Research Article
Elective vs. Emergency Stoma Surgery Outcomes
Adnan Qureshi1*, Joanne Cunningham2 and Anil Hemandas3
1Department of Surgery, Northampton General Hospital, UK
2Department of Cellular Pathology, Milton Keynes University Hospital, UK
3Department of General Surgery, Keynes University Hospital, UK
*Corresponding author: Adnan Qureshi, Department of Surgery, Northampton General Hospital, NN1 5BD, UK
Published: 27 Aug, 2018
Cite this article as: Qureshi A, Cunningham J, Hemandas
A. Elective vs. Emergency Stoma
Surgery Outcomes. World J Surg
Surgical Res. 2018; 1: 1050.
Abstract
Aim: The aim of this study was to compare general and stoma specific complications in patients
having stoma surgery in either an emergency or elective setting during their index hospital
admission.
Method: We retrospectively analysed data for all stomas created over the last three years in Milton
Keynes University Hospital. This covered the period from January 2013 to January 2016. A full
electronic record of patient’s kept by stoma department was used besides demography we analysed
the type of stoma i.e. colostomy or ileostomy, indications for the stoma, most common operation,
Length of Stay (LOS) and short term complications based on the Clavien-Dindo classification and
long term complication on one year follow-up.
We compared stoma specific complications, in emergency and elective cohort.
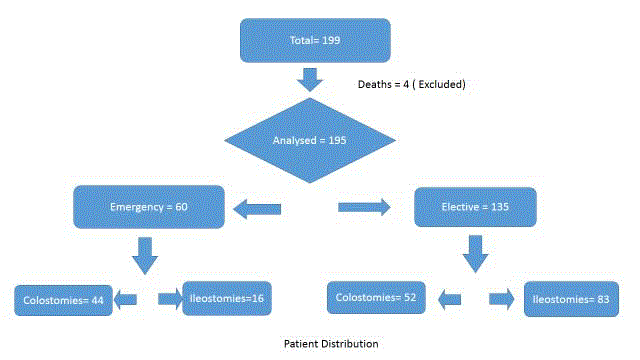
Results: A total of 199 patients had new ostomies created during the three year period. Four patients
died during the inpatient stay and these were excluded from the analysis. The total number of stomas
created in emergency were 60 and 135 stomas were elective procedures. The male to female ratio was
1:1.01. The average age for the emergency cohort was 6 years older than for the elective cohort. There
was statistically significant difference in length of stay between two cohorts. The rate of grade 3 or 4
complications higher in the emergency cohort of patients. Long term complication was also high in
patients operated in emergency i.e. 48% compared to 25% for elective patients. Most common long
term complication in emergency stoma was parastomal hernia.
Conclusion: Emergency surgery procedures are frequently bowel related. Since the introduction of
consultant lead services in UK the outcomes have improved significantly. Similarly we recommend
any bowel surgery involving stoma should be done under direct supervision of consultant surgeons
to improve long term outcomes.
Keywords: Parastomal hernia; Stoma surgery; Ileostomy; Ostomies
Introduction
The first deliberate surgical creation of a stoma was in the early 18th century when a stoma was
created to divert faecal material in anal agenesis. However, it wasn’t until the twentieth century,
towards the end of the world war one when this became a widespread surgical technique. A
successful technique for ileostomy was described by Brooks in 1952 and this is still in use today. A
stoma can be permanent or temporary and with the success of improved perioperative care, stomas
are now routinely made during emergency and elective surgery [1,2].
In the elective setting trends are more towards an ileostomy as a temporary stoma, for
example, defunctioning in a low anterior resection and colostomy as a permanent stoma which is
easier to manage. The role of a defunctioning stoma for low anterior resection is well established,
although defunctioning procedures does not decrease the anastomotic leak rate but does affect the
consequences of small anastomotic leak in relation to the rate of a second operation [3]. For elective
patients preoperative planning and counseling are extremely important prior to the creation of
an acceptable and functional ostomy. Even with the improved stoma care support and counseling
in elective settings, the psychological effects of having a stoma can affect the short and long term
outcomes.
In emergency surgery a stoma may be a lifesaving procedure to control sepsis during the acute
illness, this normally get reversed when the patient has fully recovered. Due to time constrains
pre-operative counseling and planning are not possible especially when operating out of hours. In
the emergency setting stoma formation is often regarded as the least
important part of an operation, which may be relegated to the most
junior member of the operating team.
