Research Article
Review of Predictors of Postoperative Pain
Arthur Paredes Gatti*
Department of Head and Neck Surgery, Federal University of São Paulo, Brazil
*Corresponding author: Arthur Paredes Gatti, Department of Head and Neck Surgery, Federal University of São Paulo, Napoleão de Barros Str, 566 (ap. 71). Vila Cementino, São Paulo-SP, (04024- 002), Brazil
Published: 27 Aug, 2018
Cite this article as: Gatti AP. Review of Predictors of
Postoperative Pain. World J Surg
Surgical Res. 2018; 1: 1048.
Abstract
Introduction: Pain in the postoperative period reported by the patient (acute or chronic) is an
important aspect that must be taken into consideration and widely studied, since it interferes in
the patient's acceptance by this method of treatment, prognosis, quality of life, besides being a
descriptor of the quality of the service in which the surgery was performed and of the professionals
involved. Currently, the patient takes into consideration not only the treatment itself of his illness,
but how this will impact his life after the procedure.
Materials and Methods: A review was conducted in the literature in order to describe the main
predictors of postoperative pain and its importance. Fifty studies were analyzed between 2002 and
2018, whose objective was to evaluate the impact of postoperative pain on the patient's quality of life.
Results and Discussion: Different types of scores were shown to be used as a predictor of
postoperative pain. The psychological and emotional changes, followed by the demographic
differences were the most important aspects found in the preoperative period that can measure the
risk for postoperative pain.
Conclusion: The perception of quality of life changes according to the study group analyzed in
relation to the referred disease and the cultural and social environment in which the individual
is inserted, making the analysis often subjective, but as fundamental for the relationship between
patient and multi professional team with better outcome treatment.
Keywords: Predictors; Postoperative; Pain
Introduction
Pain, according to the International Association for the Study of Pain (IASP), is described as
"an unpleasant sensory and emotional experience associated with actual or potential tissue damage
or described in terms of such damage" [1]. About 5% of individuals who undergo any surgical
procedure will develop persistent severe pain associated with some chronic physical limitation or
psychosocial impairment [2,3], especially those associated with neurological lesions [4]. The study
for the management of postoperative pain for more than three decades focused on pharmacology
and anesthesiology [5,6], but faced with a modest solving of cases addressed [7,8].
Neural messages ascend through the peripheral nerves to the cortex, generating awareness of
the message. These messages can be modulated through these pathways in several places, allowing
similar pain stimuli to generate different responses in each individual [9,10].
Painful sensations are a major concern in post-operative multidisciplinary and interdisciplinary
care, not only because of the patient's suffering, but also because it influences the recovery process
[11].
Tissue trauma generates a mediated inflammatory response that increases sensitivity around the
lesion (hyperalgesia) or alteration of pain perception to generally non-harmful stimuli (allodynia).
Another mechanism that contributes to these two phenomena includes the sensitization of peripheral
pain receptors (primary hyperalgesia) and increased excitability of central nervous system neurons
(secondary hyperalgesia) [12-14].
In the literature it is possible to find that pain is not exclusively dependent on the degree of
the lesion that generated it (organic), being the intensity and the character directly influenced by
previous experiences, memories and the capacity of the human being to understand the causes and
consequences [15]. Among the several factors, the psychological, cognitive, affective variables, age,
gender, weight and location of the lesion are the most prominent [16-21].
All these aspects, associated with the reason for the injury, generate a series of postoperative
complications, such as cardiopulmonary, thromboembolic,
immunological and endocrinological disorders [22-25]. The
adequate management of postoperative pain is a fundamental item
of preoperative care to avoid the problems already mentioned,
improving recovery of the patient, quality of life, prognosis, and it
can be considered for the patient, hospital and the care team also a
predictor of quality and satisfaction of the service provided [26-31].
Due to the importance presented and the great divergence of
predictors of postoperative pain in published studies, we reviewed
the literature search in major predictors and how they have proved
important.
