Research Article
Staged Closure of Gastroschisis using Alexis Wound Retractor and Protector
Achariya Tongsin*, Rangsan Niramis, Veera Buranakitjaroen, Varaporn Mahatharadol, Wannisa Poocharoen and Suranetr Laorwong
Department of Surgery, Queen Sirikit National Institute of Child Health, Thailand
*Corresponding author: Achariya Tongsin, Department of Surgery, Queen Sirikit National Institute of Child Health, Bangkok, 10400, Thailand
Published: 15 Aug, 2018
Cite this article as: Tongsin A, Niramis R, Buranakitjaroen
V, Mahatharadol V, Poocharoen W,
Laorwong S. Staged Closure of
Gastroschisis using Alexis Wound
Retractor and Protector. World J Surg
Surgical Res. 2018; 1: 1036.
Abstract
Background: Gastroschisis is the most common congenital anterior abdominal wall defect. The
principle of management is to reduce the eviscerated content safely and to close the abdominal wall
defect with an acceptable cosmetic appearance.
Objectives: Compare the using of Steri-drape Artificial Sac (SAS) and Alexis Wound Protector and
Retractor (AWR) for staged closure of gastroschisis.
Methods: A retrospective study of patients with gastroschisis who were treated by staged closure
at Queen Sirikit National Institute of Child Health between January 2013 and December 2016 was
conducted. Patient’s information was compared between the usage of SAS and AWR regarding
demographic data, operative procedure and results of treatment. The statistical differences were
analyzed by the Chi-square, Fisher exact and student t-test with p-value less than 0.05 considered
significant. Patients who had associated intestinal atresia or perforation were excluded.
Results: Eighty-four patients with gastroschisis were treated by staged closure (SAS: 39, AWR:
45). Average gestational age, birth weight, maternal age and defect size in both groups were not
significantly different (p>0.05). AWR placements were performed at bedside 33 cases, in the
operating room 7 cases. The AWR group had shorter operative time for placement and abdominal
wall closure than SAS group significantly (p< 0.001). Regarding duration of parenteral nutrition,
duration of ventilator support and length of stay, significantly shorter in the AWR group (p< 0.05).
There were no complications attributed to AWR placement.
Conclusion: Staged closure of gastroschisis with AWR is simple, convenient and safe technique, in
addition, to avoid anesthetic risk in the first day of life and good cosmetic appearance.
Keywords: Gastroschisis; Staged closure; Steri-drape artificial sac; Alexis wound protector and
retractor; Surgical management
Introduction
Gastroschisis is a fully thick defect of the abdominal wall with herniation of a variable amount
of uncovered intestinal loops through a defect immediately to the right of a normally formed
umbilicus. The intestine is frequently foreshortened, covered with gelatinous exudates, matted
together, and edumacated due to its exposure to amniotic fluid and compression of the mesenteric
blood supply at the defect.
The management of gastroschisis has gradually evolved and improved over the years. The
principles of management, however, remain the same: to reduce the viscera safety, to close the
abdominal wall defect with an acceptable cosmetic appearance, and proper nutrition support, in
addition to detection and proper management of any associated anomalies or complications [1].
The safety of reduction and closure techniques are related to the level of Viscera Abdominal
Disproportion (VAD). When primary reduction and facial closure under general anesthesia
is impossible due to VAD and intra abdominal hypertension, staged closure with a silo is
recommended. Surgical silo was created using a variety of materials (e.g., Prolene, Silastic, steridrape
and stockinette or intravenous infusion bag) [2-6]. The surgical silo with no suture is used in
most Western setting. However, it is not performed in Thailand where the current procedure is a
Steri-drape Artificial Sac (SAS) sutured directly to all layers of the abdominal wall circumferentially
around the defect under general anesthesia.
The aim of this study is to compare the usage of SAS and Alexis
Wound protector and Retractor (AWR) for staged closure of
gastroschisis.