The stoma made in emergency surgery have high short and long
term complication rate.
Emergency stomas where the site has not been marked
preoperatively by a stoma therapist are more prone to complications.
These complications may severely affect a patient’s quality of life.
We have retrospectively evaluated 199 operations where a stoma
was created. These were carried out at a single centre over a three
years period. We analysed the data and identified the short and long
term general and stoma specific complications in emergency and
elective cohorts.
Figure 1
Table 1
Methods and Materials
This was a retrospective analysis of data for all of the ostomy
patients over the last 3 years covering the period from January 2013
to January 2016, using the electronic record system. The department
stoma care team keeps a detailed record of all the patients who have
had a stoma.
The inclusion criteria for the study were
(1) All patients who had a non-urological stoma created in a last
four year period.
(2) Patient age >16 years.
The exclusion criteria was
1) Any patient who died within 48 hours of admission was
excluded from the study.
There were four patients excluded from the analysis. We included
all remaining patients who had either had emergency surgery or an
elective stoma during this period. Patients were divided into two
cohorts of elective and emergency surgery. The patient’s demography,
indication for the stoma, type of stoma (i.e. colostomy or ileostomy,
loop or end), intension of the stoma (i.e. temporary or permanent),
length of hospital stay (LOS) and early complications, were all
analysed.
We used the Clavien-Dindo classification to compare the short
term complication rate during the inpatient hospital stay. We also
recorded how many patients given a temporary stoma subsequently
their stoma had reversed. Long term stoma specific complications
were compared between two cohorts.
Table 2
Results
199 patients were identified over the three year study period. Four patients died within forty eight hours of their hospital admission and were therefore excluded from the analysis. One death was after elective surgery and three were emergency admissions. Patient distribution is shown in Figure 1.
Demography
The mean age was 63 ± 21 years in the emergency cohort and 57±
19 years in the elective cohort.
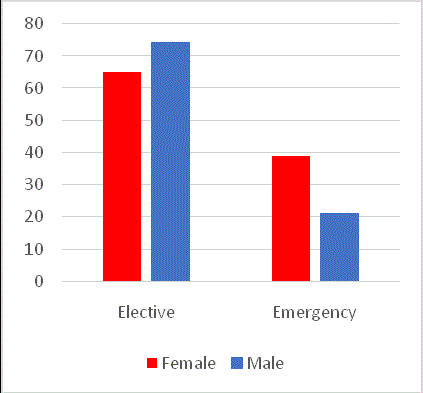
There were 102 female and 93 male patients. The male to female
ratio in the elective and emergency surgery cohorts is shown in Figure
2. Most emergency stomas were female patients compared to male
who had predominantly elective stomas.
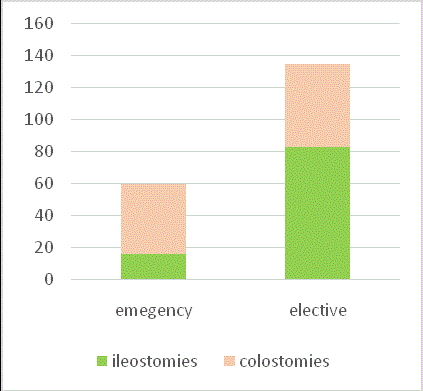
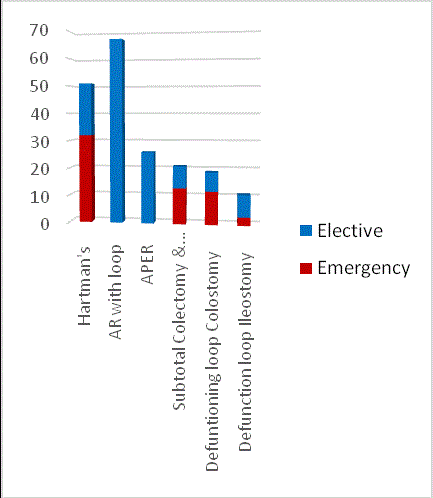
Figure 3 shows the type of stomas made in emergency and
elective cohort, predominant stomas in elective setting was ileostomy
as compared to colostomy in emergency cohort. Surprisingly only 60
stomas were created during emergency surgery. The most common
type of stoma made during emergency surgery was an end colostomy
(Hartman’s procedure). The emergency indications for stoma
formation are shown in Table 1. The most common indication was
perforated diverticular disease followed by large bowel obstruction
secondary to colorectal cancer. Two colostomies were required
secondary to iatrogenic trauma during gynaecological surgeries.