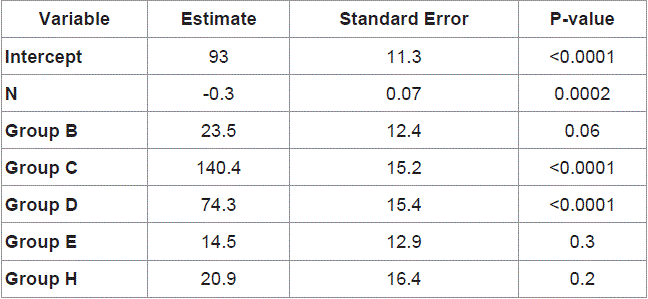
Table 1
Materials and Methods
A review was conducted in the literature in order to describe the main predictors of postoperative pain and its importance. Fifty studies were analyzed between 2002 and 2018 (PubMed, SunSearch and Scielo), whose objective was to evaluate the impact of postoperative pain on the patient's quality of life. The descriptors analyzed were Predictors, Postoperative, Pain, and Postoperative Pain.
Results and Discussion
In several studies, preoperative tests were used and compared
with the postoperative response. Among these tests, the Quantitative
Sensory Testing (QST) [32] defined based on mechanical quantifiable
(pressure, local puncture, vibration and light touch), thermal (painful
cold, refreshing, warm and painful heat) or electrical stimulation. In
one study, the preoperative pain tests were predictors of 4% to 54%
of the postoperative pain experience (varying between the methods
used) [33]. Other results (divergent from the present study using
QST) have shown that factors such as demographic (age and sex [34-
37]) and psychological factors (depression [38-42], anxiety [43-45]
and vulnerability [46]) are of great importance in the prediction of
postoperative pain [33].
In another research [4], which was based on the Diffuse Noxious
Inhibitory Control (DNIC), new results were obtained. DNIC is
calculated as the difference in pain rating between two identical pain
tests, applied first at the baseline and then concomitantly with another
distressing stimulus at distant [47]. Decreased DNIC efficiency is
associated with an increased history of pain in healthy patients [48].
Thus, it was suggested that DNIC was also a good predictor of chronic
postoperative pain. Such research has resulted in the evidence that
DNIC is efficient for evaluation of pain modulation, not as a statistical
parameter of pain threshold or to estimate the supralimilar magnitude
of the noxious stimulus; thus being a predictor of postoperative pain
for this purpose [4].
The Visual Analogue Scale (VAS) can be used to measure pain,
ranging from 0 mm to 100 mm. Its use requires the patient to score
the intensity of their pain represented by a point between the extremes
"without any pain" and "worse imagined pain". In addition to being
simple, this validated test is a great tool for describing pain in severity
and intensity [49]. For these reasons, VAS was used in a research to
determine whether preoperative pain expectancy could be correlated
with post-operative pain experience [50]. Psychological factors
(anxiety and/or depression) were considered as important predictors
of POD [39,40,51] as well as age, especially in the lower extremities
[39]. In this particular case, the researchers were nurses, which value
the research, since they spend an extended time with each patient
to better evaluate them [52]. Patients with an efficient and more
collaborative analgesia had a faster recovery and were discharged
earlier, even with a reduced risk of postoperative pain [53].
In this same analysis [39], the Multidimensional Health Locus
of Control (MHLC) was used. This scale measures expectation about
patient control and was developed for the prediction of health-related
behaviors [54]. In the study, no correlation was found between the
MHLC and the intensity of the pain [50], confronting the literature,
where correlations can be found between these two [54].
As already described, analgesia has an important credit to prevent
postoperative pain. Some studies [55,56] have shown that inadequate
analgesia [55], gender, age, body weight, presence of cancer and the
variety of the surgical site are important variables for evaluating
postoperative pain [56]. These results, in one of them, were obtained
from the study between Intravenous Patient-Controlled Analgesia
(IVPCA) with narcotic and postoperative pain. Body weight was the
most relevant item when compared to the other factors evaluated and
the presence of cancer was the least relevant [56].