Figure 1
Material and Methods
After obtaining approval from the institutional Research Ethics
Committee, a retrospective review was performed of all patients with
gastroschisis who treated by staged closure at Queen Sirikit National
Institute of Child Health (QSNICH) between January 2013 and
December 2016.
Surgical techniques
Initial management aimed at maintaining circulation to the bowel
and preventing infection by covering the defect with sterile dressing
soaked in warm 0.9% normal saline to prevent fluid loss, stabilization
infants within appropriate temperature, gastric decompression, and
intravenous fluid with glucose and broad-spectrum antibiotics. After
stabilization of the infants in the neonatal surgical unit, the herniated
viscera was inspected and assessed for proper reduction method. The
decision of primary closure was based on the size of the herniated
viscera and the size of the abdominal cavity.
When primary closure was not possible due to the presence of
discrepancy between the size of the herniated viscera and the volume
of the abdominal cavity, a staged reduction of the herniated viscera
and delayed closure of the abdomen was considered, then the silo
pouch was fashioned by one of two methods as followed by the
responsible surgeons. Half of the surgeon’s preferred SAS and the
other half preferred AWR.
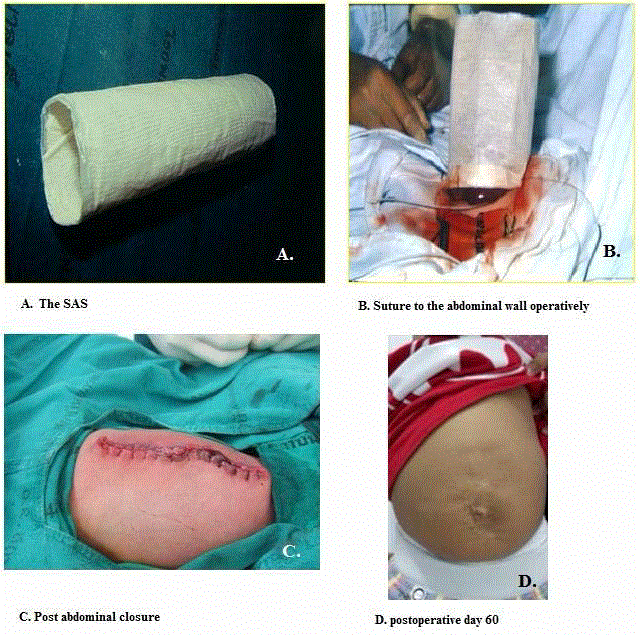
1. A Steri-drape Artificial Sac (SAS) used at QSNICH was described
by Havanonda et al. [5] and Havanonda [6]. It is made of a stockinette
pouch which is lined both inside and outside with steri-drape. The
abdominal wall defect was extended upwards and downwards 2 cm
to 3 cm. in order to prevent of obstruction during bowel reduction.
The SAS was placed to cover over the herniated viscera and the defect.
Continuous suturing was approximated between the SAS and all
layers of the abdominal defect by non-absorbable sutures (2-0 nylon),
the upper limit of the SAS was closed with a simple tie with umbilical
tape and the base was closed with gauze soaked in povidone iodine
solution, as shown in (Figure 1). This procedure was done in the
operating room under general anesthesia. In the second postoperative
day the herniated viscera was manually reduce and daily cot-side
reduction. When the viscera had been complete reduce, fascial and
skin closure were achieved at a second anesthetic. The fascia defect
was closed vertically with interrupted 2-0 polyglactin sutured and
the skin was trimmed and approximated by interrupted stitches with
umbilical cord preservation.
