Research Article
First 200 Robotic General Surgery Cases in a Community Hospital: A Retrospective Cohort Study
Rodolfo J Oviedo, MD, FACS, FASMBS1*, Naomi C Brownstein, PhD2, SchMiyah L Smith, MD1, Jarrod C Robertson, MD1 and Sangeeta Nair-Collins, MD, PhD1
1Department of Surgery, Florida State University College of Medicine, USA
2Department of Behavioral Sciences and Social Medicine, Florida State University College of Medicine, USA
*Corresponding author: Rodolfo J Oviedo, MD, FACS, FASMBS, Department of Surgery, Valley Health Metabolic & Bariatric Program, Winchester Medical Center 1870 Amherst Street, Suite F Winchester, Virginia, 22601, USA
Published: 08 Aug, 2018
Cite this article as: Oviedo RJ, Brownstein NC, Smith SL,
Robertson JC, Nair-Collins S. First
200 Robotic General Surgery Cases in
a Community Hospital: A
Retrospective Cohort Study. World J
Surg Surgical Res. 2018; 1: 1034.
Abstract
Background and Objectives: A retrospective series and learning curve of the first 101 robotic
general surgery cases from a single surgeon in a small community hospital has been previously
reported. This study serves as a continuation and offers a more detailed statistical analysis while
demonstrating the efficacy and safety of a general surgery robotics program in a community hospital
with quality assessment measures.
Methods: Measurements included total operative time, console time, conversion rates,
complications, surgical site infections, surgical site occurrences, length of stay, and patient
demographics. Descriptive statistics were included for all variables. Linear regression was used to
test the hypothesis of a learning curve, reflected by a decrease in console time with experience.
Results: Between March 2014 and February 2017, 200 robotic general surgery cases were
performed by a single surgeon in a 266-bed community hospital, including laparoscopic
cholecystectomies; ventral, incisional, and umbilical hernia repairs; colorectal; foregut and
bariatric; inguinal hernia repairs; and miscellaneous procedures. One hundred and ninety-eight of
the cases (99%) were completed robotically. Thirteen patients were readmitted within 30 days, and
21 had complications (11%). There were no mortalities, and all complications were resolved
positively. The mean operative and console times of all 200 cases were 214.8 and 105.7 minutes,
respectively. Decreased console time was significantly associated with increasing case load, even
after controlling for surgery type.
Conclusion: With increased operative volume, general surgeons who utilize the robotic platform
can improve operative outcomes, decrease operative times and perform increasingly complicated
procedures while maintaining low complication rates.
Keywords: Community hospital; General surgery; Robotic surgery; Learning experience;
Outcomes
Introduction
The da Vinci Surgical System (Intuitive Surgical, Inc. Sunnyvale, California, USA) was approved
by the U.S. Food and Drug Administration (FDA) in 2000, with early applications for heart surgery,
cholecystectomy, and Nissen fundoplication [1,2]. Within general surgery, applications have
expanded to colorectal surgery, abdominal wall reconstruction, and bariatric surgery.
While opposition to the use of robotic technology in general surgery has slowly decreased, there
is some resistance based on concerns regarding an overuse of resources. Proponents of the robotic
platform cite enhanced visualization, improved instrument dexterity, and increased surgeon control
as advantages [3]. The use of the da Vinci surgical system for single site cholecystectomy was first
reported in large American and European academic medical centers in 2011 [4,5]. Since this time,
many groups have shown single site cholecystectomy to have minimal complications and good
outcomes [6,7].
Reductions in postoperative pain, complication rates, and recovery time served as the foundation
for the transition from open to laparoscopic ventral hernia repair, which was first performed in
1992 [8,9]. The advent of the robotic platform offered the same advantages as the laparoscopic
technique, with some studies showing the additional benefit of a greater decrease in pain by avoiding
trans-fascial sutures, and a greater ease of mesh implantation [10,11]. Most inguinal hernias still
continue to be repaired open rather than laparascopically [12]. Several single surgeon reports exist
documenting successful robotic inguinal hernia repair [6,13,14].