The psychological evaluation of the patient in the preoperative
period is a fundamental criterion, described in several studies. In
one, VAS was used again to evaluate patients who underwent surgery
in the oral, pharyngeal, laryngeal, neck and salivary glands regions.
In this study, it was found that the variables age, sex, preoperative
pain, expected pain, short-term fear, and catastrophic pain have a
predictive value for postoperative pain [57]. This last variable was the
differential of this study when compared with others, since most do
not use catastrophic pain as a criterion, placing pain expectation and
anxiety as independent predictors [58-60], while in this it is shown
that there are several other points to be the patient's evaluation [57].
Still regarding pain catastrophizing, a study of patients who
underwent arthroplasty knee showed that psychological disorders
such as depression, anxiety, panic or beliefs related to health, such
as belief in themselves, pain catastrophizing and instability to the
movement are related with predictions reserved after this surgery
[61], based on previous research [62-65].
The anxiety was present in almost all the works analyzed and the
items on which these works were based. In multidisciplinary aspects,
research in the dentistry area showed that anxiety is a predictor of
acute pain in patients submitted to outpatient exodontia. In this case,
the history of tooth extraction and pain are intimately fixed, since
it was from these points that the study of anesthesia was developed.
The parameters analyzed were collected through a multiparametric
oximeter (heart rate, oxygen saturation and blood pressure) during
and after the procedure, besides the use of VAS and repeated after 48
hrs and 7 days. Through vital signs, no significant differences were
found, but with VAS there were such differences [66]. The use of
analgesic drugs in the postoperative period was also a predictor of
postoperative pain, based on a study that analyzed the consumption
and variables: pain, anxiety, age and kind of surgery [67]. In this
case, the patients analyzed by gynecologists and obstetricians in the
post-cesarean period [68,69] revealed that the perception of pain or
analgesia has a correlation with postoperative pain [59,60,70] and
consumption of analgesics [71].
Post-surgical recovery was the main focus in many studies. One
of them dealt with the redistribution of immune cells induced by
surgical stress and postoperative recovery, being this an important
predictor, adding other variables as sex (little relevant, with
discrete worse results for the female sex) [72]. Another showed that
demographic factors such as age, body mass index, and gender (this
is more relevant in females) has a potential impact on recovery [73].
Endorsing this predictor, there was a work with cancer patients with
esophageal disease and quality of life, which included post-operative
pain [74,75] in addition to using different scales such as the Social
Functioning Scale, Pain Scale and the expected Global Activity Level
[74].
Only two studies [76,78] aimed the pediatric patient for
post-operative pain predictors. The first questioned whether the
presence of the parents in the post-anesthesia recovery room would
have a positive effect on pain, crying and recovery. In the case of
crying, there was no significant evidence, but there was a decrease
in the negative response two weeks after surgery. In addition, it
was pointed out that anxiety is related to high levels of pain, sleep
disorders and behavior problems [77]. In the second, the question
was whether the introduction of Professional Clown Doctors during
the period of anesthesia in children would have some positive effect
on the reduction of anxiety and, consequently, improvements in
the postoperative period, including decreased crying, pain and
acceleration recovery [78]. The result was that health professionals
indicated that there was an expected benefit, reducing the anxiety
rates of pediatric patients, but most of the professionals objected to
the implantation of this system, warning that there was a negative
interference in the procedures in the surgical center [78] (which
contrasts, in part, with the literature [79,80]).
Some hospitals use tools to measure their quality through analysis
of patient satisfaction, which includes the response to postoperative
pain. One of the studies used the 5-point Likert scale and the 6-point
Likert scale to discover that the overall satisfaction level was moderate
(56.5%) with their anesthetic care due to different reasons. Nausea
and vomiting control (35.6%) was the most common postoperative
reasons for dissatisfaction followed by pain control (31.7%) [81].
The Generalized Anxiety Disorder 7-Item Scale (GAD-7)
measured 42.5% of anxiety on 106 patients with lumbar disc
herniation, corroborating with the literature [82].