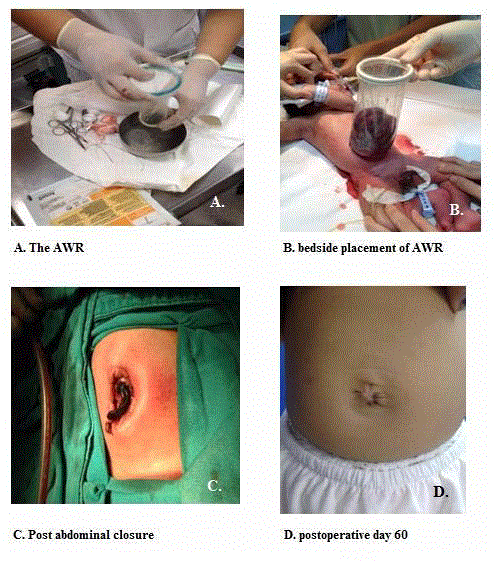
2. Alexis® Wound Retractor and protector (AWR) device (Applied
Medical Resources Corp. USA) is a commercial wound protector and
retractor system, made from polyurethane which is used for open
laparotomy and hand-assisted laparoscopic surgery to protect the
wound and is considered to be low reactivity to human tissue [7]. The
AWR consisted of two rings, an elastic white one and elastic green
one, a transparent rubber cylinder connects the two rings. This device
is available in different diameters. We used the sizes XS with the ring
diameter of 4 cm (Figure 2). At the bedside under aseptic precaution, the
AWR placement was performed. The herniated viscera were inserted
into the retractor through the green ring, and then the bottom ring
was placed into the peritoneal cavity through the gastroschisis defect
without suturing to the fascia defect. Adhesion from the fascia to the
bowel wall was gently disrupted manually. In case of dense adhesions
to the bowel wall or very small gastroschisis defect, AWR placement
was performed in the operating room under general anesthesia. Some
time, because of the very small defect, a small skin incision in the
midline is required for ring insertion. The diameter of the internal
ring of AWR was not reduced as described in Japanese report [8].
The white ring is then gently lifted; avoid any leakage of peritoneal
fluid out of the peritoneal cavity. The base of the AWR was closed
with gauze soaked in povidone iodine solution and its upper limit
was closed with a simple tie with umbilical tape. Over the next 2 days,
the herniated viscera was gradually integrated the abdominal cavity,
the cylinder was reduced with repeated tying until complete bowel
reduction was obtained within 7 days. Following complete reduction,
the patients were returned to the operating room and abdominal
defect was closed under general anesthesia as follows. Firstly, the
AWR was removed without any difficulty then the peritoneum and
fascia was approximated with interrupted 2-0 polyglactin sutured and
the skin was closed with umbilical cord preservation.
Antibiotics were administrated for 14 days, local wound care was
performed. Feeding was commenced once nasogastric aspiration
has become minimal and clear, patients were discharge home when
feeding was full established.
Each patient was evaluated with regard to time to closure of the
abdominal wall, time to initiating enteral feeds, time to full feeds,
hospital course and any complications.
Figure 2
Table 1
Table 2
Data Analysis
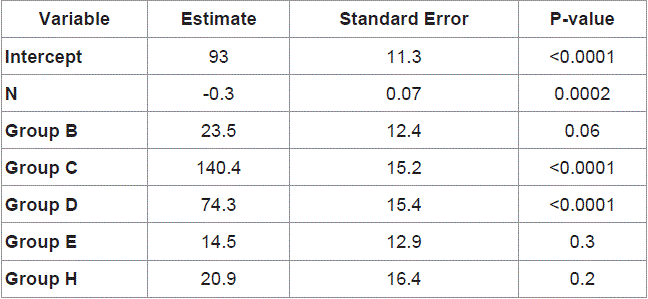
Information evaluation included demographic data, technique of abdominal closure, and time interval to the first feeding, time interval to the full feeding, duration of Parenteral Nutrition (PN), Length of Hospital Stay (LOS) and result of treatment. Data is presented as mean, median, percentage and range. Mean comparisons used unpaired Student’s t-test, unequal variances. Continuous data with skewness distribution comparisons used Willcoxon rank sum test. A p-value less than 0.05 were considered significant. Data processing was aided by the SPSS program version 20.0.
Results
Perinatal data
Between 2013 and 2016, 155 neonates with gastroschisis were
referred to Queen Sirikit National Institute of Child Health. Ninetysix
patients were treated by staged closure, 12 patients had associated
intestinal atresia or perforation and were excluded from this study.