Overall 62% (37 cases) of emergency stoma were later reversed.
Patients with major co-morbidities and being high risk for a second
operation were the most common reason for non-reversal of the
stoma.
There were 135 elective stomas undertaken. Table 2 shows
diagnosis and indication for stoma surgery in elective cohort while
Figure 4 shows the type of operations in both the elective and
emergency cohorts. The most common stoma type was an ileostomy
and the most common indication was defunctioning after rectal
surgery. 77% (103 cases) of the ileostomy cohort were later reversed.
The main reason for non-reversal in the elective group was patient
choice and this was followed by patient comorbidities.
There were 52 colostomies made in elective setting including low
Hartman’s, APER and defunctioning colostomies.
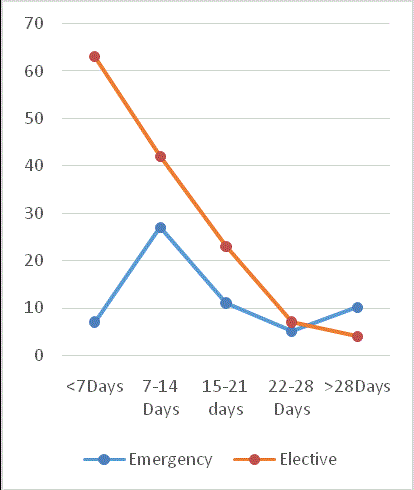
The average length of stay was higher in emergency group then
elective group. Median stay was 11days in elective and 14 days in
emergency cohort. (T-Test P Value .02). Figure 5 shows 46% of
elective patients and 11% of emergency patients were discharged
home within one week of surgery. In the second week post-surgery
the majority (45%) of patients discharged were in the emergency
group. After the second week there was no difference between the
two cohorts.
The short term complication rate was graded using the Clavien-
Dindo classification (see appendix 1). There is no significant
difference in grade 1 and grade 2 complications in emergency and
elective stoma patients. However there is a significant higher rate of
grade 3 and grade 4 complications in the emergency cohort compared
to the elective cohort. This is shown in Table 3.
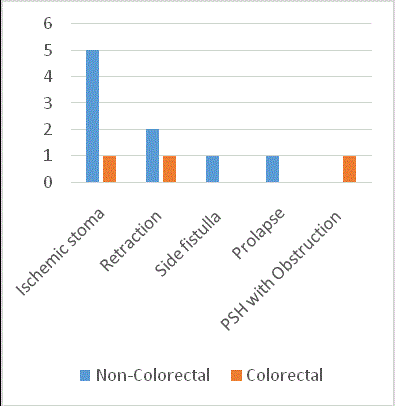
The majority of complications in emergency surgery group
were related to the stoma (Figure 6). This includes ischemic stoma,
retraction, and side fistula all requiring a second operation. Most of
these surgeries are directly or indirectly supervised by consultant
surgeons.
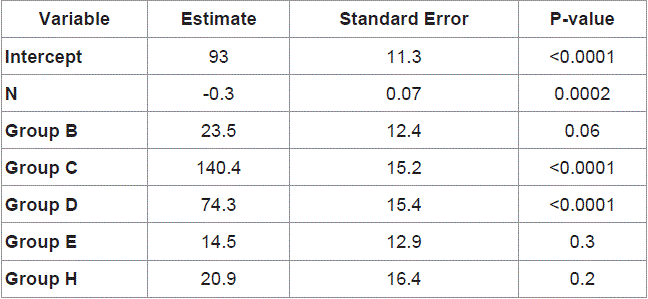
Table 4 shows the long term out come over the follow up period
of 1 year only. There is 3 fold increases in skin complication in
emergency group due to poor fittings and para-stomal hernias.
Similarly the incidence of para-stomal hernia is much higher in
patients who have emergency operation.