After the first reports of telerobotic-assisted laparoscopic
colectomies in 2001 [15] robotic colorectal surgery has been shown
to have efficacy similar to that of conventional laparoscopy [16].
The robotic technology has potentially augmented benefits in rectal
and oncologic surgery secondary to fine visualization and enhanced
dexterity crucial to the efficacious manipulation in small operative
fields where precision with tissue manipulation is crucial [17,18].
Regarding foregut and bariatric surgery, the first reported robotassisted
bariatric procedure, gastric banding, occurred in 1998 [19].
Since then, robotic systems have also been applied to sleeve gastrectomy
and Roux-en-Y gastric bypass [20]. Robotic Nissen fundoplication
has a positive role in repair of hiatal hernia and surgical management
of gastroesophageal reflux disease. Although a 2013 meta-analysis on
robotic and laparoscopic Nissen fundoplication found no significant
difference in outcomes, a review article reports a general consensus
from 16 published papers supporting the use of robotics for complex
surgeries or redo procedures [21,22]. The first major reports on the
successful implementation of robotic technology in the surgical
management of achalasia presented no instances of esophageal
perforation with robotic Heller myotomy compared to an incidence
rate of 5% to 10% with laparoscopic Heller myotomy [23-25].
Aim and Objectives
In 2016, we described the outcomes of the first robotic general surgery case series in an American community-based, non-tertiary hospital performed by a single surgeon [6]. The present paper is a follow-up study. We have further examined our minimally invasive robotic surgery program with the primary aim to evaluate for safety in terms of review of complications. Our secondary objective was to test for an improvement over time in key surgical outcomes to demonstrate that robotic general surgery can be successfully implemented in a community hospital with appropriate training of the surgeon and the surgical team. With increasing number of cases, both in volume and complexity, the surgeon and the team gain valuable experience that contributes to better outcomes. The previous retrospective review series of 101 cases suggests that this experience may lead to a decrease in console time; the present paper tests this hypothesis.
Materials and Methods
Under approval from the Capital Regional Medical Center
Institutional Review Board, we performed a single-center
retrospective chart review and analysis of the first 200 robot-assisted
general surgery cases completed by a single surgeon in a 266-bed
acute care community hospital. Electronic medical records and
operative logs were reviewed corresponding to the surgeon’s first 139
cases completed with the da Vinci S system from March of 2014 to
August of 2015, and 61 cases completed with the da Vinci Si system
from August 2015 to February 2017. There was no exclusion criteria.
The data is being reported utilizing the Strengthening The Reporting
Of Cohort Studies in Surgery (STROCSS) criteria [26].
Surgical technique
The first 139 surgeries in this retrospective series were performed
using the da Vinci S surgical system, which consists of four
components: the patient-side cart, the EndoWrist instruments, the
surgeon console, and the vision system. The patient-side cart at the
side of the operating table is composed of three or four robotic arms,
one which holds the camera system. The remaining robot arms can
be fitted with various surgical EndoWrist instruments mounted
to trocars to enable the surgeon to dissect, cut, retract, clamp, and
suture with a broader range of motion as compared to open and
laparoscopic surgery. In addition to the expected duties, the surgical
first assistant at the bedside is tasked with exchanging the surgical
instruments at the surgeon’s request. The surgeon console includes
a binocular stereoscopic viewer that delivers images from the two
5 mm cameras docked on one of the arms of the patient-side cart,
producing a 3-dimensional image with up to 10x magnification. The
surgeon controls the robot from the master controls mounted to
the surgeon console. The 5 mm cameras also relay information to a
processing center displaying the surgeon’s view on a high-definition
screen within the operating room to the benefit of the first assistant
[27].
The remaining 61 surgeries in this report were performed using
the da Vinci Si surgical system. The overall set-up is similar to that
of the S system, but it is important to note new features such as the
motorized patient-side cart, a one-piece sterile drape, and the ability
to have a single-site configuration feature introduced to increase the
efficiency of the system [27]. Both the da Vinci S surgical system and
the da Vinci Si surgical system have been shown to be safe surgical
options across many surgical specialties including general surgery [1-
25,28-32].