Conclusion
Many clinical trials have used tests and scores as predictors of
postoperative pain both in the pre-surgical and postoperative periods,
with large and important results (Table 1). It has been shown that, in
addition to the correct management of medications to relieve pain
resulting from surgery, demographic and psychological factors are
closely related.
It has been shown in previous research that in humans, the "pain"
factor is not only dependent on the degree of the organic lesion, but
also on several other factors, such as intensity and previous memories,
as well as understanding the consequences that the lesion can generate
[15,16], showing that the psychological factor is present and should
be investigated to differentiate patients at risk for postoperative pain.
According to some authors [83,84], fear can be considered a primary
emotion related to a specific object or situation and the individual
reacts with a set of behavioral and neurovegetative responses. When
associated with a non-obvious danger, but which presents itself in a
vague and persistent way, a picture of apprehension, called anxiety,
can be seen. Anxiety, along with other psychological aspects, proved
to be a strong predictor of postoperative pain and easy measurement
by tests such as VAS [66] and MLHC [50].
The combination of psychosocial and psychological aspect of
dor [4,59,61,85] including pain catastrophizing [57] should not
be considered separately. A broad approach should also be taken
in the whole picture, including the kind of surgery the patient will
undergo [67,86], the kind of anesthesia to be administered [67] and
the patient's response to all preoperative management [87], both for
adults and for children [78].
A mutation in the μ-opioid receptor gene has been shown to
increase β-endorphin binding affinity, resulting in a reduction in pain
sensitivity in healthy adults [88]. This shows that, in addition to the
approach focused on this study, other biomolecular aspects can be
used as predictors of pain.
The recovery of the patient after surgery, as well as their
satisfaction [76] with the service provided is related to the adequate
management of pain [26-30]. This adequate regulation not only can
be seen macroscopically, but immunological data can be analyzed to
collaborate with the research89 and predict what kind of response the
patient will present and what help we can provide [72].
It is expected that in the future, based on researches such as this
one, the health team can routinely find patients at greater risk for
developing postoperative pain and use predictive criteria for their
management.
Acknowledgment
We thank the Department of Head and Neck Surgery – Federal University of São Paulo and São Camilo University Center for their assistance in the development of this research.
References
- Crombie IK. The potencial of Epidemiology. In: Crombie, editor. Epidemiology of pain: a report of the Task Force on Epidemiology. Seattle: IASP Press, 1999;1:1-5.
- Kehlet H, Jensen TS, Woolf CJ. Persistent postsurgical pain: Risk factors and prevention. Lancet. 2006;367(9522):1618-25.
- Poleshuck EL, Green CR. Socioeconomic disadvantage and pain. Pain. 2008;136(3):235-8.
- Yarnitsky D, Crispel Y, Eisenberg E, Granovsky Y, Ben-Nun A, Sprecher E, et al. Prediction of chronic post-operative pain: Pre-operative DNIC testing identifies patients at risk. Pain. 2008;138:22-8.
- Werner MU, Rotboll-Nielsen P. The acute pain service - roles and challenges. Curr Anaesth Crit Care. 2007;18(3):135-9.
- Rawal N. Organization, function and implementation of acute pain service. Anesthesiol Clin North America. 2005;23:211-25.
- Liu SS, Wu CL. Effect of postoperative analgesia on major postoperative complications: A systematic update of the evidence. Anesth Analg. 2007;104(3):689-702.
- White PF, Kehlet H. Postoperative pain management and patient outcome: Time to return to work! Anesth Analg. 2007;104(3):487-9.
- Edwards RR. Individual differences in endogenous pain modulation as a risk factor for chronic pain. Neurology. 2005;65(3):437-43.
- Mogil JS. The genetic mediation of individual differences in sensitivety to pain and its inhibition. Proc Natl Acad Sci USA. 1999;96(14):7744-51.
- Shiloh S, Zukerman G, Butin B, Deutch A, Yardeni I, Benyamini Y, et al. Postoperative Patient-Controlled Analgesia (PCA): How much control and how much analgesia? Psychology and Health. 2003;18(6):753-70.
