Case Report
Mycotic Peripheral Pulmonary Arterial Pseudoaneurysm in Patent Ductus Arteriosus with Infective Endocarditis: A Rare but Fatal Complication
Kartik Patel1*, Suresh Kumar Rajan1, Pankaj Garg1, C Anantnarayan1, Yashpal Rana2 and Trushar Gajjar1
1Department of Cardiovascular and Thoracic Surgery, U N Mehta Institute of Cardiology and Research Center, India
2Department of Cardiac Radiology, U N Mehta Institute of Cardiology and Research Center, India
*Corresponding author: Kartik Patel, Department of Cardiovascular and Thoracic Surgery, U N Mehta Institute of Cardiology and Research Center, New Civil Hospital Campus, Asarwa, Ahmadabad, Gujarat, 380016, India
Published: 03 May, 2018
Cite this article as: Patel K, Rajan SK, Garg P, Anantnarayan C, Rana Y, Gajjar T. Mycotic Peripheral Pulmonary Arterial Pseudoaneurysm in Patent Ductus Arteriosus with Infective Endocarditis: A Rare but Fatal Complication. World J Surg Surgical Res. 2018; 1: 1007.
Abstract
Patent ductus arteriosus with infective endocarditis complicated by peripheral pulmonary arterial mycotic pseudoaneurysm is rare now-a-days especially due to early diagnosis and more efficient antibacterial drug management. We here described a case report of PDA with infective endocarditis complicated by peripheral pulmonary artery mycotic pseudoaneurysm which was managed successfully via ligation of PDA and left lower lobectomy.
Case Presentation
A 7 year female child was admitted to department of paediatric cardiology with complaints of
dyspnoea NYHA II and high grade fever since 15 days. On general examination, she had continuous
murder in left infra clavicular region. On chest x-ray there was cardiomegaly with dilated
pulmonary arteries along with pulmonary plethora without any soft tissue shadow in lung field.
2D echocardiography showed moderate sized Patent Ductus Arteriosus (PDA) with vegetation on
main pulmonary artery 6 mm × 6 mm in sized. Blood culture showed growth of streptococcus
viridians. So diagnosis of moderate PDA with infective endocarditis was made and she was started
on antibiotics according to culture sensitivity. She responded well after starting the antibiotics and
her fever subsided. After 5 days, she developed massive haemoptysis for which urgent Computed
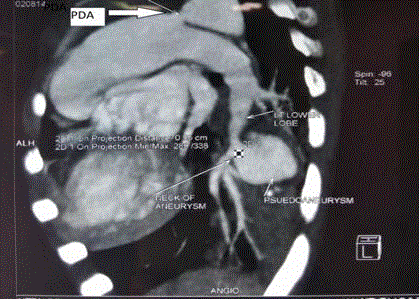
Angiography (CT) was performed. Contrast CT scan of pulmonary artery showed PDA with
diameter of 14 mm at aortic end and 7.5 mm at pulmonary end with 3.2 cm × 2.9 cm × 2.5 cm
pseudo aneurysm of anteromedial basal branch of left lower pulmonary artery within the cavity
along with prolapse of left lower lobe (Figure 1 and 2).
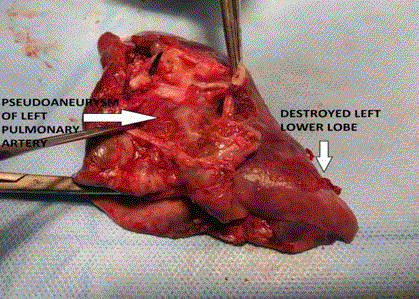
Patient was stabilized and posted for urgent surgery. Patient was approached through 4th left
posterolateral thoracotomy. PDA was looped and ligated. Left lower lobectomy was performed.
Procedure was uneventful. Patient was extubated within 2 hours and remained stable without any
haemoptysis or fever in post op period. She was discharge after completion of 4 weeks of antibiotic
course. Till date patient was asymptomatic and still in follow up.