Data analysis
SAS version 9.4 (SAS Institute, Cary, North Carolina, USA) was
used for statistical analysis. Descriptive statistics are provided on
demographic and other clinical variables, such as length of hospital
stay. Means, medians, standard deviations, quartiles, and ranges are
provided for continuous variables, and frequencies are provided for
categorical variables. Safety was measured using complication rates,
readmissions, and 30 day morbidity, noting how they compare to
standards of rates for laparoscopic surgery. For hernias, recurrence
was examined. Linear regression models were fit for console time
using backward selection with case number, surgical type (described
below) and American Society of Anesthesiologists (ASA) physical
status classification as potential covariates. To test the hypothesis that
console time decreases with increasing experience, we examined the
magnitude and significance of the coefficient for case number, using
a two-sided test at the Bonferroni-adjusted 5% level.
Results
Between March 2014 and February 2017, 200 robotic general
surgery cases were performed by the first author of this paper at
Capital Regional Medical Center in Tallahassee, Florida, USA. The
data collected were analyzed after the cases were divided into the
following 6 groups by type of surgery performed. Group A:
Cholecystectomy (n=28), Group B: Ventral, Incisional, Umbilical
Hernia (n=60), Group C: Colorectal (n=28), Group D: Gastric,
Esophageal, Bariatric (n=21), Group E: Inguinal Hernia (n=45),
Group H: Multiple Procedures (n=18). Surgery types are similar to
our previous report with a few exceptions [6]. In this report, we have
combined foregut and bariatric procedures into a single group
(group D). Surgeries that included multiple procedures, e.g.,
cholecystectomy and umbilical hernia repair performed during the
same operation, were categorized into a separate group (group H).
Descriptive statistics are provided in (Tables 1 and 2) for
continuous and categorical variables, respectively. The patients
averaged 53 years of age and were evenly matched by gender. The
mean Body Mass Index (BMI) of the patients was 31.6 kg/m2. Most
patients (over 90%) were in the ASA II or III classification.
Robotic surgery times ranged from 74 minutes to 722 minutes,
including 41 minutes to 677 from cut to close, and 29 minutes to
525 minutes on the console. The mean (standard deviation) robotic
surgery times for all cases irrespective of category were 214.8 (90.3)
minutes for total operative time, 158.9 (91.1) minutes for cut to close
and 105.7 (66.6) minutes of surgeon console time. The median robotic
surgery times were 188.5 minutes for total operative time, 133.5
minutes for cut to close and 85 minutes of surgeon console time.
Surgical outcomes were positive. Of the 200 procedures, 198 were
completed robotically. Nearly half (96 patients, or 48%) of surgeries
were outpatient, over three-quarters required no more than two days
in the hospital, and over 90% required no more than 4 days. Overall,
there was a complication rate of 11% (21 complications), including
to open, re-admission within 30 days, 30 day morbidity,
Surgical Site Infections (SSI), Surgical Site Occurrence (SSO), blood
transfusions, and recurrence if applicable. Overall, 13 patients were
readmitted to the hospital within 30 days. There were no mortalities
in any of the groups, and all complications were resolved on followup
with good outcomes.
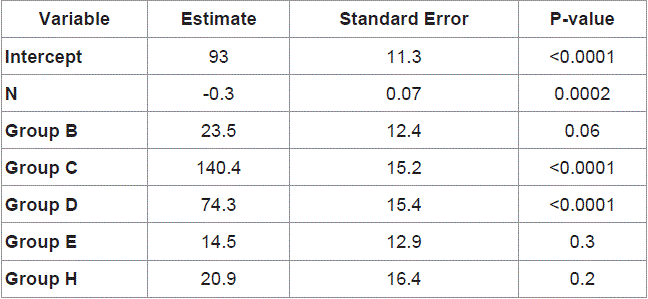
The linear regression parameter estimates modeling the console
times adjusted for surgery group and patient number are provided
in (Table 3). The estimates in Table 3 for groups B-H denote the
expected difference between a surgery in that group compared to a
hypothetical surgery in Group A conducted at the same time. ASA
class was not included because it was not associated with console
time after adjusting for surgery group and patient number. On the
other hand, surgery group was strongly associated with console time
(p < 0.0001). Cholecystectomy (group A), the reference group, took
the shortest time on average, and Colorectal (group C) took the most
console time, followed by Gastric/Esophageal/Bariatric (group D).
