the
omentum as shown in our case, making the surgical treatment very
aggressive.
There is no pathognomonic sign for the diagnosis of PMP, but
symptoms are variant and goes from a simple abdominal pain and
transit disorders as seen in our patient’ case, to signs of subocclusion.
The imagery (endovaginal ultrasounds, RMI, and TDM) and
exploratory laparoscopy stays the gold standard for the diagnosis of
PMP as seen in the published literature.
Tumor markers (CEA, CA19.9, CA125) are not useful for the
diagnosis of the disease. In our case, all the tumor makers were
normal except of the CA125 that was slightly increased and was not
specific also.
The mainstay of the treatment is cytoreductive surgery and
Hyperthermic Intraperitoneal Chemotherapy (HIPEC). The surgical
approach depends on the size of the lesions. But laparotomy remains
the preferred method. During the operation, the appendix must
obligatorily be removed; sometimes even a right hemicolectomy and
hysterectomy with bilateral adnexectomy can be performed.
The prognosis is really improved by the IPC and more recently,
doctors in specialized centers resort to the Pressurized Intraperitoneal
Aerosol Chemotherapy (PIPAC) to defeat the pharmacokinetic
limitations of intraperitoneal chemotherapy. Studies have shown that
the pressured aerosol increases the drug uptake by the tumor cells
with fewer complications compared to the use of IPC [11,12].
The recurrence rate of the disease is very high because the removal
of the entire peritoneum and all the mesos is really impossible. The
disease remains microscopic and no exam can detect a peritoneal
lesion pre and post operatively. Tumor blood markers are ineffective
and do not evaluate the chemotherapy efficiency. Reported cases
showed a morbidity rate of 24% while the mortality is estimated at
2% [13,14].
Figure 3
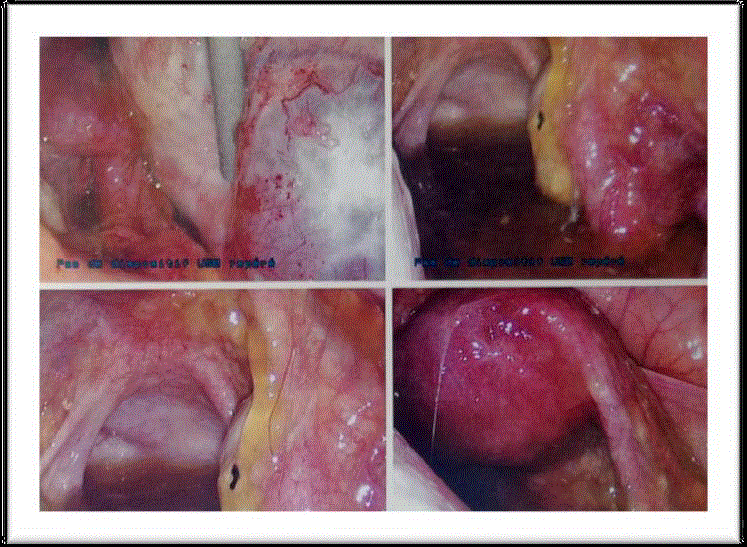
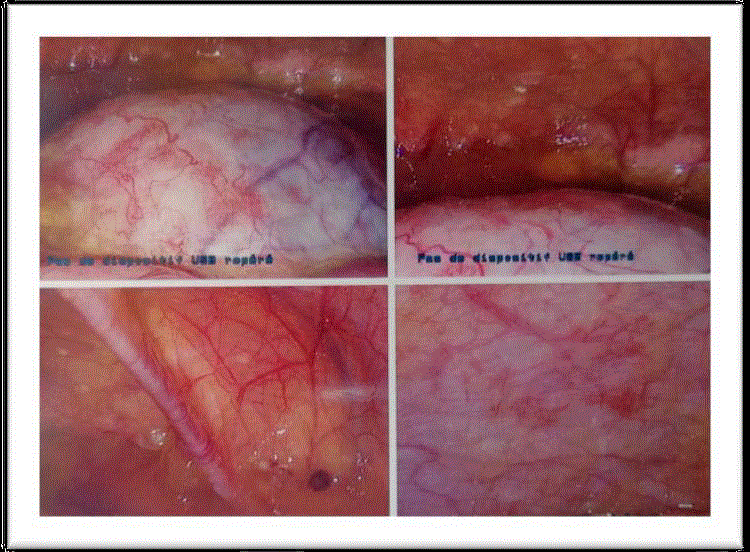
Figure 3
Intraoperative findings showing the left ovarian tumor with the
diffuse gelatinous ascite around.