Discussion
The term mycotic aneurysm, first described by Osler, has been used to denote infection involving
arterial wall [1]. Mycotic pseudo aneurysm of pulmonary artery in case of infective endocarditis
with PDA is rare now-a-days due to early diagnosis and availability of efficient antibacterial drugs
[2]. Most of the authors reported a case of mycotic aneurysm in patients with right sided infective
endocarditis [3,4]. This case is rare as patient developed pseudo aneurysm of pulmonary artery
despite being on antibacterial treatment and was developed within a short span of 5 days as the chest
x-ray on admission failed to show any soft tissue shadow.
Pulmonary artery mycotic pseudo aneurysms by definition do not have a covering of all three
layers of the arterial wall with infection of the involved artery. When occurring within a consolidated
or infected lung, it can erode the bronchial tree and this communication with the airways, may
result in massive hemoptysis or even death. Early recognition and prompt treatment may help to
reduce the associated mortality rate. The various options available for management includes: 1)
Surgical 2) Catheter based intervention. The catheter based interventions are now-a-days preferred due to several advantages which includes minimal trauma to normal
lung parenchyma, minimal blood loss and smaller incision. However
there are several limitations of this approach 1. It cannot be offered in
a patient with unsuitable anatomy like patients with main pulmonary
artery aneurysm 2. Persistent aneurysm and persistent infection
which can be present in up to 22% of patients 3 [5,6]. Non-availability
of facilities in every center; surgery remains main stay of treatment
in a patient with destroyed lung parenchyma, aneurysms involving
main pulmonary artery and where endovascular treatment not
possible. The options available are resection of aneurysm, lobectomy,
patch repair or dacron graft replacement [7-9]. In index case, there
was peripheral mycotic pseudo aneurysm within the cavity with
destroyed lower lobe of left lung along with large PDA. These findings
made patient unsuitable for percutaneous treatment so PDA ligation
with left lower lobectomy was performed successfully.
Figure 1
Figure 1
Contrast CT Angiography showing large pseudoaneurysm of anteromedial branch of left lower pulmonary artery with patent ductus arteriosus.
Figure 2
Conclusion
Large patent ductus arteriosus complicated by infective endocarditis with large peripheral mycotic pseudo aneurysm of pulmonary artery complicated with massive hemoptysis is rare now-a-days. Along with antibiotics, emergent Surgery remained the treatment of choice in this condition.
References
- Osler W. The Gulstonian lectures on malignant endocarditis. Br Med J. 1885;1(1262):467-70.
- Charlton RW, Du Plessis LA. Multiple pulmonary artery aneurysms. Thorax. 1961;16(4):364-71.
- Benvenieste O, Bruneel F, Bedos JP, Wolff M, Lesèche G, Leport C, et al. Ruptured mycotic pulmonary artery aneurysm: an unusual complication of right-sided endocarditis. Scand J Infect Dis. 1998;30(6):626-9.
- Chellamuthu S, John RB. Treatment of a large pulmonary artery pseudoaneurysm secondary to fungal infection using amplatzer plugs: New embolisation devices for the management of haemoptysis. Respir Med Case Rep. 2012;5:78-80.
- Priya J, Sanjiv S, Rajnish J, Randeep G. Transcatheter treatment of pulmonary artery pseudoaneurysm using a PDA closure device. Diagn Interv Radiol. 2011;17(1):92-4.
- Lee WK, Mossop PJ, Little AF, Fitt GJ, Vrazas JI, Hoang JK, et al. Infected (mycotic) aneurysms: spectrum of imaging appearances and management. Radiographics. 2008;28(7):1853-68.
- Bartter T, Irwin RS, Nash G. Aneurysms of the pulmonary arteries. Chest. 1988;94:1065-75.
- Remy J, Smith M, Lemaitre L, Marache P, Fournier E. Treatment of massive hemoptysis by occlusion of a Rasmussen aneurysm. AJR Am J Roentgenol. 1980;135(3):605-6.
- Williams TE, Schiller M, Craenen J, Hosier DM, Sirak HD. Pulmonary artery aneurysm: successful excision and replacement of the main pulmonary artery. J Thorac Cardiovasc Surg. 1971;62(1):63-7.