Review Article
Bilobar Liver Metastases: A Challenge for Surgical Strategies
Fabio Uggeri1,2, Mattia Garancini1, Simone Famularo1,2, Enrico Pinotti1,2, Luca Gianotti1,2 and Fabrizio Romano1,2*
1Department of Surgery, San Gerardo Hospital, Italy
2Department of Surgery, University of Milano Bicocca, Italy
*Corresponding author: Fabrizio Romano, Department of Surgery, School of Medicine, University of Milano Bicocca, Chirurgia I San Gerardo Hospital via Pergolesi 33, Monza, Italy
Published: 13 Jul, 2018
Cite this article as: Uggeri F, Garancini M, Famularo S, Pinotti E, Gianotti L, Romano F. Bilobar Liver Metastases: A Challenge for Surgical Strategies. World J Surg Surgical Res. 2018; 1: 1023.
Abstract
In recent decades, the surgical approach in patients with liver metastasis has seen substantial changes. The encouraging results in terms of survival after surgical resection led to more interventionist attitude, widening indications and bringing more and more patients to curative treatments. Moreover, the technological advancement of surgical devices and the improvement of imaging techniques have made liver surgery safer and more feasible. But, in the most complex cases the attempt to perform surgical curative resections often collided with the inability to preserve an appropriate post-operative volume, necessary to avoid postoperative hepatic failure. In fact the management of liver cirrhosis or small size hepatic remnant still remains a challenge. Currently post-hepatectomy liver failure is the major cause of death after liver resection often associated with sepsis and ischemia-reperfusion injury. In recent years, surgeons have been working to develop new strategies to overcome this limit. Several methods have been proposed for preventing postoperative hepatic failure both in the preoperative, perioperative and postoperative management. Since the introduction of the preoperative portal embolization proposed by Makucchi in the 80’s giant steps have been made. To date in order to limit the damage to parenchyma and to optimize regenerative hepatic capacity many technical considerations have been taken into account. The purpose of this chapter is to describe the new surgical attitudes regarding the treatment of bilobar liver metastases, focusing on surgical techniques that at present seem to be more effective, underlying the benefit and limits of each procedure. In addition to the technical description, a comparison of the various procedures was carried out to demonstrate the feasibility and to check for the critical issue of each one.
Keywords: Liver metastases; Hepatectomy; ALPPS
Introduction
The liver is a common site of metastases from malignant tumors of gastrointestinal tract and
about 50% to 60% of liver tumors have a secondary origin with over 50% of patients with colorectal
cancers who will develop liver metastases during the course of disease [1,2].
Although in the last decades the improvement in surgical techniques, chemotherapy and
biological therapies has led to more favorable prognostic results with survival rates ranging prior
from 23% to 45 % increasing to almost 60% more recently, a large portion of these patients still die
for this disease [3-7].
Besides the encouraging results obtained in terms of survival in the surgical treatment
of metastatic colorectal and neuroendocrine cancers [8-11] has prompted the surgeon to an
increasingly aggressive attitude towards this disease. Surgery with radical intent is considered to be
the focal point in the treatment of patients suffering from colorectal cancer liver metastases, being
the only treatment associated with chemotherapy that can significantly improve survival.
The role of surgery in this context is becoming increasingly important and the indications for
surgical intervention in advanced disease are expanding.
The need to perform a surgery with radical intent in many cases conflicts with the impossibility
of recruiting patients for resection for the extension of bilobar disease that is too advanced to allow
a radical resection, in fact only about 15% to 25% of patients with colorectal metastases at the time
of diagnosis is eligible for primary liver resection [12].
Moreover in patients with extensive bilobar liver metastases
resection is challenging is due to the necessity to preserve an adequate
proportion of liver parenchyma after resection, in order to avoid the
risk of Postoperative Liver Failure (PLF) [13].
The present purpose is to minimize the chance of postoperative
hepatic dysfunction using strategies aimed to induce hypertrophy of
the Future Remnant Liver (FLR), in order to increase the safety of
resection [14].
An extensive liver resection is frequently required to achieve a
Radical resection (R0); it is evident that the safety of this procedure
conflicts with the inability to preserve in many cases a sufficient
post-operative liver parenchyma. PLF is the most common cause
of mortality after an extended hepatectomy, so PLF is the biggest
obstacle faced by hepato-biliary surgeons [15].
In the 1980s Makuuchi et al. [16] introduced the concept of Portal
Vein Embolization (PVE); this technique involves the embolization
of the right portal branch in order to induce hypertrophy in the left
lobe, enabling a safer removal of large or multiple tumors, mostly
located in the right hemiliver and segment IV. This procedure was
rapidly adopted by many surgeons to prevent liver failure after a
variety of extensive right-sided hepatectomies [17].
The next advances of technique were proposed about 10 years
later by the surgical team of Paul-Brousse Hospital in Paris with the
introduction of sequential surgical procedures, referred “ Two-Stage
Hepatectomy (TSH)” to stepwise remove multiple liver tumors, with
the aim of allowing the liver to regenerate between both procedures
[18].