There were three deaths in emergency surgery cohort. The causes
for which were multifactorial including pulmonary embolism,
hospital acquired pneumonia and Myocardial Infarction (MI). These
patients were generally unwell and had a metabolic abnormality on
admission. They were operated on for a life threatening condition and
the reason for stoma in this group of patients was as they would not
tolerate an anastomosis or lengthy procedure. This explains the high
mortality rate in this group.
One elective death was due to massive Myocardial Infarction
(MI) in HDU is early post-operative period.
Figure 2
Figure 3
Figure 4
Table 3
Table 4
Figure 5
Figure 6
Discussion
On review of literature several studies were found to show that
colorectal patients undergoing emergency surgery are normally older
than those having elective surgery [3,4]. The reason of this is mainly
due to effective screening and awareness program in western world to
decrease colonic cancer mortality. Our study also showed this trend,
with the mean age in the emergency cohort being 6 years older than
the elective group.
The literature does not show any gender specific difference for
emergency colorectal surgery. However elective colorectal surgery
has a slightly higher incidence toward male patients [5]. This was also
true in our study which showed a slight male predominance in the
elective group. Whilst the emergency surgery group showed a slight
female predominance.
Colonic emergencies remain major life threatening conditions
associated with high morbidity and mortality rates [6]. Non-specific
abdominal symptoms account for their delayed presentation especially
in elderly patients with multiple comorbidities and limited metabolic
reserves. In our study there is a significant difference in the mortality
rate among the emergency and elective groups. The mortality rate in
the emergency cohort was related to the underlying pathology and
was not found to be a direct complication of the surgery.
It is relatively common to create stoma in both emergency and
elective bowel surgery. They are necessary for several colonic and
rectal conditions and represent a major change in patient quality of
life. Previous studies have discussed risk factors, complications and
outcomes of stomas made in both the emergency and elective setting
[7].
Emergency stomas are shown to have a higher complication rate
[8]. This was also true in our study which showed a higher rate of
complications in the emergency cohort. We found the majority of
complications were grade 1 and 2. However surprisingly there was
a significant difference for grade 3 complications between the two
groups which were directly related to the stoma leading to a second
operation.
The choice of stoma in emergency surgery is disease depend.
In our study most of the stomas were end colostomy secondary to
a recto-sigmoid resection (Hartmann’s procedure). As compared to
elective settings it is the surgeon choice to bring an ileostomy or a
colostomy for defunctioning after an anastomosis [9]. Technically
emergency stomas are much more difficult to create due oedema and
inflammation of bowel.
It has been discussed that single stage colonic surgery with
primary anastomosis in selected cases is deemed safe, but mainly in
specialist hands. In many studies the optimal strategy proposed for
perforated diverticulitis was a resection with a primary anastomosis
with defunctioning stoma [10] and the colorectal surgeons were more
likely to perform a single stage operation.
Stoma creation is not a trivial undertaking. It involves a careful
surgical technique to minimize the complication rate (which may be
relatively frequent) and promotes good ostomy function. Various
studies have reported stoma complication rates of 21% to 70% [11,12].
Approximately a fifth of stomas have to be sited in emergencies.
These stomas may be left permanently due to patient choice or comorbidities
preventing further surgery as shown in our study too.
Therefore selecting the site for stoma placement is important for a
good outcome. This has been discussed in the literature which shows
in the absence of input, for marking and placement of the stoma,
from a stoma specialist nurse there is increase in both short and long
term complications [13].
There are several classification systems for parastomal hernias
that are based on size, location, contents, and radiologic findings
associated with the hernia [14-17]. The evidence favour the use of
mesh in elective setting to prevent the long term complication of
para-stomal hernia without any increase in morbidity [18]. Although
there is controversy on the type of mesh and location of the mesh used
during elective setting. The use of prophylactic mesh in emergency
stomas setting is still not recommended.
Skin complication related to stoma is multifactorial in origin. It
can range from simple allergic reaction to skin excoriation due to
poorly fitted appliances. Most of the skin related problems are dealt
with stoma nurses and these patients never get to see the surgeons. In
our study there is threefold increase in the skin complication among
emergency group. This could be possibility due to high incidence of
parastomal hernias leading to poor appliance fitting etc.
As previous studies have shown clear outcome differences between
emergency and elective operation for bowel related operations, our
study has focused on the stoma related outcomes in emergency
and elective settings. This is very important with regards to patient
morbidity and in some cases can influence long term outcomes such
as the patient’s quality of life.