Console times were similar for groups B, E, and H, all of which involve
hernia procedures. After adjusting for surgery group, console time
was also associated with case load; average console time dropped by
0.3 minutes per case over the course of the study (p=0.0002). Similar
results (not shown) held for total operative time and cut to close
time, even though only the surgeon at the console was constant for all
procedures; operating room teams varied throughout the study. The
model demonstrated that surgical time decreased over time, as the
surgeon gained experience and grew more proficient at the reported
robotic procedures.
Group A: Cholecystectomy
This group consisted of 28 robot assisted cholecystectomies
performed from March 2014 through February 2017. Twenty-one of
these were completed using the multi-port technique on 6 male and
15 female patients with a mean age of 45.8 years. The mean BMI was
32.4. The mean total operation time was 174.1 minutes with a mean
console time for the multi-port cholecystectomies of 79.2 minutes.
There were 3 complications in this group, occurring in the 2nd, 6th
and 17th multi-port laparoscopic cholecystectomy. One was due to a
superficial accidental thermal injury to the gastric wall serosa in the
setting of a fixed stomach related to a PEG tube. The serosal injury
was easily repaired intraoperatively with a gastrorrhaphy performed
with the robotic technology. Also in this group, a port-site superficial
SSI occurred. Two readmissions occurred with one patient requiring
a blood transfusion. The aforementioned complications were seen
early, during the first year of this surgeon’s robotic experience. All
cases were successfully completed robotically.
The remaining 7 cases were completed using the da Vinci Si
single site instruments on 1 male and 6 female patients with a mean
age of 43.3 years. The mean BMI was 32.0. The mean total operation
time was 143.4 minutes with a mean console time for the single site
cholecystectomies of 60.1 minutes, a reduction of 6.4 minutes from
the surgeon’s mean console time for multi-port cholecystectomy.
All 7 cases were completed successfully with no complications or
conversions to open. There were no transfusions and all patients were
discharged home the same day. There were no post-operative SSOs
or SSIs. One patient was admitted within a 30 day time period postoperatively
for community-acquired pneumonia.
Group B: Ventral, Incisional, Umbilical Hernias
This group consisted of 60 ventral abdominal wall, incisional
and umbilical hernia repairs which were all successfully completed
robotically; of note, over 50% of these cases incorporated component
separations and/or enterolysis. The patient group was comprised of
22 males and 38 females with an average age of 52.1 years. The mean
BMI was 34.0. The mean total operation time was 214.5 minutes with a
mean console time of 91.6 minutes; the console time was not available
for 6 of these cases. There were 3 complications in this group caused
by a port site hernia in the 3rd case of this group, a port site seroma
in the 5th case of this group, and one port site SSI in the 30th case of
this group. There was one patient who required a blood transfusion.
Average length of stay was 1.5 days with 20 patients able to go home
the same day. Four operations were performed for repair of hernia
recurrences after previous repair by the first author.
Group C: Colorectal
Twenty-eight cases comprise this group and range from colostomy
reversal to hemi-colectomy. Specifically there were 20 left/sigmoid
colectomies, 6 right colectomies, and 2 colostomy reversals. This
patient group was comprised of 10 males and 18 females with a mean
age of 55.1 years and mean BMI of 33.04. The mean total operation
time was 348.4 minutes with a mean surgeon console time of 204.4
minutes. The console time was not recorded for 6 of these cases.
There were 8 complications-case 3, 8, 13, 17, 18, 24, 24, 26-within
the group. Of these, 5 occurred while performing sigmoid colectomy,
an advanced procedure the surgeon began to perform with increased
frequency after case 101. Only 1 case required conversion to open
secondary to need for extensive enterolysis which was early in the
first 6 months of the study. There was 1 patient who required a blood
transfusion. The average length of stay was 5.5 days (range 2-14 days).