Although at first the technique did not foresee in all cases the
embolization of the right portal branch, the further evolutions with the
routine use of portal embolization after the left lobe surgical cleaning,
allowed a higher rate of hypertrophy with a safer curative right or
extended-right hemihepatectomy [19]. Subsequently the group from
Zurich modified this approach by proposing concomitant ligation of
a Portal right Vein (PVL) with the resections of all left-sided tumors
during the first surgery, followed a few weeks later by an extended
right hepatectomy [20].
The rationale behind this change is that the portal vein ligation is
easy to perform during the first surgical step with the left liver surgical
cleansing and leads to a rate of regeneration even greater than PVE.
The drawback of these techniques is a long time to achieve
hypertrophy between the two surgical step that leads in about
19% to 28% of cases to a disease progression and therefore to the
impossibility of being enrolled for the second surgical stage [21,22].
Other shortcomings included the insufficient hypertrophy of a
putative remnant liver, preventing curative resection or, if performed,
leading to postoperative failure due to “small for size” syndrome.
Recently to overcome the problems mentioned above, this
technique has been modified by performing a portal vein ligation
with a "split in liver" during the first stage; Schnitzbauer et al. [23]
described a this novel approach: “Associating Liver Partition and
Portal vein ligation for Staged hepatectomy” (ALPPS). This technique
resulted in a 74% increase in the volume of the liver remnant, and
ALPPS leads to faster liver hypertrophy rate in 7-14 days when
compared to TSH which has an average of 99 days (range: 32-210
days) to reach the desired result before the second surgery [24,25].
Initially, the major controversies to the technique were due to the high rate of morbidity and mortality, reported in about 68% and
14% respectively by Schnitzbauer. Although so many advances and
refinements of the initial technique have been made in the last years
with a reduction in complications, ALPPS continues to cause heated
controversy.
One-Stage Hepatectomy
In the surgical treatment of bilobar metastases from colorectal
cancer, the two-stage hepatectomy approach is commonly used. This
method allows extending the surgical indication to patients judged
initially inoperable and leads to a higher rate of curative resections,
but this approach have some drawbacks. Primarily, patients
underwent two surgical procedures and each of which is associated
with morbidity and mortality. Secondly, not all patients underwent
the first intervention can also be subjected to the second surgical step
for progression of the disease occurring in the time elapsed between
the two procedures.
A possible alternative was proposed by Torzilli et al. [26]; they
showed how both for primary or metastatic liver tumors a welldefined
policy of ultrasonically guided hepatectomy allows to carry
out radical operations safely and without major removal of liver
parenchyma in the vast majority of patients. This group demonstrated
how One-Stage Hepatectomy (OSH) can be performed even in
the presence of a complex tumor presentation such as multiplicity
and vascular invasion [27,28]. The aims of this technique were to
establish a surgical procedure that maximizes parenchymal-sparing
and allows curative resection in one stage. The technique uses a very
accurate Intraoperative Ultrasound (IOUS) also with specific contrast
agent to identify the relationship between tumor lesions and liver
vascularization. The hepatic vessels were spared if it is detectable by
IOUS a thin layer of liver parenchyma even if <5 mm from neoplastic
lesion, if the portal branch was in contact with metastases without
vessel wall discontinuation and without proximal bile duct dilation;
in all the other conditions vessel resection was carried out, even if the
aim of this procedure is to maintain the skeletal architecture of the
liver intact.
The technique leads to minimizing the loss of healthy parenchyma
that normally occurs during a major hepatectomy, extending the
resection as close as possible to the neoplastic lesion. This inevitably
leads to obtain surgical disease-free margins in many cases of the
order of 1 mm or less. In fact the main criticism to OSH could be the
high proportion of patients receiving a resection with surgical margin
with microscopic neoplastic infiltration (R1 resection) [29].
It is widely shown that an adequate disease-free surgical margin is
essential to provide to patients an effective neoplastic treatment; but
actually especially as regards colorectal liver metastases, the surgeon's
approach was to move towards a progressive reduction in surgical
margins, which ranged from 1 cm to 1 mm.
Moreover, the complexity of these resections often requires that
R1 resection is needed, especially when the lesion is located near a
vessel. Vessel detachment (R1 vascular margin) is mandatory in
many circumstances to avoid greater resection that would result in a
higher rate of non-resectable patients for possible PLF.
In this regard Viganò et al. [30] showed how R1 vascular resection
can be considered in terms of outcome comparable to parenchymal
R0 resection. They claimed that R1 vascular resection guaranteed the
same local control of the disease as compared to parenchymal R0
resection, confirming the hypothesis that neoplastic contact with the vessel walls limits neoplastic spread.
A recent multicenter study compared patients underwent two
stage hepatectomy with patients in whom performed one stage
hepatectomy to elucidate if drop-out (patients not achieving the
second stage) of TSH is a patient selection or loss of chance [29]. The
patients were matched to have similar tumor features. The manuscript
reported a similar outcome for the two surgical procedures and
postulated that drop-out of TSH may be a loss of chance rather than
a patient's selection. Unselected patients whom underwent to OSH
have same outcomes as selected patients who completed the TSH
with similar survival and recurrence rates.
Another point in favor of the surgical technique proposed by
Torzilli et al. [26] is the high level of lesions identified intraoperatively
that it is reported up to 42% of the metastases removed, which had
not been identified by preoperative instrumental examinations.