- Kelly DJ, Ahmad M, Brull SJ. Preempive analgesia I: Physiological pathways and pharmacological modalities. Can J Anaesth. 2001;48(10):1000-10.
- Woolf CJ, Chong MS. Preemptive analgesia-treating postoperative pain by preventing the establishment of central sensitization. Anesth Analg. 1993;77(2):362-79.
- Suzuki H. Recent topics in the management of pain: Development of the concept of preemptive analgesia. Cell Transplant. 1995;4(Suppl 1):S3-6.
- Maggirias J, Locker D. Psychological factors and perceptions of pain associated with dental treatment. Community Dent Oral Epidemiol. 2002;30(2):151-9.
- Sullivan MJ, Rodgers WM, Kirsch I. Catastrophizing, depression and expectancies for pain and emotional distress. Pain. 2001;91(1-2):147-54.
- Burns JW, Hodsman NBA, McLintock TTC, Gillies GWA, Kenny GNC, McArdle CS. The influence of patient characteristics on the requirements for postoperative analgesia. A reassessment using patient-controlled analgesia. Anaesthesia. 1989;44:2-6.
- Chang KY, Tsou MY, Chan KH, Sung CS, Chang WK. Factors affecting patient-controlled analgesia requirements. J Formos Med Assoc. 2006;105(11):918-25.
- Glasson JC, Sawyer WT, Lindley CM, Ginsberg B. Patient-specific factors affecting patient-controlled analgesia dosing. J Pain Palliat Care Pharmacother. 2002;16(2):5-21.
- Macintyre PE, Jarvis DA. Age is the best predictor of postoperative morphine requirements. Pain. 1996;64(2):357-64.
- Tsui SL, Tong WN, Irwin M, Ng KF, Lo JR, Chan WS, et al. The efficacy, applicability and side-effects of postoperative intravenous patient-controlled morphine analgesia: An audit of 1233 Chinese patients. Anaesth Intensive Care. 1996;24(6):658-64.
- Ballantyne JC, Carr DB, DeFerranti S, Suarez T, Lau J, Chalmers TC, et al. The comparative effects of postoperative analgesic therapies on pulmonary outcome: Cumulative meta-analyses of randomized, controlled trials. Anesth Analg. 1998;86(3):598-612.
- Beattie WS, Buckley DN, Forrest JB. Epidural morphine reduces the risk of postoperative myocardial ischaemia in patients with cardiac risk factors. Can J Anaesth. 1993;40(6):532-41.
- Scarry E. The body in pain. Oxford, Oxford University Press. 1985.
- Kiecolt-Glaser JK, Page GG, Marucha PT, MacCallum RC, Glaser R. Psychological influences on surgical recovery. Perspectives from psychoneuroimmunology. Am Pshycol. 1998;53(11):1209-18.
- Rosenberger PH, Jokl P, Ickovics J. Psychosocial factors and surgical outcomes: An evidence-based literature review. J Am Acad Orthop Surg. 2006;14(7):397-405.
- Schimmer RC, Brulhart KB, Duff C, Glinz W. Arthroscopic partial meniscectomy: A 12-year follow-up and two-step evaluation of the long-term course. Arthroscopy. 1998;14(2):136-42.
- Daniel DM. Selecting patients for ACL surgery. In: Jackson DW, editor. The anterior cruciate ligament. Current and future concepts. New York: Raven Press. 1993;251-8.
- McConville OR, Kipnis JM, Richmond JC, Rockett SE, Michaud MJ. The effect of meniscal status on knee stability and function after anterior cruciate ligament reconstruction. Arthroscopy. 1993;9(4):431-9.
- Swenson TM, Harner CD. Knee ligament and meniscal injuries. Current concepts. Orthop Clin North Am. 1995;26(3):529-46.
- Myles PS, Williams DL, Hendrata M, Anderson H, Weeks AM. Patient satisfaction after anaesthesia and surgery: Results of a prospective survey of 10,811 patients. Br J Anaesth. 2000;84:6-10.