There were 3 post-operative SSOs, no SSIs, and 5 readmissions for
a urinary tract infection, abdominal pain, and suspected pulmonary
embolism; four of these patients were ASA class IV at the time of
operation.
Group D: Gastric, Esophageal, Bariatric
Twenty-one cases comprise this group. For the purpose of ensuring
sufficient sample size for the linear model, which is required to answer
the primary hypothesis, esophageal, gastric, and bariatric procedures
were combined into a single group. Procedures performed include 1
Nissen fundoplication, 2 Heller myotomies, 1 gastrocutaneous fistula
resection, 10 para-esophageal hernia repairs, 3 sleeve gastrectomies,
and 1 Roux-en-Y gastric bypass. There were 5 males and 16 females
with a mean age of 50.4 years. The mean BMI was 33.5. The mean
total operation time was 258.3 minutes with a mean surgeon console
time of 137.9 minutes. There were 3 complications in this group, one
of which occurred in a Heller myotomy with hiatal hernia repair and
Dor fundoplication that required a subsequent POEM procedure for
recurrent achalasia in the setting of a sigmoid esophagus in a 21-yearold
male patient with end-stage achalasia.
The robotic Roux-en-Y gastric bypass, case 188 of this 200
case series, was the first robotic bariatric operation performed by
the surgeon and the first one of its kind in the history of the city.
Overall, the case went well. There was continued abdominal pain
from adhesions that was treated 3 months later with laparoscopic
enterolysis. After pain resolution, the patient’s course was satisfactory
and her BMI 6 months status-post surgery had decreased from 41.3 to
32.6. The patient denied any signs or symptoms of gastroesophageal
reflux disease, which was a secondary reason to perform a gastric
bypass in her case, given her BMI. There was 1 patient who required a
blood transfusion. The average length of stay was 2.5 days (range 1-6
days); 1 patient stayed in the hospital for an extra day because of lack
of transportation. There was 1 post-operative SSO which occurred
in case 101 of 200, zero SSI, and 1 readmission. No case required
conversion to open.
Group E: Inguinal Hernias
Forty-five cases comprise this group with 40 of the patients
being male and 5 female. The mean age was 52.9 years and the mean
BMI was 27. The mean total operation time was 161.18 minutes
with a mean surgeon console time of 84.4 minutes; 3 data points
were missing for surgeon console time. Five cases were performed
for recurrent inguinal hernias. There were 4 complications which
occurred in cases 2,111,417 of the group. No patients required a
blood transfusion. The majority of these cases, 39, were performed as
outpatient procedures; the remaining 6 cases had an average length
of stay of 2.7 days (range 1-6 days). There was 1 post-operative SSIs,
no SSOs, and 2 readmissions. No case required conversion to open.
Group H: Multiple Procedures
This group includes 18 cases where the surgeon completed
multiple procedures during one operation. The decision was made
to keep this group separate to better document the console times and
the progression of the surgeon’s learning experience. The procedure
most often performed was repair of inguinal hernia associated with
repair of ventral and/or umbilical hernia. Two female patients and
16 male patients comprise this group. The mean age was 57.9 years
with a mean BMI of 30.3. The mean total operation time was 166.1
minutes with a mean surgeon console time of 84.6 minutes; one data
point was not recorded for surgeon console time. Of the 18 cases, 15
were performed as outpatient. Length of stay was 1 day for a patient
who underwent robotic bilateral inguinal and umbilical hernia repair,
4 days for cholecystectomy with enterolysis and ventral hernia repair,
and 5 days for a patient with BMI of 60 who underwent partial
colectomy and umbilical hernia repair. No case required conversion
to open. There were no complications, SSIs, SSOs, or readmissions.
Table 1
Table 2
Table 3
Table 3
Regression parameters: denoting the average console time for each
surgery group and decrease in console with increasing patient number.