Evaluated the oncological efficacy of the OSH compared with
the most well-established two stage hepatectomy, some limitations
should be highlighted: first of all, the technique involves an adequate
preparation of the surgeon on the use of intraoperative ultrasound
imaging, since without a correct training it is difficult to perform such
complicated interventions.
The fact that the technique involves multiple combined procedures
with the aid of ablative techniques also leads to longer duration
of surgery and long vascular clamping times, leads to anesthesia
risk and a greater chance of alteration of liver function on the first
postoperative days. Although these possible causes of morbidity are
in part negligible, reduced liver flow by vascular clamping minimizes
the rate of perioperative transfusions with beneficial effects on long
and short term outcomes [31].
In conclusion, the technique, albeit with the aforementioned
limits, appears to be a valid alternative to TSH and can overcome
some of the limitations and consequences of a 2-stage approach.
Two-Stage Hepatectomy
Two-Stage Hepatectomy (TSH) has been developed as a surgical
strategy for extremely complicated cases of bilobar metastatic liver
disease in order to achieve a curative R0 resection. The main principle
of this approach is a sequential resection by a two-staged liver surgery;
its goal is to perform a complete metastasectomy in those cases in
which a major resection in a single time would have left a FLR too
small for patient's survival. The success of this approach is dependent
on regeneration of liver tissue after the first stage. Experiments
performed almost a century ago suggested that selective occlusion
of the portal branch causes atrophy of the ipsilateral liver lobe and
hypertrophy of the contralateral lobe. Portal vein embolization and
portal vein ligation are procedures used in order to increase the size of
the future liver remnant before major hepatic resection. A significantly
greater volume of FLR correlates with improved synthetic function
and thus enables a reduction in the risk of postoperative liver failure.
In the late 1980s, Makuuchi et al. [16] first used the selective occlusion
strategy in patients in order to extend the limits of liver resection.
The technique includes a first stage in which FLR (the less affected
lobe that will be designated the future liver remnant, usually the left
lobe) is resected by either wedge resections and/or ablation. Portal
vein ligation may be performed during the first stage otherwise portal
vein embolization can be performed after the first operation to induce
hypertrophy of the future liver remnant [32].
PVE stimulates the proliferation of hepatocytes as well as the
growth of occult metastases located in the non-embolized hemiliver,
as a consequence, progression of liver metastases in the remnant
liver could preclude the achievement of a curative liver resection;
for this reason metastasectomy in the future liver remnant should
precede PVE. In the most of liver units PVE is usually planned two
weeks after the first surgical stage. The second-stage operation will
then be performed most commonly with a hepatectomy of the more
affected contralateral lobe. The success of this method relies on liver
regeneration between the two interventions, allowing the second
surgical step to be performed with a lower risk of PLF. The optimal
time interval before performing the second liver resection has not yet
been clarified and is currently calculated based on the rate of liver
regeneration and the control of remnant liver tumors with CT scan
(mean time 30-50 days after PVE). Although portal occlusion (PVE
or PVL) can increase the volume of the FLR by up to 40%, the second
stage of the procedure was not always performed [33]. Some authors
reported a drop-out rate ranging from 22% to 28% [29], in most cases;
the second surgical stage is abandoned for the presence of disease
progression in a short time or for insufficient liver regeneration.
The rate of patients who can be enrolled in the second stage is
about 76% with a range from 64% to 87% [34,35], as mentioned
above the most frequent cause of not completion of the procedure
is progression of disease that is present in 13% to 35% of patients, in
a less part of patients two stage hepatectomy can't be performed for
inadequate liver regeneration (0% to 4%) or for poor condition of
patient (3%) [36,37]. Patients who did not complete two stage had
extremely unfavourable prognosis with a median survival of 20.4
months compared to those underwent second surgical stage ( median
survival 56.8%). Three and 5-year survival rates were 68% and 49%,
respectively, for patients who underwent second-stage resection and
6% and 0%, respectively, for patients who did not [38,39].
Regard postsurgical morbidity Passot et al. [38] reported a rate of
major complications of 26% after the second surgical stage and of 6%
for the first. 90-day mortality after second surgery was 7%.
Some authors highlighted how several features on FLR can be
considered as negative prognostic factors, as regard the study of Narita
et al. [36] showed how the presence of three or more metastases in
FLR is an independent risk factor for the failure to achieve the second
stage leading to a progression of disease and formation of “de novo”
metastases in the remnant liver.
Several experimental studies suggested that an alteration
hypoxia-induced of tumor microenvironment leads to increased
production of Vascular Endothelial Growth Factors (VEGF), which
can stimulate beyond liver regeneration the growth of dormant
micrometastases [40]. Transient hypoxia generated by PVE in nonembolized
hemiliver could explain the rate of progression of disease
observed [41].
In consideration of this patients enrolled for the procedure
should receive an interval chemotherapy in order to control tumor
progression while awaiting the regeneration of FLR, this is also based
on initial observations that showed how in patients who did not
underwent to an interval chemotherapy a second-stage hepatectomy
became impossible. The actual administration of the interval
chemotherapy is mandatory.