Conclusion
Pseudo Myxoma Peritonei (PMP) is a very rare condition. The definitive diagnosis relies on laparoscopic findings combined with histopathology and immunochemical exam. As revealed in the few published cases and recently in our case, the disease can affect woman at any age. Consequently, PMP should be considered as a differential diagnosis in any female presenting with an ovarian tumor suspicious for malignancy associated with peritoneal effusion.
References
- Diaz-Zorrilla C, Ramos-De la Medina A, Grube-Pagola P, Ramirez-Gutierrez de Velasco A. Pseudomyxoma extraperitonei: A rare presentation of a rare tumour. BMJ Case Reports. 2013;4.
- Smeenk RM, van Velthuysen ML, Verwaal VJ, Zoetmulder FA. Appendicealneoplasms and pseudomyxoma peritonei: a population based study. Eur J Surg Oncol. 2008:34(2);196-201.
- Buell-Gutbrod R, Gwin K. Pathologic diagnosis, origin, and natural history of pseudomyxoma peritonei. Am Soc Clin Oncol Educ. 2013:221-5.
- Leen SL, Singh N. Pathology of primary and metastatic mucinous ovarian neoplasms. J Clin Pathol. 2012:65(7);591-5.
- Varona JF, Guerra JM, Salamanca J, Colina F, Lopez G, Morales M. Pseudomyxoma peritonei: a clinicopathologic analysis and follow-up of 21 patients. Hepatogastroenterology. 2005:52(63);812-6.
- Zeraidi N, Chahtane A, Lakhdar A, Khabouz S, Berrada R, Rhrab B, et al. La maladie gélatineuse du péritoine à propos d’un cas: médecine du Maghreb. 1996;59:34-6.
- Ioannidis O, Cheva A, Paraskevas G, Papadimitriou N, Konstantara A, Chatzopoulos S, et al. Pseudomyxoma retroperitonei: report of 2 cases and review of literature. Rev Esp Enferm Dig. 2012;104:268-75.
- Fairise A, Barbary C, Derelle AL, Tissier S, Granger P, Marchal F, et al. Mucocele of the appendix and pseudomyxoma peritonei. Journal de radiologie. 2008;89(6):751-62.
- Semino-Mora C, Liu H, Macavoy T, Nieroda C, Studeman K, Sardi A, et al. Pseudomyxoma peritonei: is disease progression related to micro-bial agents? A study of bacteria, MUC2 and MUC5AC expression in disseminated peritonel adenomucinosis and peritoneal mucinous carcino-matosis. Ann Surg Oncol. 2008;15(5):1414-23.
- O’Connell JT, Hacker CM, Barsky SH. MUC2 is a molecular marker for pseudomyxoma peritonei. Mod Pathol. 2002;15:958-72.
- Dedrick RL, Flessner MF. Pharmacokinetic problems in peritoneal drug administration: tissue penetration and surface exposure. J Natl Cancer Inst.1997;89(7):480-7.
- Hubner M, Teixeira H, Boussaha T, Cachemaille M, Lehmann K, Demartines N. PIPAC- Chimiothérapie intrapéritonéale vaporisée. Un traitement innovateur de la carcinose péritonéale. Rev Med Suisse. 2015;11:1325-30.
- Chua TC, Moran BJ, Sugarbaker PH, Levine EA, Glehen O, Gilly FN, et al. Early and long- term outcome data of patients with pseudomyxoma peritonei from appendiceal origin treated by a strategy of cytoreductive surgery and hyperthermic intraperitoneal chemotherapy. J Clin Oncol. 2012;30:2449-56.
- Yan TD, Bjelic L, Sugarbaker PH. Critical analysis of treatment failure after complete cytoreductive surgery and perioperative intraperitoneal chemotherapy for peritoneal dissemination from appendicular mucinous neoplasms. Ann Surg Oncol. 2007;14(8):2289-99.