- Arendt-Nielsen L, Yarnitsky D. Experimental and clinical applications of quantitative sensory testing applied to skin, muscle and viscera. J Pain. 2009;10(6):556-72.
- Werner MU, Mjobo HN, Nielsen PR, Rudin A. Prediction of postoperative pain: A systematic review of predictive experimental pain studies. Anesthesiology. 2010;112(6):1494-502.
- Hadjistavropoulos T, Herr k, Turk DC, Fine PG, Dworkin RH, Helme R, et al. An interdisciplinary expert consensus statement on assessment of pain in older persons. Clin J Pain. 2007;23:S1-43.
- Gibson SJ. IASP global year against pain in older persons: Highlighting the current status and future perspectives in geriatric pain. Expert Rev Neurother. 2007;7(6):627-35.
- Keogh E, Herdenfeldt M. Gender, coping and the perception of pain. Pain. 2002;97(3):195-201.
- Holdcroft A, Berkley KJ. Sex and gender differences in pains and its relief. Wall and Melzack’s Textbook of Pain, 5th Ed, Filadélfia, Elsevier Churchill Livingstone. 2006;1181-97.
- Kain ZN, Sevarino FB, Rinder C, Pincus S, Alexander GM, Ivy M, et al. Preoperative anxiolysis and postoperative recovery in women undergoing abdominal hysterectomy. Anesthesiology. 2001;94(3):415-22.
- Caumo W, Schmidt AP, Schneider CN, Bergmann J, Iwamoto CW, Adamatti LC, et al. Preoperative predictors of moderate to intense acute postoperative pain in patients undergoing abdominal surgery. Acta Anaesthesiol Scand. 2002;46(10):1265-71.
- Ozalp G, Sarioglu R, Tuncel G, Aslan K, Kadiogullari N. Preoperative emotional states in patients with breast cancer and postoperative pain. Acta Anaesthesiol Scand. 2003;47:26-9.
- Kudoh A, Takahira Y, Katagai H, Takazawa T. Small-dose ketamine improves the postoperative state of depressed patients. Anesth Analg. 2002;95:114-8.
- Brander VA, Stulberg SD, Adams AD, Harden RN, Bruehl S, Stanos SP, et al. Predicting total knee replacement pain: A postoperative, observational study. Clin Orthop Relat Res. 2003;27-36.
- Munafo MR, Stevenson J. Anxiety and surgical recovery. Reinterpreting the literature. J Psychosom Res. 2001;51(4):589-96.
- Kalkman CJ, Visser K, Moen J, Bonsel GJ, Grobbee DE, Moons KG, et al. Preoperative prediction of severe postoperative pain. Pain. 2003;105(3):415-23.
- Granot M, Ferber SG. The roles of pain catastrophizing and anxiety in the prediction of postoperative pain intensity: A prospective study. Clin J Pain. 2005;21(5):439-45.
- Rotboll-Nielsen P, Rudin A, Werner MU. Prediction of postoperative pain. Curr Anaesth Crit Care. 2007;18(3):157-65.
- Granot M, Weissman-Fogel I, Crispel Y, Pud D, Granovsky Y, Sprecher E, et al. Determinants of endogenous analgesia magnitude in a Diffuse Noxious Inhibitory Control (DNIC) paradigm: Do conditioning stimulus painfulness, gender and personality variables matter? Pain. 2008;136(2):142-9.
- Edwards RR, Ness TJ, Weigent DA, Fillingim RB. Individual differences in Diffuse Noxious Inhibitory Controls (DNIC): Association with clinical variables. Pain. 2003;106(3):427-37.
- Katz J, Melzack R. Measurement of pain. Surg Clin North Am. 1999;79(2):231-52.
- Ene KW, Nordberg G, Sjostrom B, Bergh I. Prediction of postoperative pain after radical prostatectomy. BMC Nurs. 2008;7:14.
- Nayman J. Measurement and control of postoperative pain. Ann R Coll Surg Engl. 1979;61(6):419-26.
- Nash R, Yates P, Edwards H, Fentiman B, Dewar A, McDowell J, et al. Pain and the administration of analgesia: What nurses say. J Clin Nurs. 1999;8(2):180-9.