Currently TSH should be considered in selected patients with
bilobar colorectal liver metastases in which a right hepatectomy would leave more than three metastases or any metastasis of more
than 3 cm in the FLR [42].
In conclusion TSH combined with chemotherapy and timed PVE
achieved good results in terms of long-term survival and morbidity
with acceptable mortality, but selection criteria for chemotherapy
regimens during TSH have not yet been well defined and further
clinical trials will be needed to improve the usefulness of the
procedure.
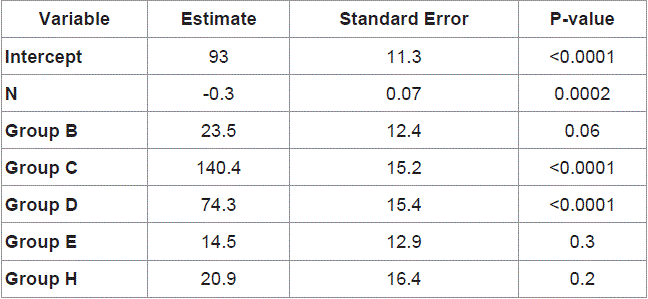
Table 1
ALPPS (Associating Liver Partition and Portal Vein Ligation for Staged Hepatectomy)
The rate of patients not meeting the second stage reflects the
two-stage hepatectomy limits, mostly for the progression of disease
occurring within the longest time needed to achieve an adequate
hypertrophy in the future liver remnant. Recently, to overcome these
limits in attempt to bring more patients to radical resection, a new
surgical approach was proposed with an acronym ALPPS (Associating
Liver Partition and Portal vein ligation for Staged hepatectomy). It
represents an evolution of two-stage hepatectomy. This technique has
led to an increase of 74% in the volume of the FLR in a mean period
of 9 days and greatly reduced the time between the two surgical
procedures with a completion rate close to 100%, offering a chance to
patients with otherwise irresectable tumors [43].
ALPPS is typically applied to those patients with very low FLR and
may be offered to patients without adequate FLR after embolization of
the portal branch or in patients without an initial surgical indication
with other techniques [44,45].
The procedure involves two surgical stages: During exploratory
laparotomy the liver tissue was assessed macroscopically and general
resectability was defined on the basis of a tumor-free left later liver
lobe. The liver is mobilized through the section of falciform, triangular
and coronary ligaments and the cava vein is exposed with the
relevant hilar structures. Furthermore the assessment of resectability
is evaluated and confirmed with intraoperative ultrasound and the
positioning of the tumor in relation with vessels. The right portal vein
branch is identified and sectioned, the right liver lobe is mobilized
and parenchymal transection in situ is performed. All portals, arterial
and biliary branches for segment IV° are divided along the rim of the
round ligament. Finally, the right lobe is covered in a plastic bag to
prevent any post-operative adhesions and the abdomen is closed [33].
Usually after an interval of 7-14 days patients undergo to a CT hepatic
volumetry and the second surgical stage is performed to complete the
resection with the ligation of the right artery [46], right bile duct and
the right hepatic vein.
The technique was first performed in 2007 by Schlitt in Regensburg
(Germany) but was first described in a scientific publication in
Annals of Surgery in 2012 by Schnitzbauer et al. [23]. They described
the first series of 25 cases; the study reported an increased percentage
of FLR of 74% in 9 days, so more rapid and effective than normally
occurs with the techniques of vascular occlusion (14-42 days with a
hypertrophy rate until 40%) [47].
Therefore, ALPPS offers a solution for the two major limitations
of PVE and TSH: Failure to achieve the desired hypertrophy, long
time to reach it and the high drop-off rate following the progression
of the disease. Failure to complete the second stage in TSH leads to
a really poor prognosis that is lower than patients treated only with
chemotherapy hence outlines the importance of completing the two stage procedures [48].
The rationale of this new approach is based on the fact that liver
transection leads to an interruption of possible collateral vessels
between the two portions of hepatic parenchyma, amplifying the
effect of the portal overflow to the FLR hindering recanalization of
embolized portal branches. It may be explained with the impressive
effect on liver regeneration.
The study of Knoefel et al. [49] compared a rate of parenchymal
hypertrophy in series of 22 patients underwent isolated PVE (12
patients), ALPPS (7 patients) and combined procedures (3 patients),
they reported a mean volume increase by 63% after 3 days in patients
underwent ALPPS with a volume gain of 22% per day, significantly
higher than the group treated with PVE alone.
Also with regard to neoplastic progression on the "nonembolized"
liver in the interval between the portal embolization and
second surgery, fact demonstrated by some authors [50,51], ALPPS
seems to partly obviated the problem by greatly reducing the waiting
time to complete the procedure.
Another point in favor of the ALPPS is the possibility of avoiding
neoplastic infiltration of FLR, especially in the presence of lesions
adjacent to major vascular structures that should otherwise be
sacrificed in case of infiltration or encasement [52].
Past Authors emphasized that the feasibility of achieving tumor
resection appears to be the most significant advantage of ALPPS. To
date analysis of international ALPPS registry showed a completion
rate near 100% on 553 patients from 84 centers around the world [53].
On the other hand the procedure has raised many criticisms for
the high morbidity and mortality rate shown in the first case studies.
