Case Report
A Rare Case of Malakoplakia Masquerading as a Recurrence of Surgically Treated Renal Cell Carcinoma
Matthew Megson*, Suresh Ganta, Jay Khastagir and Sid Singh
Department of Urology, George Eliot Hospital, UK
*Corresponding author: Matthew Megson, Department of Urology, George Eliot Hospital, UK
Published: 24 Aug, 2018
Cite this article as: Megson M, Ganta S, Khastagir J,
Singh S. A Rare Case of Malakoplakia
Masquerading as a Recurrence
of Surgically Treated Renal Cell
Carcinoma. World J Surg Surgical Res.
2018; 1: 1039.
Abstract
A 57 year old woman presented with ongoing pain and a mass in her left loin approximately four
months after undergoing laparoscopic radical nephrectomy because of a left renal mass. She had
a large mass at the site of her resection which continued to grow and cause destruction of bone,
in this case her left sacral wing. However, the histology showed that this was not a recurrence
but Malakoplakia secondary to a wound infection. To the best of our knowledge, Malakoplakia
stemming from a urinary tract source this extensive and including bone destruction, has never been
reported before.
Keywords: Malakoplakia; Multi-disciplinary team; Renal cell carcinoma
Introduction
The current report represents a rare case of malakoplakia which presented after a left-sided laparoscopic radical nephrectomy. Malakoplakia represents a differential diagnosis which needs to be considered in these cases, since despite an appropriate source control with drainage of collections and antibiotics; this type of infection might increase fast and significantly. Finally, the presented woman underwent a surgically open exploration of the left retroperitoneum to exclude recurrent disease (which might not have been necessary if the patient would have been treated with antibiotics adequately, that are highly effective in malakoplakia).
Case Presentation
A 57 year old female initially presented to the Department of Urology of a general district hospital
with visible haematuria and a CT revealed a left renal tumour. Her past medical history included
non-insulin dependent diabetes and hypertension, which were both controlled with medications.
After Multi-Disciplinary Team (MDT) discussion she underwent a left laparoscopic radical
nephrectomy. Histology showed a clear cell renal cell carcinoma, Grade 3 (pT2a N0M0).
Histopathology confirmed there were negative surgical margins. Postoperatively she made an
uneventful recovery and was discharged three days after the operation. Nevertheless, she complained
of ongoing discomfort around her wound and also left sided abdominal pain at the time of discharge.
Almost four months later she presented with severe anaemia and considerably worsened
abdominal pain. On examination a left iliac fossa mass was palpated. CT revealed a 10 cm left psoas
abscess and CT guided drainage was done. After twelve days, she was discharged with the drain-insitu.
The drain was removed after two days, when it was draining sufficiently small amounts.
She re-presented two months after this with worsening pain in the left loin and left iliac fossa
and there was a recurrence of the left iliac fossa mass. She had another CT (Figure 1) that showed
extensive para-aortic lymphadenopathy extending into iliopsoas and left Sacroiliac joint with abscess
formation. Changes were reported to have increased compared to the previous scan. A drain was
inserted on the ward and 200 mls of pus was drained. CT guided biopsy of retroperitoneal mass was
undertaken and histologically a diagnosis of malakoplakia was made. This was the same pathologist
who diagnosed the original cancer after the patient’s nephrectomy. After an inpatient stay for two
weeks, the patient was discharged.
Within a couple of weeks, the patient was readmitted with collapse, general malaise, lethargy
and worsening left loin pain. Despite histologically confirming a diagnosis of malakoplakia, there
was mounting concerns that this was a recurrent tumour. After an MDT discussion the general
consensus was that a proper histological diagnosis was needed before labelling the findings as a
recurrent tumour as it could still be an ongoing inflammatory/infectious process. A repeat CT
biopsy was done which again confirmed malakoplakia. An additional
detailed CT was conducted (Figure 2). This stated that the entire left
rectoperineal area was abnormal with irregular enhancing soft tissue
with extension into left groin pushing iliac vessels medially. This mass
was also extending into the posterior abdominal wall and was causing
destruction of the left sacral wing extending into left sacral iliac joint
and left iliac crest. Additionally, the medial margin of this mass was
abutting the aorta over a long length. From these images it was felt
that this mass represented a huge incurable retroperitoneal renal cell
tumour recurrence complicated by secondary infection.