Eighty-four patients were evaluated.
Demographic data are highlight in Table 1. There were no
difference (p>0.05) concerning gender, antenatal diagnosis by
ultrasonography, gestational age, birth weight, maternal age, modes
of delivery, birth order of the mother and defect size.
Operative procedures
Eighty-four cases of gastroschisis underwent staged closure
procedure. Thirty-nine cases had SAS placement and 25 cases were
performed at night time. Forty-five cases had AWR placement,
AWR was inserted bedside in the neonatal surgical unit without
general anesthesia or sedative drug in 33 cases. Seven cases had a
dense adhesion from abdominal wall to the bowel wall and 5 cases
had a very small opening so AWR placements were performed in the
operating room to allow lyses of adhesions or widening of the fascial
defect with short operative time. Postoperatively, the daily dressing
changes were performed in the neonatal unit. The eviscerated bowels
were manually reduced in the second postoperative day. The average
time for complete reduction was 8.0 days (6-15) and 7.7 days (5-20)
for SAS and AWR respectively (p=0.401). Three cases that underwent
AWR placement in the operation room and widening of the defect
had AWR dislodgement on third and fourth day after placement
and replacement of AWR was performed in the operating room. The
final staged, abdominal closure and umbilical preserved procedure in
the operating room under general anesthesia were performed. The
mean operative time in SAS and AWR were 65.8 (35-155) and 24.5
(25-65) minutes (p< 0.01), respectively. The AWR group had shorter
operative time for placement and abdominal wall closure than SAS
group significantly (Table 2).
Functional outcome measures were the mean time of first oral
feeding and full feeding, duration of Parenteral Nutrition (PN),
duration of ventilator support and length of stay. The duration from
closure of abdomen to the first day of oral feeding range from 18-77
days (average 27.9) in SAS group and 14-40 days (average 22.7) in
AWR group (p=0.027). The AWR group had earlier initial of enteral
feeding, short duration of PN, short duration of ventilator support
and short length of stay than SAS group significantly.
Septicemia occurred in 25% (n=10) in SAS group and 11.1% in
AWR group (Table 3). The rate of NEC was 10% (n=4) in SAS group
and 6.6% (n=3) in AWR group. Six wound infections were identified
in each group. There was 1 death in this study, in detail; a 2,200
gm female was born at 36 weeks gestation by spontaneous vaginal
delivery, APGAR 8, 9. She underwent SAS placement at age three
hour post-delivery and abdominal wall closure at age seven days.
However, at age of thirteen days, she was respiratory distress and
developed respiratory failure. She ran down and died of septicemia
bilateral pneumonia (K. pneumoniae).
Mean time of follow-up was 11 months (range 2 to 48 months).
All patients had a normal weight gain. One case in SAS group
underwent reoperation due to adhesive small bowel obstruction at
22 months old. At one year follow up, four cases in SAS group had
a small umbilical hernia and three cases in AWR group had a small
umbilical hernia that resolved during follow-up. The AWR group
had less surgical scar and cosmetically acceptable appearance of the
umbilicus.
Table 3
Discussion
Gastroschisis is the most common congenital abdominal wall
defect. The incidence of gastroschisis is rising over the last decade. It
has been estimated between 4 to 10 in 10,000 live births [9-12].
There are five key consideration of surgical management of
gastroschisis patients,
1. Reduce the evisceration safely,
2. Close the defect with a cosmetically acceptable outcome,
3. Identify and treat the associated anomalies,
4. Support nutrition until full independent enteral feeding is
established and
5. Recognize and treat abdominal, wound or bowel
complications [13].
In 1943, Watkins [14] reported the first successful primary
closure of gastroschisis.
In 1975, Shermata and Haller [15] used a performed transparent
silo sutured to the abdominal wall. The silo was suspended to allow
relief of bowel edema and also to allow a gradual reduction of the
viscera into the abdominal cavity.