Schnitzbauer reported a morbility of 64% and a mortality of 12%,
while Knoefel showed that only two of 7 patients had a course free
of complication.
The major complications are due to septic events supported
by the presence of bile leak and largely by the necrosis of the IV°
liver segment although initial data could be discouraged to the use
of this technique [54], ALLPS have not been abandoned and these
disadvantages have led to a technical review. In fact a recent work of
Hernandez-Alejandro et al. [55] reported a reduction in morbidity
rate of 36% and a 90-day mortality rate of 0%. The achievement
of these results is due to a revision of the technique by the authors
who avoid dissection of the structures of the hepatoduodenal
ligament and the saving of the vascular and biliary afferences to the
IV° hepatic segment. In recent years many other authors proposed
further technical revisions in an attempt to make ALPPS more safety:
Totally laparoscopic [56], hybrid [57], partial [58], anterior approach
[59], left, rescue, right ALPPS [60] and satisfactory results were
achieved. These surgical changes, in addition to a careful assessment
of patient recruitment based on neoplastic biology in accordance to
chemotherapy response, may result in a reduction in mortality and
morbidity rate.
Beyond the flexibility of the technique the validation of such
extreme surgical procedure should be supported by significant
oncological findings. At present also due to the limited follow-up
of this new procedure, long-term oncological outcomes remain
unknown [61-64].
The promising short-term results obtained are difficult to translate oncologically, because of the heterogeneous group of patients with
different underlying pathologies, variable chemotherapy use, and
technical variations applied. In case of Colorectal Liver Metastases
(CRLM) in a 2-centers study including 33 patients, Disease Free
Survival (DFS) after TSH for CRLM was 85% and 68% at 1 and 2
years, respectively [65]. In a larger cohort the rate of DFS of those
patients [63], who completed the second stage (n=47), reached 39%
at 1 year and 20% at 3 years in an intent-to-cure analysis but only
in patients, who underwent both stages. In comparison, the 1 and
2-year DFS in the ALPPS registry for patients with CRLM of 59%
and 41%, respectively, with a median DFS of 14 months, may be
considered acceptable, particularly assessing that almost all patients
could eventually benefit from a curative resection [64].
A study by Oldhafer et al. [45] found that 86% of patients had a
tumor recurrence with a median time of 8 months after ALPPS. They
stated that ALPPS had the same potential for tumor progression as
PVE.
Another concern raised was that liver is strongly manipulated in
the ALPPS procedure, which may promote tumor cell dissemination
by detaching cells into the systemic and pulmonary circulation.
Additionally, the local and systemic release of growth factors may
further stimulate tumor growth.
Recurrence rate data are unsatisfactory with ranges from 5%
to 86% due to different follow-up periods and heterogeneous case
evaluated.
The observation that DFS is lower in ALPPS than TSH could
come to the conclusion that many patients go to the procedure with
little or no oncological benefit. Numerous studies showed that in TSH
the DFS are higher and morbidity lower than ALPPS [65,66].
Actual gold standard indication for ALPPS is colorectal
bilobar liver metastases in patients younger than 60 years. Pringle's
manoeuvres, primitive liver disease, previously systemic chemo or
radiotherapy, cholestasis, primary biliary tumors (Klatskin tumor's)
are risk factors for a worse prognosis after first surgical procedure for
reducing liver regeneration. Both TSH and PVE should be preferred
in oncological terms when it is possible with these techniques to
achieve complete resection.
In conclusion, ALPPS should be seen an interesting evolution of
two-stage procedures for colorectal liver metastases. Its advantage
in terms of feasibility compared with TSH is real but limited when
the procedures are clearly indicated. Additionally, ALPPS should
be proposed to patients with caution and warnings about a still
higher morbidity than with TSH or one stage hepatectomy, which
will remain the standard approach for obtaining R0 resection in
patients with bilobar advanced CRLM and inadequate FLR [67].
It is foreseeable that with the rapid diffusion of new neoadjuvant
chemotherapic regimens, the need for ALPPS, as a safe strategy to
the classic two-stage approach, will increase. In fact more patients are
and will gain resectability due to partial or sometimes full response to chemotherapy protocols. Thus a multidisciplinary approach
starting with aggressive neoadjuvant regimen, under indications of
institutional tumor boards will push more patients to ALPPS (Table 1).
Conclusion
Nowadays the feasibility of major liver resections is well
established and the coming years will lead to improve the safety of
liver resections. In the spectrum of future surgical barriers, the risk of
postoperative liver failure will always be the main concern in pushing
the surgical indications on complicated patients. Taking into account
the basic hepatic functional principles the regeneration techniques
now focused on pure quantitative hypertrophy will move in an
attempt to achieve a higher qualitative hypertrophy. The progression
of these procedures will have to keep in mind some fundamental
factors: Minimisation of morbidity and mortality associated with
the given procedures. The rapid increase of FLR in order to prevent
disease progression and further research should be carried out to
clarify the causes leading to tumor progression during the period
between the two procedures. In addition, another issue that remains
unresolved is to refine the role of chemotherapy and the optimal
timing to use it.
In the end, the evolution of surgery in this field has led to
encouraging success but surgeons should never forget that a justified
non-operative approach will always be less invasive than the least
invasive surgical approach.