Discussion
This retrospective review of the first 200 robotic general surgery
cases by a single surgeon in a small community hospital without the
resources that would normally be available in a large academic center
shows that, with outcomes comparable to those found in laparoscopy
[28], a robotics program can be safely implemented in a community
hospital setting. This study does not intend to show that robotic
surgery is superior to laparoscopy, nor does it suggest that a robotics
program should be implemented at all community hospitals. What
it hopes to express is that with a surgical team that is motivated and
willing to undergo proper training, a robotics program can be safely
and effectively implemented. The opponents to robotics in general
surgery express concerns that the increased operative time results
in significantly more post-operative complications [29]. Robotics in
general surgery might still be in its early stages with a relative paucity
of data regarding peri-operative outcomes; as such, this position is
understandable. This criticism underscores the need for more studies
on robotic general surgery outcomes and the benefit of implementing
robotics programs, with well-trained surgical teams, in community
hospitals.
A well-trained surgical team is of utmost importance in all robotics
programs and is especially essential in a general surgery program
housed within a non-academic center in which the surgeon assumes
responsibility for arranging training and learning experiences for the
surgical team [30]. Training for the surgical team included a robotics
basics course, an advanced colorectal course, and several case
observations for foregut and bariatrics where the surgeon took his
first assistants and surgical technologists to learn from robotic surgery
experts in other cities and states. The early inexperience of the team
resulted in many confounders for total operative time and docking
time; thus, for the purposes of this review, we focused on console time
to better capture the surgeon’s growth and improvement.
The surgeon’s learning progress on the reported surgical
procedures flowed as follows: cholecystectomy, inguinal hernia,
umbilical, ventral, incisional, colorectal, foregut, bariatric. This
progression highlights measurable improvement from minimal case
difficulty to highly complex cases. Within the subgroups, there is also
a linear progression whereby cases completed early in the surgeon’s
experience required more time than those that came later. In general,
the console time decreased with each additional procedure. We
utilized a linear regression model to investigate the effect of console
time with each additional procedure, controlling for surgical case
type. With each additional case, console time decreased by an average
of 0.3 minutes (p=0.0002), indicating that the surgeon and surgical
team indeed improved with experience.
There were a few items missing from our data. In particular,
surgeon console times were missing for 17 cases: 2 from group A, 6
from group B and C, 2 from group E, and 1 from group H. Missing
data is a common challenge, especially in retrospective studies. The
proportion of missing data in the present study is below 10%, a
threshold above which statistical analyses are likely to be biased [31].
The surgical team attained intimate knowledge of the requisite
training required of the first assistants, surgical technologists, and
nursing staff, in addition to the surgeon to successfully implement a
robotic general surgery program in a community hospital. Another
valuable lesson highlighted in the literature review and throughout
our cases is that, although the robotic technology has been typically
supported for complex surgeries such as foregut and colorectal
procedures, or bariatric revisions, it could also be applied to a large
variety of cases that have been traditionally performed
laparoscopically with comparable benefits to patients. The most
efficient and safest way to acquire the knowledge and skills required
to perform complex robotic procedures is to undergo extensive
model training followed by application of the technology to less
complex cases, which when completed successfully, build the team’s
confidence and abilities for the most complex operations.
After an extensive review of the literature, to our knowledge,
no other surgeon or group to date has reported a robotic general
surgery learning experience encompassing this variety of procedures
in any other American non-academic, small community hospital
environment. Since this retrospective review series of 200 robotic
general surgery cases was completed, other publications by the first
author of this study have supported the observations described in this
paper, both with statistical and clinical significance [32,33].
Conclusion
With increasing case volume while utilizing the robotic platform, and with systematic training for the surgeon and the surgical team, it is possible to show progression by decreasing operative time while maintaining low complication rates in a successful robotic general surgery program in a community hospital. The robotic technology can be applied to complex and routine general surgery procedures while achieving results comparable to those of laparoscopy.