- Perkins FM, Kehlet H. Chronic pain as an outcome of surgery. A review of predictive factors. Anesthesiology. 2000;93(4):1123-33.
- Wallston KA, Wallston BS, DeVellis R. Development of the Multidimensional Health Locus of Control (MHLC) scales. Health Educ Monogr. 1987;6(2):160-70.
- Puntillo KA, Wild LR, Morris AB, Stanik-Hutt J, Thompson CL, White C. Practices and predictors of analgesic interventions for adults undergoing painful procedures. Am J Crit Care. 2002;11(5):415-29.
- Yen CR, Tsou MY, Mandell MS, Chan CT, Chan KH, Chen TH, et al. An analysis of patient variables that influence intravenous patient-controlled analgesic use of morphine with quantile regression. Anesthesiology. 2010;112(3):688-95.
- Sommer M, Geurts JW, Stessel B, Kessels AG, Peters ML, Patijn J, et al. Prevalence and predictors of postoperative pain after ear, nose and throat surgery. Arch Otolaryngol Head Neck Surg. 2009;135(2):124-30.
- Thomas T, Robinson C, Champion D, McKell M, Pell M. Prediction and assessment of the severity of post-operative pain and of satisfaction with management. Pain. 1998;75(2-3):177-85.
- Pan PH, Coqhill R, Houle TT, Seid MH, Lindel WM, Parker RL, et al. Multifactorial preoperative predictors for postcesarean section pain and analgesic requirement. Anesthesiology. 2006;104(3):417-25.
- Mamie C, Bernstein M, Morabia A, Klopfenstein CE, Sloutskis D, Forster A. Are there reliable predictors of postoperative pain? Acta Anaesthesiol Scand. 2004;48(2):234-42.
- Riddle DL, Wade JB, Jiranek WA, Kong X. Preoperative pain catastrophizing predicts pain outcome after knee arthroplasty. Clin Orthop Relat Res. 2010;468(3):798-806.
- Ayres DC, Franklin PD, Ploutz-synder R, Boisvert CB. Total knee replacement outcome and coexisting physical and emotional illness. Clin Orthop Relat Res. 2005;440:157-61.
- Ayres DC, Franklin PD, Trief PM, Ploutz-synder R, Freund D. Psychological attributes of preoperative total joint replacement patients: Implications for optimal physical outcome. J Arthroplasty. 2004;19(7 Suppl 2):125-30.
- Brander V, Gondek S, Martin E, Stulberg SD. Pain and depression influence outcome 5 years after knee replacement surgery. Clin Orthop Relat Res. 2007;464:21-6.
- Brander VA, Stulberg SD, Adams AD, Harden RN, Bruehl S, Stanos SP, et al. Predicting total knee replacement pain: A prospective, observational study. Clin Orthop Relat Res. 2003;416:27-36.
- Siviero M, Nhani VT, Prado EFGB. Análise da ansiedade como fator preditor de dor aguda em pacientes submetidos a exodontias ambulatoriais. Rev Odontol UNESP. 2008;37(4):329-36.
- Ip HY, Abrishami A, Peng PW, Wong J, Chung F. Predictors of postoperative pain and analgesic consumption: A qualitative systematic review. Anesthesiology. 2009;111(3):657-77.
- Strulov L, Zimmer EZ, Granot M, Tamir A, Jakobi P, Lowenstein L. Pain catastrophizing, response to experimental heat stimuli and post-cesarean section pain. J Pain. 2007;8(3):273-9.
- Granot M, Lowenstein L, Yarnitsky D, Tamir A, Zimmer EZ. Postcesarean section pain prediction by preoperative experimental pain assessment. Anesthesiology. 2003;98(6):1422-6.
- Taenzer P, Melzack R, Jeans ME. Influence of psychological factors on postoperative pain, mood and analgesic requirements. Pain. 1986;24:331-42.