References
- Alberts SR, Wagman LD. Chemotherapy for colorectal cancer liver metastases. Oncologist. 2008;13(10):1063-73.
- Kasper HU, Drebber U, Dries V, Dienes HP. Liver metastases: incidence and histogenesis. Z Gastroenterol. 2005;43(10):1149-57.
- Goldberg RM, Rothenberg ML, Van Cutsem E, Benson AB, Blanke CD, Diasio RB, et al. The continuum of care: a paradigm for the management of metastatic colorectal cancer. Oncologist. 2007;12(1):38-50.
- Jaeck D, Pessaux P. Bilobar colorectal liver metastases: treatment options. Surg Oncol Clin N Am. 2008;17(3):553-68.
- Benoist S, Nordlinger B. The role of preoperative chemotherapy in patients with resectable colorectal liver metastases. Ann Surg Oncol. 2009;16(9):2385-90.
- Ismaili N. Treatment of colorectal liver metastases. World J Surg Oncol. 2011;9:154.
- Quan D, Gallinger S, Nhan C, Auer RA, Biagi JJ, Fletcher GG, et al. The role of liver resection for colorectal cancer metastases in an era of multimodality treatment: a systematic review. Surgery. 2012;151(6):860-70.
- Spelt L, Andersson B, Nilsson J, Andersson R. Prognostic models for outcome following liver resection for colorectal cancer metastases: a systematic review. Eur J Surg Oncol. 2012;38(1):16-24.
- Jagannath P, Chhabra D, Shrikhande S, Shah R. Surgical treatment of liver metastases in neuroendocrine neoplasms. Int J Hepatol. 2012; 2012:782672.
- Lee SY, Cheow PC, Teo JY, Ooi LL. Surgical treatment of neuroendocrine liver metastases. Int J Hepatol. 2012;2012:146590.
- Adam R, Chiche L, Aloia T, Elias D, Salmon R, Rivoire M, et al. Hepatic resection for noncolorectal nonendocrine liver metastases: analysis of 1452 patients and development of a prognostic model. Ann Surg. 2006;244(4):524-35.
- Lang H. ALPPS for Colorectal Liver Metastases. J Gastrointest Surg. 2017;21(1);190-2.
- Okabe H, Beppu T, Nakagawa S, Yoshida M, Hayashi H, Masuda T, et al. Percentage of future liver remnant volume before portal vein embolization influences the degree of liver regeneration after hepatectomy. J Gastrointest Surg. 2013;17(8):1447-51.
- Imamura H, Seyama Y, Kokudo N, Maema A, Sugawara Y, Sano K, et al. One thousand fifty-six hepatectomies without mortality in 8 years. Arch Surg. 2003;138(11):1198-206.
- Cai YL, Song PP, Tang W, Cheng NS. An updated systematic review of the evolution of ALPPS and evaluation of its advantages and disadvantages in accordance with current evidence. Medicine (Baltimore). 2016;95(24):e3941.
- Makuuchi M, Thai BL, Takayasu K, Takayama T, Kosuge T, Gunven P, et al. Preoperative portal embolization to increase safety of major hepatectomy for hilar bile duct carcinoma: a preliminary report. Surgery. 1990;107(5):521-7.
- de Baere T, Roche A, Elias D, Lasser P, Lagrange C, Bousson V. Preoperative portal vein embolization for extension of hepatectomy indications. Hepatology. 1996;24(6):1386-91.
- Adam R, Laurent A, Azoulay D, Castaing D, Bismuth H. Two-stage hepatectomy: a planned strategy to treat irresectable liver tumors. Ann Surg. 2000;232(6):777-85.
- Jaeck D, Oussoultzoglou E, Rosso E, Greget M, Weber JC, Bachellier P. A two-stage hepatectomy procedure combined with portal vein embolization to achieve curative resection for initially unresectable multiple and bilobar colorectal liver metastases. Ann Surg. 2004;240(6):1037-49.
- Clavien PA, Petrowsky H, DeOliveira ML, Graf R. Strategies for safer liver surgery and partial liver transplantation. N Engl J Med. 2007;356(15):1545-59.
- Shindoh J, Vauthey JN, Zimmitti G, Curley SA, Huang SY, Mahvash A, et al. Analysis of the efficacy of portal vein embolization for patients with extensive liver malignancy and very low future liver remnant volume, including a comparison with the associating liver partition with portal vein ligation for staged hepatectomy approach. J Am Coll Surg. 2013;217(1):126-33.
- Tsai S, Marques HP, De Jong MC, Mira P, Ribeiro V, Choti MA, et al. Two-stage strategy for patients with extensive bilateral colorectal liver metastases. HPB (Oxford). 2010;12(4):262-9.
- Schnitzbauer AA, Lang SA, Goessmann H, Nadalin S, Baumgart J, Farkas SA, et al. Right portal vein ligation combined with in situ splitting induces rapid left lateral liver lobe hypertrophy enabling 2-staged extended right hepatic resection in small-for-size settings. Ann Surg. 2012;255(3):405-14.
- Sala S, Ardiles V, Ulla M, Alvarez F, Pekolj J, de Santibañes E. Our initial experience with ALPPS technique: encouraging results. Updates Surg. 2012;64(3):167-72.