An open exploration of the left retroperitoneum was done and
findings were of a hard, inflammatory area with no collection to
drain. Extensive biopsies were taken and 200 mls of pus were drained
from a separate gluteal incision. No fungi or acid fast bacilli were seen
on special staining.
The sarcoma unit (a tertiary referral specialist centre unit
specialising in sarcoma) was involved as it was felt she may
have possible osteomyelitis complicating an extensive, invasive
retroperitoneal and a left retro-pelvic mass that was confirmed to be
malakoplakia. Additionally there was continuing evidence of chronic
local sepsis. The sarcoma unit recommended a Contrast CT and
defunctioning colostomy as they had considered the possibility of
bowel leak that was persisting to account for the chronic sepsis. The
CT did not show any colonic leak and therefore no further operations
were undertaken.
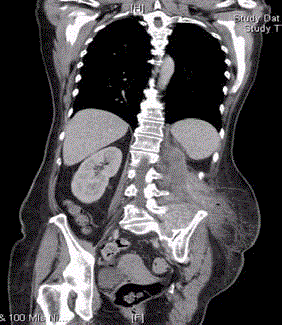
Figure 1
Figure 1
This is a CT slice showing extensive inflammation with paraaortic
lymphadenopathy extending into iliopsoas and left Sacroiliac joint with
abscess formation.
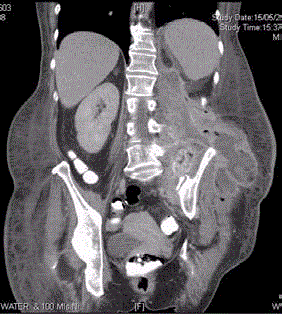
Figure 2
Figure 2
This is a CT slice showing there is an irregular enhancing soft
tissue with extension into left groin pushing iliac vessels medially. This CT
also showed the mass was also extending into the posterior abdominal wall
and was causing destruction of the left sacral wing extending into left sacral
iliac joint and left iliac crest. Additionally, the medial margin of this mass was
abutting the aorta over a long length.
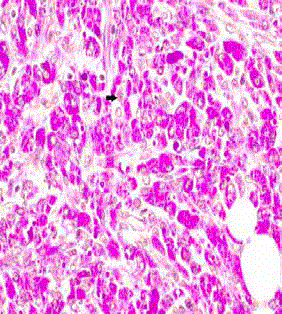
Figure 3
Figure 3
This is a Histology slide of the specimen using the periodic
acid-Schiff stain. This shows Michaelis-Gutmann bodies (histiocytes with
basophilic inclusions with concentric laminations) which are diagnostic.
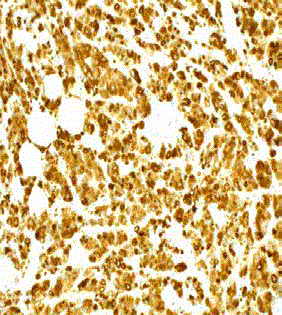
Figure 4
Figure 4
This is an immunohistochemical study of the specimen using
CD68 antibodies. This positive stain for CD68 antibodies suggests that the
Michaelis-Gutmann bodies (which consist of lysosomes filled with partially
digested bacteria) contain gram negative bacteria.
Investigations
The patient’s haemoglobin continued to be low and she required
several blood transfusions. Urine cultures had always shown a
coliform infection and multiple CTs demonstrated that the mass was
increasing in size and causing bone destruction (Figures 1 and 2).
Blood tests were all normal apart from raised inflammatory marker
(CRP), which settled after appropriate treatment.
Histology showed classic Michaelis-Gutmann bodies consistent
with malakoplakia (Figures 3 and 4). There was no positivity for
pan cytokeratin, CK7 or CK20 further confirming there was no
histological evidence to suggest carcinoma. Her cultures from the
biopsies showed coliforms resistant to most oral antibiotics but
sensitive to Ciprofloxacin.
Outcome
During the course of the disease this patient has been treated
with multiple antibiotics, including IV Tazocin and IV Teicoplanin.
However, she did make a good recovery when she was switched to
ciprofloxacin.
The patient had initially reduced mobility and chronic pain
from the bony retroperitoneal involvement. These symptoms all
resolved with minimal sequelae after the appropriate antibiotics and
physiotherapy.
Her follow-up after the Malakoplakia was initially based around
her infection. However, this then returned to her long-term follow-up
which was based on the guidelines for her intermediate risk renal cell
carcinoma, so no follow-up images were taken for her Malakoplakia.