We acknowledge that this study is subject to the limitations of a
single centre retrospective study. Nevertheless, our data is a useful
guide for future efforts attempting to improve outcomes for stoma
surgery in emergency and elective settings.
Conclusion
Emergency stoma surgery is a challenging operation. Dealing
with poorly optimised patient with poor metabolic reserves needs an
expert surgeon to improve both short and long term out comes.
Further studies are needed to show that does surgeon’s
subspecialty interest in colorectal surgery influence the outcome in
these patients?
References
- Shiomi A, Ito M, Saito N, Hirai T, Ohue M, Kubo Y, et al. The indications for a diverting stoma in low anterior resection for rectal cancer: A prospective multicentre study of 222 patients from Japanese cancer centres. Colorectal Dis. 2011;13(12):1384-9.
- Ulrich AB, Seiler C, Rahbari N, Weitz J, Büchler MW. Diverting stoma after low an-terior resection: More arguments in favour. Dis Colon Rectum. 2009;52(3):412-8.
- Scott NA, Jeacock J, Kingston RD. Risk factors in patients presenting as an emergency with colorectal cancer. Br J Surg. 1995;82(3):321-3.
- Merkel S, Meyer C, Papadopoulos T, Meyer T, Hohenberger W. Urgent surgery in colon carcinoma. Zentralbl Chir. 2007;132(1):16-25.
- Wen-long Gu, Sheng-wen Wu. Meta-analysis of defunctioning stoma in low anterior resection with total mesorectal excision for rectal cancer: Evidence based on thirteen studies. World J Surg Oncol. 2015;13:9.
- Bayar B, Yılmaz KB, Akıncı M, Şahin A, Kulaçoğlu H. An evaluation of treatment results of emergency versus elective surgery in colorectal cancer patients. Ulus Cerrahi Derg. 2016;32(1):11-17.
- Kwan TL, Lai F, Lam CM, Yuen WC, Wai A, Siu YC. Population-based information on emergency colorectal surgery and evaluation on effect of operative volume on mortality. World J Surg. 2008;32(9):2077-82.
- Biondo S, Kreisler E, Millan M, Fraccalvieri D, Golda T, Frago R, et al. Impact of surgical specialization on emergency colorectal surgery outcomes. Arch Surg. 2010;145(1):79-86.
- Arumugam PJ, Bevan L, Macdonald L, Watkins AJ, Morgan AR, Beynon J, et al. A prospective audit of stomas analysis of risk factors and complications and their management. Colorectal Dis. 2003;5(1):49-52.
- Caricato M, Ausania F, Ripetti V, Bartolozzi F, Campoli G, Coppola R. Retrospective analysis of long-term defunctioning stoma complications after colorectal surgery. Colorectal Dis. 2007;9(6):559-61.
- Goligher J. Colorectal surgery as a specialty. J R Soc Med. 1996;89(11):601- 3.
- Constantinides VA, Heriot A, Remzi F, Darzi A, Senapati A, Fazio VW, et al. Operative strategies for diverticular peritonitis: A decision analysis between primary resection and anastomosis versus Hartmann's procedures. Ann Surg. 2007;245(1):94-103.
- Shabbir J, Britton DC. Stoma complications: A literature overview. Colorectal Dis. 2010;12(10):958-64.
- Devlin HB. Peristomal hernia. In: Dudley H, editor. Operative surgery: alimentary tract and abdominal wall. 4th edition. London: Butterworths; 1983;1:p.441-3.
- Moreno-Matias J, Serra-Aracil X, Darnell-Martin A, Bombardo-Junca J, Mora-Lopez L, Alcantara-Moral M, et al. The prevalence of parastomal hernia after formation of an end colostomy. A new clinico-radiological classification. Colorectal Dis. 2009;11(2):173-7.
- Gil G, Szczepkowski M. A new classification of parastomal hernias from the experience at Bielański Hospital in Warsaw. Pol Przegl Chir. 2011;83(8):430-7.
- Seo SH, Kim HJ, Oh SY, Lee JH, Suh KW. Computed tomography classification for parastomal hernia. J Korean Surg Soc. 2011;81(2):111-4.
- Cross AJ, Buchwald PL, Frizelle FA, Eglinton TW. Meta-analysis of prophylactic mesh to prevent parastomal hernia. Br J Surg. 2017;104(3):179- 86.