- Torzilli G, Procopio F, Botea F, Marconi M, Del Fabbro D, Donadon M, et al. One-stage ultrasonographically guided hepatectomy for multiple bilobar colorectal metastases: a feasible and effective alternative to the 2-stage approach. Surgery. 2009;146(1):60-71.
- Torzilli G, Donadon M, Marconi M, Palmisano A, Del Fabbro D, Spinelli A, et al. Hepatectomy for stage B and stage C hepatocellular carcinoma in the Barcelona Clinic Liver Cancer classification: results of a prospective analysis. Arch Surg. 2008;143(11):1082-90.
- Torzilli G, Donadon M, Marconi M, Botea F, Palmisano A, Del Fabbro D, et al. Systematic extended right posterior sectionectomy: a safe and effective alternative to right hepatectomy. Ann Surg. 2008;247(4):603-11.
- Viganò L, Torzilli G, Cimino M, Imai K, Vibert E, Donadon M, et al. Drop-out between the two liver resections of two-stage hepatectomy. Patient selection or loss of chance? Eur J Surg Oncol. 2016;42(9):1385-93.
- Viganò L, Procopio F, Cimino MM, Donadon M, Gatti A, Costa G, et al. Is tumor detachment from vascular structures equivalent to R0 resection in surgery for colorectal liver metastases? An observational cohort. Ann Surg Oncol. 2016;23(4):1352-60.
- Yamamoto J, Kosuge T, Takayama T, Shimada K, Yamasaki S, Ozaki H, et al. Perioperative blood transfusion promotes recurrence of hepatocellular carcinoma after hepatectomy. Surgery. 1994;115(3):303-9.
- Capussotti L, Muratore A, Baracchi F, Lelong B, Ferrero A, Regge D, et al. Portal vein ligation as an efficient method of increasing the future liver remnant volume in the surgical treatment of colorectal metastases. Arch Surg. 2008;143(10):978-82.
- Turrini O, Ewald J, Viret F, Sarran A, Goncalves A, Delpero JR. Two-stage hepatectomy: who will not jump over the second hurdle? Eur J Surg Oncol. 2012;38(3):266-73.
- Homayounfar K, Liersch T, Schuetze G, Niessner M, Goralczyk A, Meller J, et al. Two-stage hepatectomy (R0) with portal vein ligation--towards curing patients with extended bilobular colorectal liver metastases. Int J Colorectal Dis. 2009;24(4):409-18.
- Tsim N, Healey AJ, Frampton AE, Habib NA, Bansi DS, Wasan H, et al. Two-stage resection for bilobar colorectal liver metastases: R0 resection is the key. Ann Surg Oncol. 2011;18(7):1939-46.
- Karoui M, Vigano L, Goyer P, Ferrero A, Luciani A, Aglietta M, et al. Combined first‐stage hepatectomy and colorectal resection in a two‐stage hepatectomy strategy for bilobar synchronous liver metastases. Br J Surg. 2010;97(9):1354-62.
- Narita M, Oussoultzoglou E, Jaeck D, Fuchschuber P, Rosso E, Pessaux P, et al. Two‐stage hepatectomy for multiple bilobar colorectal liver metastases. Br J Surg. 2011;98(10):1463-75.
- Wicherts DA, Miller R, de Haas RJ, Bitsakou G, Vibert E, Veilhan LA, et al. Long-term results of two-stage hepatectomy for irresectable colorectal cancer liver metastases. Ann Surg. 2008;248(6):994-1005.
- Passot G, Chun YS, Kopetz SE, Zorzi D, Brudvik KW, Kim BJ, et al. Predictors of safety and efficacy of 2-stage hepatectomy for bilateral colorectal liver metastases. J Am Coll Surg. 2016;223(1):99-108.
- Naumov GN, Akslen LA, Folkman J. Role of angiogenesis in human tumor dormancy: animal models of the angiogenic switch. Cell cycle. 2006;5(16):1779-87.
- Yokoyama Y, Nagino M, Nimura Y. Mechanisms of hepatic regeneration following portal vein embolization and partial hepatectomy: a review. World J Surg. 2007;31(2):367-74.
- Lam VW, Laurence JM, Johnston E, Hollands MJ, Pleass HC, Richardson AJ. A systematic review of two‐stage hepatectomy in patients with initially unresectable colorectal liver metastases. HPB (Oxford). 2013;15(7):483-91.
- Oldhafer KJ, Stavrou GA, van Gulik TM. ALPPS-where do we stand, where do we go?: eight recommendations from the first international expert meeting. Ann Surg. 2016;263(5):839-41.
- Björnsson B, Sparrelid E, Røsok B, Pomianowska E, Hasselgren K, Gasslander T, et al. Associating liver partition and portal vein ligation for staged hepatectomy in patients with colorectal liver metastases--intermediate oncological results. Eur J Surg Oncol. 2016;42(4):531-7.
- Rosok BI, Björnsson B, Sparrelid E, Hasselgren K, Pomianowska E, Gasslander T, et al. Scandinavian multicenter study on the safety and feasibility of the associating liver partition and portal vein ligation for staged hepatectomy procedure. Surgery. 2016;159(5):1279-86.