In 1995, Fischer [2] used a silastic silo (Dow Corning, Midland,
MI) with a spring-loaded ring (Ben Tec, Sacramento, CA) to place
over the exposed viscera, under the fascial defect without suturing,
performed under sterile condition in the NICU with patient sedation.
The current method of treatment has change to the use of sutureless
performed silo [16,17].
In Thailand, silastic sheet, spring loaded silo and sutureless silo
is not available. In 1971, Havanonda [5,6] performed a steri-drape
artificial sac which made from steri-drape and stockinette sutured
directly to all layers of the abdominal wall circumferentially around
the defect. This procedure was performed in the operating room
under general anesthesia and left a long vertical surgical scar.
The use of AWR was first described in 2005 by Kusafuka et al. [8],
as the usual spring-loaded silo was not available in Japan. AWR was
used as a protective silo for staged closure of gastroschisis after having
reduced the diameter of the internal ring. Four years later, Ogasawara
et al. [18] reported the using of AWR in 7 patients. In 2014, Ferreira et
al. [19] reported the used of AWR for staged closure of gastroschisis
in 8 patients. All previous reports, AWR placement were performed
in the operating room under general anesthesia [19].
This study was the first and largest published series of AWR
for staged closure of gastroschisis in Thailand. The procedure was
performed at bedside; avoid the need for first day surgery and general
anesthesia. We usually used the size XS with the ring diameter of 4 cm.
The ring can fit appropriately without urine retention or respiratory
complication.
In the case that had a dense adhesion from abdominal wall to
the bowel wall or a very small defect, we recommended to performed
AWR placement in the operating room to prevent further injury to
the eviscerated organs.
Although in 12 patients, the AWR placements were performed
in the operating room under general anesthesia it’s took shorter
operative time than when performed SAS, which is a significant
advantage. Three cases had AWR dislodgement, the causes of
AWR dislodgement were widening of the all layers of the defect in
placement procedure and shearing force when reduction the visceral
content. Prevention could be divided only sheath when placement,
care the AWR in central position of the defect and gradual reduction
without traction the AWR. The gradual reduction of the viscera with
the AWR minimized the risk for intra abdominal hypertension and
visceral discoloration. The transparent nature of the AWR allows
monitoring of visceral color that is not possible when SAS has been
applied.
This study has limitations. Most importantly, the patients of each
groups were not randomized due to it is a retrospective in nature.
The surgical techniques were chosen by the responsible surgeons.
Half of the surgeons preferred SAS, and the other half who concerned
about general anesthesia in the first day of life preferred AWR. The
responsible surgeons have preference of surgical technique regardless
of the patient’s condition.
We have demonstrated that placement of AWR device is feasible
at the bedside in most infants (73% in this series), without the need
for general anesthesia or sedation. This can preclude the need for “out
of hours” operation, avoid surgery and general anesthesia on the first
day of life. Comparison between cosmetic outcome of SAS and AWR,
the AWR group had less surgical scar and cosmetically acceptable
appearance of the umbilicus. Overall outcomes of AWR used are
reviewed in Table 4.
Table 4
Conclusion
The staged closure of gastroschisis with AWR is a simple, convenient and safe technique. The advantage of AWR use are reduce number of time to operation of patients, decrease anesthetic risk in the first 24 hour of life, reduce night time workload of physician, shorter length of stay when compare with the traditional method and in addition to being good cosmetic appeal. We concluded that AWR is to be an effective alternative and recommended device to use for staged closure of gastroschisis.
Acknowledgement
The authors wish to thank Dr. Somkiat Lalitwongsa, the Director of Queen Sirikit National Institute of Child Health for permission of publication and Dr. Jarruphong Noitumyae for supporting of statistical analysis.
References
- Owen A, Marven S, Johnson P, Kurinczuk J, Spark P, Draper ES, et al. Gastroschisis: a national cohort study to describe contemporary surgical strategies and outcomes. J Pediatr Surg. 2010;45(9):1808-16.
- Fischer JD, Chun K, Moores DC, Andrews HG, Linda L. Gastroschisis: a simple technique for staged silo closure. J Pediatr Surg. 1995;30(8):1169-71.