Limitations
As this study is a retrospective review of a single surgeon’s operative experience, limitations arise due to the sample size. For example, the small number of cases per category renders the team unable to statistically test for the presence of learning curves for safety outcomes. Another limitation lies within the nature of the rotating surgical team; if all 200 of the cases in this study were performed by this single surgeon and a non-rotating surgical staff for the duration, it would eliminate the confounding factors inherent in rotating teams. As with all retrospective studies, there are missing data points, but the proportion of patients with the main outcomes missing was small.
Future
We hope that our results may serve as a platform for other multiprocedural studies and provide evidence to support the feasibility of a general surgery robotics program in similar, small community hospitals.
Disclosures
Dr. Oviedo has no conflicts of interest or financial ties to disclose. Dr. Brownstein has no conflicts of interest or financial ties to disclose. Dr. Smith has no conflicts of interest or financial ties to disclose. Dr. Robertson has no conflicts of interest or financial ties to disclose. Dr. Nair-Collins has no conflicts of interest or financial ties to disclose.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Research Data for this Article
Research data for this article is confidential as it was obtained from medical records. Providing open access to the data would be a HIPAA violation and thus this information must remain confidential and cannot be shared.
References
- Cadière GB, Himpens J, Germay O, Izizaw R, Degueldre M, Vandromme J, et al. Feasibility of robotic laparoscopic surgery: 146 cases. World J Surg. 2001;25(11):1467-77.
- Pugin F, Bucher P, Morel P. History of robotic surgery: From AESOP® and ZEUS® to da Vinci®. J Visc Surg. 2011;148(5 Suppl):e3-8.
- Jayaraman S, Davies W, Schlachta CM. Getting started with robotics in general surgery with cholecystectomy: The Canadian experience. Can J Surg. 2009;52(5):374-8.
- Kroh M, El-Hayek K, Rosenblatt S, Chand B, Escobar P, Kaouk J, et al. First human surgery with a novel single-port robotic system: Cholecystectomy using the Da Vinci Single-Site platform. Surg Endosc. 2011; 25(11):3566-73.
- Morel P, Hagen M, Bucher P, Buchs N, Pugin F. Robotic single-port cholecystectomy using a new platform: Initial clinical experience. J Gastrointest Surg. 2011;15(12):2182-86.
- Oviedo RJ, Robertson JC, Alrajhi S. First 101 robotic general surgery cases in a community hospital. JSLS. 2016;20(3).
- Morelli L, Guadagni S, Di Franco G, Palmeri M, Di Candio G, Mosca F. Da Vinci single site surgical platform in clinical practice: a systematic review. Int J Med Robot. 2016;12(4):724-34.
- LeBlanc K, Booth W. Laparoscopic repair of incisional abdominal hernias using expanded polytetrafluoroethylene: Preliminary findings. Surg Laparosc Endosc. 1993;3(1):39-41.
- Beldi G, Ipaktchi R, Wagner M, Gloor B, Candinas D. Laparoscopic ventral hernia repair is safe and cost effective. Surg Endosc. 2006;20(1):92-5.
- Allison N, Tieu K, Snyder B, Pigazzi A, Wilson E. Technical feasibility of robot-assisted ventral hernia repair. World J Surg. 2012;36(2):447-52.
- Gonzalez A, Escobar E, Romero R, Walker G, Mejias J, Gallas M, et al. Robotic-assisted ventral hernia repair: A multicenter evaluation of clinical outcomes. Surg Endosc. 2017;31(3):1342-9.
- Trevisonno M, Kaneva P, Watanabe Y, Fried GM, Feldman LS, Andalib A, et al. Current practices of laparoscopic inguinal hernia repair: A population-based analysis. Hernia. 2015;19(5):725-33.
- Kudsi O, McCarty J, Paluvoi N, Mabardy A. Transition from Laparoscopic Totally Extraperitoneal Inguinal Hernia Repair to Robotic Transabdominal Preperitoneal Inguinal Hernia Repair: A Retrospective Review of a Single Surgeon’s Experience. World J Surg. 2017;41(9):2251-7.
- Waite K, Herman M, Doyle P. Comparison of robotic versus laparoscopic transabdominal preperitoneal (TAPP) inguinal hernia repair. J Robot Surg. 2016;10(3):239-44.