- Oldhafer KJ, Donati M, Jenner RM, Stang A, Stavrou GA. ALPPS for patients with colorectal liver metastases: effective liver hypertrophy, but early tumor recurrence. World J Surg. 2014;38(6):1504-9.
- Van Lienden KP, Van Den Esschert JW, De Graaf W, Bipat S, Lameris JS, van Gulik TM, et al. Portal vein embolization before liver resection: a systematic review. Cardiovasc Intervent Radiol. 2013;36(1):25-34.
- Simoneau E, Aljiffry M, Salman A, Abualhassan N, Cabrera T, Valenti D, et al. Portal vein embolization stimulates tumour growth in patients with colorectal cancer liver metastases. HPB (Oxford). 2012;14(7):461-8.
- Knoefel WT, Gabor I, Rehders A, Alexander A, Krausch M, Schulte am EJ, et al. In situ liver transection with portal vein ligation for rapid growth of the future liver remnant in two‐stage liver resection. Br J Surg. 2013;100(3):388-94.
- Kokudo N, Tada K, Seki M, Ohta H, Azekura K, Ueno M, et al. Proliferative activity of intrahepatic colorectal metastases after preoperative hemihepatic portal vein embolization. Hepatology. 2001;34(2):267-72.
- Schadde E, Ardiles V, Slankamenac K, Tschuor C, Sergeant G, Amacker N, et al. ALPPS offers a better chance of complete resection in patients with primarily unresectable liver tumors compared with conventional-staged hepatectomies: results of a multicenter analysis. World J Surg. 2014;38(6):1510-9.
- Ratti F, Cipriani F, Gagliano A, Catena M, Paganelli M, Aldrighetti L. Defining indications to ALPPS procedure: technical aspects and open issues. Updates Surg. 2014;66(1):41-9.
- Clavien PA, Lillemoe KD. Note from the editors on the ALPPS e-Letters-to-the-Editor. Ann Surg. 2012;256(3):552.
- Andriani OC. Long-term results with associating liver partition and portal vein ligation for staged hepatectomy (ALPPS). Ann Surg. 2012;256(3):e5.
- Hernandez-Alejandro R, Bertens KA, Pineda-Solis K, Croome KP. Can we improve the morbidity and mortality associated with the associating liver partition with portal vein ligation for staged hepatectomy (ALPPS) procedure in the management of colorectal liver metastases? Surgery. 2015;157(2):194-201.
- Xiao L, Li JW, Zheng SG. Totally laparoscopic ALPPS in the treatment of cirrhotic hepatocellular carcinoma. Surg Endosc. 2015;29(9):2800-1.
- Li J, Kantas A, Ittrich H, Koops A, Achilles EG, Fischer L, et al. Avoid “All-Touch” by hybrid ALPPS to achieve oncological efficacy. Ann Surg. 2016;263(1):e6-7.
- Petrowsky H, Györi G, de Oliveira M, Lesurtel M, Clavien PA. Is partial-ALPPS safer than ALPPS? A single-center experience. Ann Surg. 2015;261(4):e90-2.
- Chan AC, Pang R, Poon RT. Simplifying the ALPPS procedure by the anterior approach. Ann Surg. 2014;260(2):e3.
- Gauzolino R, Castagnet M, Blanleuil ML, Richer JP. The ALPPS technique for bilateral colorectal metastases: three “variations on a theme”. Updates Surg. 2013;65(2):141-8.
- Schnitzbauer AA, Schadde E, Linecker M, Machado MA, Adam R, Malago M, et al. Indicating ALPPS for colorectal liver metastases. A critical analysis of patients in the international ALPPS registry. Surgery. 2018.
- Kambakamba P, Linecker M, Schneider M, Reiner CS, Nguyen-Kim TDL, Limani P, et al. Impact of associating liver partition and portal vein ligation for staged hepatectomy (ALPPS) on growth of colorectal liver metastases. Surgery. 2018;163(2):311-7.
- Schadde E, Ardiles V, Robles-Campos R, Malago M, Machado M, Hernandez-Alejandro R, et al. Early survival and safety of ALPPS: first report of the international ALPPS registry. Ann Surg. 2014;260(5):829-36.
- Sandström P, Røsok BI, Sparrelid E, Larsen PN, Larsson AL, Lindell G, et al. ALPPS improves resectability compared with conventional two-stage hepatectomy in patients with advanced colorectal liver metastasis: results from a scandinavian multicenter randomized controlled trial (LIGRO trial). Ann Surg. 2018;267(5):833-40.
- Ratti F, Schadde E, Masetti M, Massani M, Zanello M, Serenari M, et al. Strategies to increase the resectability of patients with colorectal liver metastases: a multi-center case-match analysis of ALPPS and conventional two-stage hepatectomy. Ann Surg Oncol. 2015;22(6):1933-42.
- Schadde E, Raptis DA, Schnitzbauer AA, Ardiles V, Tschuor C, Lesurtel M, et al. Prediction of mortality after ALPPS stage-1 an analysis of 320 patients from international ALPPS registry. Ann Surg. 2015;262:780-6.
- Belghiti J. How could we image the future in hepatic surgery. Hepatobiliary Surg Nutr. 2016;5(4):279-80.