- Jamison RN, Taft K, O`Hara JP, Ferrante FM. Psychosocial and pharmacologic predictors of satisfaction with intravenous patient-controlled analgesia. Anesth Analg. 1993;77:121-5.
- Rosenberger PH, Ickovics JR, Epel E, Nadler E, Jokl P, Fulkerson JP, et al. Surgical stress-induced immune cell redistribution profiles predict short-term and long-term postsurgical recovery. A prospective study. J Bone Joint Surg Am. 2009;91(12):2783-94.
- Fabricant PD, Rosenberger PH, Jokl P, Ickovics JR. Predictors of short-term recovery differ from those of long-term outcome after arthroscopic partial meniscectomy. Arthroscopy. 2008;24(7):769-78.
- Heijl MV, Sprangers MA, DeBoer AG, Lagarde SM, Reitsma HB, Busch OR, et al. Preoperative and early postoperative quality of life predict survival in potentially curable patients with esophageal cancer. Ann Surg Oncol. 2010;17:23-30.
- Gotay CC, Kawamoto CT, Bottomley A, Efficace F. The prognostic significance of patient-reported outcomes in cancer clinical trials. J Clin oncol. 2008;26(8):1355-63.
- Lardner DR, Dick BD, Crawford S. The effects of parental presence in the postanesthetic care unit on children’s postoperative behavior: A prospective, randomized, controlled study. Anesth Analg. 2010;110(4):1102-8.
- Kain ZN, Mayes LC, Caldwell-Andrews AA, Karas DE, McClain BC. Preoperative anxiety, postoperative pain and behavioral recovery in young children undergoing surgery. Pediatrics. 2006;118(2):651-8.
- Vagnoli L, Caprilli S, Robiqlio A, Messeri A. Clown doctors as a treatment for preoperative anxiety in children: A randomized, prospective study. Pediatrics. 2005;116(4):563-7.
- Beck CT. Humor in nursing practice: A phenomenological study. Int J Nurs Stud. 1997;34(5):346-52.
- Hunt AH. Humor as a nursing intervention. Cancer Nurs. 1993;16:34-9.
- Alsaif A, Alqahtani S, Alanazi F, Alrashed F, Almutairi A. Patient satisfaction and experience with anesthesia: A multicenter survey in Saudi population. Saudi J Anaesth. 2018;12(2):304-10.
- Laufenberg-Feldmann R, Kappis B, Camara RJA, Ferner M. Anxiety and its predictive value for pain and regular analgesic intake after lumbar disc surgery - A prospective observational longitudinal study. BMC Psychiatry. 2018;18:82.
- Rocha RG. O medo e a ansiedade no tratamento odontológico: controle através de terapêutica medicamentosa. In: Feller C, Gorab R, editors. Atualização na clínica odontológica. 19° Congresso Paulista de Odontologia, São Paulo: Artes Médicas. 2000;381-410.
- Rudin A, Wolner-Hanssen P, Hellbom M, Werner MU. Prediction of post-operative pain after a laparoscopic tubal ligation procedure. Acta Anaesthesiol Scand. 2008;52(7):938-45.
- Raj PP. Management of postoperative pain. In: Raj PP, editor. Medicine: A comprehensive review, St Louis, Mosby-Year Book Inc. 1993.
- Kehlet H, Dahl JB. The value of “multimodal” or “balanced analgesia” in postoperative pain treatment. Anesth Analg. 1993;77(5):1048-56.
- Fillingim Rb, Kaplan L, Staud R, Ness TJ, Glover TL, Campbell CM, et al. The A118G single nucleotide polymorphism of the mu-opioid receptor gene (OPRM1) is associated with pressure pain sensitivity in humans. J Pain. 2005;6(3):159-67.
- Klecolt-Glaser JK, Marucha PT, Malarkey WB, Mercado AM, Glaser R. Slowing of wound healing by psychological stress. Lancet. 1995;346(8984):1194-6.
- Broadbent E, Petrie KJ, Alley PG, Booth RJ. Psychological stress impairs early wound repair following surgery. Psychosom Med. 2003;65(5):865-9.