Discussion
Malakoplakia is a chronic granulomatous inflammatory disorder
associated with an infectious etiology [1], usually involving the
urinary bladder, though it has been reported affecting the kidneys,
respiratory system and digestive system [2]. It is often associated with
those patients who are immunocompromised, either iatrogenically
by immunosuppressant drugs (e.g. post-transplant) or secondary to
their co morbidities (e.g. Diabetes, malignancy, immune deficiency
states, and alcohol abuse) [3]. Clinically, as well as radiologically
malakoplakia produces tumour‐like nodules that are able to mimic
malignant neoplasms, thus a confirmation of the diagnosis can only
be achieved histologically [4].
Since its original description in 1901 by von Hansemann [5], over
400 cases of Malakoplakia have been reported. The reason an infective
source has been linked to malakoplakia is twofold: first, within the
cytoplasm of macrophages large calcified structures called Michaelis‐
Gutmann bodies are present, which are believed to develop as a
result of ineffective digestion of bacteria [3]. Second, when examined
with an electron microscope you can find coliform bacteria within
phagolysosomes of these macrophages we have described above [4].
This is obviously not the whole story, as although having a UTI’s in
the UK with E. coli is common, malakoplakia is rare, therefore there
has to be another reason for this condition to occur.
There is still uncertainty about the pathogenesis of the disease,
however one theory is that there are defective killing and impaired
digestion of phagocytosed bacteria [6]. This is suggested by the
characteristic intracellular abnormalities within the macrophages
[4]. Ciprofloxacin is more effective in this condition as unlike other
antibiotics which are effective on E. coli, ciprofloxacin has shown to
penetrate well into macrophages [4].
Malakoplakia that involves the urinary tract has a 4:1 female
predominance with a peak incidence of over 40 years [7,8].
Relevant common laboratory findings include anaemia. The clinical
presentation is variable and non-specific, however most commonly
these patients present with flank pain, fever and a palpable abdominal
mass [3].
Due to the clinical and radiological appearance mimicking
neoplasia then it is important to get a histological diagnosis.
Malakoplakia managed medically with antibiotics, therefore avoiding
the complications and morbidities, as well as the risk of mortality,
which are associated with a nephrectomy.
Learning Points
1. Malakoplakia can masquerade as cancer on radiological
appearances and early biopsy to confirm the diagnosis is important
to ensure early treatment like antibiotics, esp. ciprofloxacin, which is
very efficacious in Malakoplakia as in the case above.
2. Awareness that surgical site infection could cause
Malakoplakia, which is a rare, unreported post-operative infective
complication of a laparoscopic nephrectomy for cancer.
3. To be aware that malakoplakia of urinary tract origin can
result in severe, extensive retro-peritoneal malakoplakia involving
bone. This has not been reported before.
References
- Hegde S, Coulthard MG. End stage renal disease due to bilateral renal malakoplakia. Arch Dis Child. 2004;89(1):78-9.
- Puerto IM, Mojarrieta JC, Martinez IB, Navarro S. Renal malakoplakia as a pseudotumoral lesion in a renal transplant patient: A case report. Int J Urol. 2007;14(7):655-7.
- McKeen SK, Tie ML. Renal parenchymal malakoplakia: An unusual case of unilateral, diffuse renal enlargement. Australas Radiol. 2002;46(1):69-72.
- Van Furth R, Van’t Wout JW, Wertheimer PA, Zwartendik J. Ciprofloxacin for treatment of malakoplakia. Lancet. 1992;339(8786):148-9.
- van der Voort HJ, ten Velden JA, Wassenaar RP, Silberbusch J. Malakoplakia. Two case reports and a comparison of treatment modalities based on a literature review. Arch Intern Med. 1996;156(5):577-83.
- Merritt AJ, Thiryayi SA, Rana DN. Malakoplakia diagnosed by fine needle aspiration (FNA) and liquid-based cytology (LBC) presenting as a pararenal mass in a transplant kidney. Cytopathology. 2014;25(4):276-7.
- Stanton MJ, Maxted W. Malakoplakia: A study of the literature and current concepts of pathogenesis, diagnosis and treatment. J Urol. 1981;125(2):139-46.
- Dasgupta P, Riddick T, Womack C, Turner AG, Blackford HN. Malakoplakia: The history of a curious disease. J Urol. 1998;159:508A.