- Weber P, Merola S, Wasielewski A, Ballantyne GH. Telerobotic-assisted lapa-roscopic right and sigmoid colectomies for benign disease. Dis Colon Rectum. 2002;45(12):1689-94.
- Sawada H, Egi H, Hattori M, Suzuki T, Shimomura M, Tanabe K, et al. Initial experiences of robotic versus conventional laparoscopic surgery for colorectal cancer, focusing on short-term outcomes: A matched case-control study. World J Surg Oncol. 2015;13:103.
- Baek S, Carmichael J, Pigazzi A. Robotic surgery: Colon and rectum. Cancer J. 2013;19(2):140-46.
- Lorenzon L, Bini F, Balducci G, Ferri M, Salvi PF, Marinozzi F. Laparoscopic versus robotic-assisted colectomy and rectal resection: A systematic review and meta-analysis. Int J Colorectal Dis. 2016;31(2):161-73.
- Cadiere G, Himpens J, Vertruyen M, Favretti F. The world’s first obesity surgery performed by a surgeon at a distance. Obes Surg. 1999;9(2):206-9.
- Villamere J, Gebhart A, Vu S, Nguyen NT. Utilization and outcome of laparoscopic versus robotic general and bariatric surgical procedures at Academic Medical Centers. Surg Endosc. 2015;29(7):1729-36.
- Yao G, Liu K, Fan Y. Robotic Nissen fundoplication for gastroesophageal reflux disease: A meta-analysis of prospective randomized controlled trials. Surg Today. 2014;44(8):1415-23.
- Tolboom R, Broeders I, Draaisma W. Robot-assisted laparoscopic hiatal hernia and antireflux surgery. J Surg Oncol. 2015;112(3):266-70.
- Galvani C, Gorodner M, Moser F. Robotic-assisted Heller myotomy: A modern technique and review of outcomes. Surg Endosc. 2006;20:1105.
- Afaneh C, Finnerty B, Abelson J, Zarnegar R. Robotic-assisted Heller myotomy: A modern technique and review of outcomes. J Robotic Surg. 2015;9(2):101-8.
- Shaligram A, Unnirevi J, Simorov A, Kothari V, Oleynikov D. How does the robot affect outcomes? A retrospective review of open, laparoscopic, and robotic Heller myotomy for achalasia. Surg Endosc. 2012;26(4):1047-50.
- Agha RA, Borrelli MR, Vella-Baldacchino M, Thavayogan R, Orgill DP; STROCSS Group. The STROCSS statement: Strengthening the Reporting of Cohort Studies in Surgery. Int J Surg. 2017;46:198-202.
- https://www.intuitivesurgical.com/products/davinci_surgical_system/.
- Tsuda S, Oleynikov D, Gould J, Azagury D, Sandler B, Hutter M, et al. SAGES TAVAC safety and effectiveness analysis: da Vinci® Surgical System (Intuitive Surgical, Sunnyvale, CA). Surg Endosc. 2015;29(10):2873.
- Philip S, Jackson N, Mittal V. Outcomes after laparoscopic or robotic colectomy and open colectomy when compared by operative duration for the procedure. Am J Surg. 2018;215(4);577-80.
- Tomulescu V, Stănciulea O, Bălescu I, Vasile S, Tudor S, Gheorghe C, et al. First year experience of robotic-assisted laparoscopic surgery with 153 cases in a general surgery department: Indications, technique and results. Chirurgia (Bucur). 2009;104(2):141-50.
- Bennett D. How can I deal with missing data in my study? Aust N Z J Public Health. 2001;25(5):464-9.
- Oviedo RJ, Robertson JC, Desai A. Robotic ventral hernia repair and endoscopic component separation: Outcomes. JSLS. 2017;21(3).
- Oviedo Barrera RJ. The Surgical Robot: Applications and Advantages in General Surgery. In: Kucuk S, editor. Surgical Robotics. Rijeka, Croatia: InTech; 2018. p. 39-64.