- Lansdale N, Hill R, Gull-Zamir S, Drewett M, Parkinson E, Davenport M, et al. Staged reduction of gastroschisis using performed silo: practicalities and problems. J Pediatr Surg. 2009;44(11):2126-9.
- Allotey J, Davenport M, Njere I, Charlesworth P, Greenough A, Ade-Ajayi A, et al. Benefit performed silos in the management of gastroschisis. Pediatr Surg Int. 2007;23(11):1065-9.
- Havanonda S, Suwatanaviroj A, Wattanatittan S, Viravaidhaya D. Gastroschisis. In: Havanonda S, Sutthiwan P, Thitawat W, Prachuabmoh K, Panichkul C, Hongprapas C, editors. Progress in Surgery Series of the Royal College of Surgeons of Thailand. Vol 3. Bangkok: Bangkok Medical Publisher; 1982. p. 79-94.
- Havanonda S. Omphalocele and gastroschisis. Bangkok: Unity Publication; 1989. p. 39-42.
- Edwards JP, Ho AL, Tee MC, Dixon E, Ball CG. Wound protectors reduce surgical site infection: a meta-analysis of randomized controlled trials. Ann Surg. 2012;256(1):53-9.
- Kusafuka J, Yamataka A, Okazaki T, Okawada M, Urao M, Lane JG, et al. Gastroschisis reduction using “Applied Alexis”, a wound protector and retractor. Pediatr Surg Int. 2005;21(11):925-7.
- Niramis R, Suttiwongsing A, Buranakitjaroen V, Rattanasuwan T, Tongsin A, Mahatharadol V, et al. Clinical outcome of patients with gastroschisis: What are the differences from the past? J Med Assoc Thai. 2011;94(Suppl 3):S49-56.
- Holland AJ, Walker K, Badawi N. Gastroschisis: an update. Pediatr Surg Int. 2010;26(9):871-8.
- Parker SE, Mai CT, Canfield MA, Canfield MA, Richard R, Wang Y, et al. Updated national birth prevalence estimates for selected birth defects in the United State, 2004-2006. Birth Defects Res A Clin Mol Teratol. 2010;88(12):1008-16.
- Mortellaro VE, St Peter SD, Fike FB, Islam S. Review of the evidence on the closure of abdominal wall defects. Pediatr Surg Int. 2011;27(4):3917.
- Marven S, Owen A. Contemporary postnatal surgical management strategies for congenital abdominal wall defect. Semin Pediatr Surg. 2008;17(4):222-35.
- Watkins DE. Gastroschisis. Virginia Med Month. 1943;78:42-3.
- Shermata DW, Haller JA Jr. A new performed transparent silo for the management of gastroschisis. J Pediatr Surg. 1975;10(6):973-5.
- Owen A, Marven S, Jackson L, Antao B, Roberts J, Walker J, et al. Experience of bedside performed silo staged reduction for gastroschisis. J Pediatr Surg. 2006;41(11):1830-5.
- Pastor AC, Philips JD, Fenton SJ, Meyers R, Lamm AW, Raval MV, et al. Routine use of a silastic spring-loaded silo for infants with gastroschisis: a multicenter randomized controlled trial. J Pediatr Surg. 2008; 43(10):1807-12.
- Ogasawara Y, Okazaki T, Kato Y, Lane GJ, Yamataka A. Spontaneous sutureless closure of the abdominal wall defect in gastroschisis using a commercial wound retractor system. Pediatr Surg Int. 2009;25(11):973-6.
- Ferreira CG, Lacreuse I, Geslin D, Schmitt F, Schneider A, Podevin G, et al. Staged gastroschisis closure using Alexis wound retractor: First experiences. Pediatr Surg Int. 2014;30(3):305-11.
- Machida M, Takamizawa S, Yoshizawa K. Umbilical cord inverting technique: A simple method to utilize the umbilical cord as a biological dressing for sutureless gastroschisis closure. Pediatr Surg Int. 2011;27(1):95-7.