Research Article
Fresh Frozen Plasma versus Albumin in Treatment of Cerebral Vasospasm in Subarachnoid Hemorrhage: A Historical Cohort Study
Abdolkarim Rahmanian1, Alireza Mohsenian Sisakht1,2, Nima Derakhshan1*, Najme Karamzade Ziarati3, Hadi Raeisi Shahraki4, Bijan Najafi5 and Babak Daneshfard5
1Department of Neurosurgery, Shiraz University of Medical Sciences, Iran
2Student Research committee, Iran University of Medical Sciences, Iran
3Student Research Committee, Tehran University of Medical Sciences, Iran
4Department of Biostatistics, School of Medicine, Shiraz University of Medical Sciences, Iran
5Student research committee, Shiraz University of Medical Sciences, Iran
*Corresponding author: Nima Derakhshan, Department of Neurosurgery, Shiraz University of Medical Sciences, Shiraz, 71937-11351, Iran
Published: 16 Apr 2018
Cite this article as: Rahmanian A, Sisakht AM, Derakhshan N, Ziarati NK, Shahraki HR, Najafi B, et al. Fresh Frozen Plasma versus Albumin in Treatment of Cerebral Vasospasm in Subarachnoid Hemorrhage: A Historical Cohort Study. World J Surg Surgical Res. 2018; 1: 1002.
Abstract
Background: Patients with Subarachnoid Hemorrhage (SAH) are susceptible of developing cerebral vasospasm, and intravascular volume expansion remains one of the mainstays of treatment. Albumin has been introduced as the customary volume expander agent for prevention and treatment of cerebral vasospasm; however Fresh Frozen Plasma (FFP) with its rich protein content is also a reasonable substitute for albumin. Unfortunately, albumin solution was not as available as recently till 2011 and prior to that, FFP was used instead, as a common means of inducing hypervolemia in patients sustaining cerebral vasospasm, in many source-limiting areas, such as southern Iran.
Objectives: To compare FFP transfusion vs. albumin infusion in terms of functional outcome and thrombo-embolic events in patients with aneurysmal SAH.
Methods: Analysis of 474 patients with aneurysmal SAH who underwent surgical clipping between September 2007 and March 2016, in Shiraz Nemazee Hospital (southern Iran) affiliated in Shiraz Nemazee Hospital was carried out in a retrospective fashion. The functional outcome and also incidence of venous thrombo-embolic events including Deep Vein Thrombosis (DVT) and Pulmonary Thrombo-Embolism (PTE) were assessed and compared between the two subgroups of patients taking FFP transfusion vs. albumin infusion.
Results: Functional outcome was better in patients taking albumin infusion; however there was no difference in the rate of thrombo-embolic events between the two groups.
Conclusion: Albumin is considered the standard of care for hypervolemic therapy in cerebral vasospasm; in source-limited areas FFP can be considered an inexpensive alternative to albumin without further increment in thrombo-embolic events. However, the use of volume expanders should only be considered in angiographic spasm and prophylactic usage is not a common practice anymore.
Keywords: Aneurysmal SAH; Cerebral vasospasm; Fresh frozen plasma; Albumin; PTE; DVT
Introduction
Patients with SAH are susceptible to develop cerebral vasospasm post-operatively cerebral vasospasm which is proved to worsen outcomes significantly [1-3]. Several therapeutic strategies have proved useful in prevention and treatment of cerebral vasospasm namely hemodilution, hypertensive therapy and hypervolemic therapy. Enhancing intravascular volume preserves cerebral perfusion pressure and avoids ischemic sequels of cerebral vasospasm in aneurysmal SAH patients [4,5]. Albumin infusion is the best known volume expander in the setting of SAH [6,7]. Albumin, like other proteins possesses an oncotic or colloid osmotic pressure, contributing to one of the main Starling forces which control the passage of fluid across the vessel walls. By administering albumin, fluid will remain in the intravascular space and enhanced intra-vascular volume, prevents vasospasm and provides adequate perfusion to the supplied areas.
Fresh Frozen Plasma (FFP) is derived from blood and contains proteins of coagulation, fibrinolytic and complements system as well as albumin, carbohydrate, fat and minerals similar to circulation.
Although it contains less albumin than most albumin solution preparations, having hyperosmolar, hypernatremic (172 mEq/Lit) and hypochloremic (73 mEq/Lit) properties makes it an interesting substitute for albumin solutions as volume expanding agents in the setting of cerebral vasospasm.
However, side effects was seen more often and more severe with FFP transfusion than albumin infusion which has hindered its widespread usage over albumin [8,9] despite its lower costs [10] thereby, emphasizing albumin as the customary intra-vascular volume expander in patients with SAH.
Patients sustaining SAH have also innate propensity for developing thrombo-embolic complications such as DVT or PTE. Venous thrombo-embolism (VTE) is a well-known etiology of mortality in patients with SAH; thus, mechanical and pharmacologic VTE prophylaxis remains an important part of their management [1,11].
Here, the question arises whether or not we can use FFP and albumin interchangeably as volume expanding agents in SAH patients, considering the potential pro-coagulant effects of FFP.
Albumin solutions were not as available as they become recently, and have a considerable contribution to the hospital bill of patients with SAH. A simple thumbnail accounting of the comparison of daily costs, renders about $57.6 for Albumin (1 gr/kg/day) vs. an average of $27.2 for FFP (15 ml/kg/day) [10].
Due to limited availability of albumin solutions, we used FFP till September 2010 and afterwards albumin became widely available we switched to albumin infusion as the volume expanding agent of choice, like other neurovascular centers.
Here in, we aim to compare the functional outcome and also the incidence of venous thrombo-embolic events (DVT and PTE) in two groups of patients in a retrospective fashion; First group taking FFP (prior to September 2010) and the second group taking albumin infusion between September 2010 and March 2016.
Table 1
Table 1
Comparison of Age, Gender, Thrombo-embolic events and functional outcome between the two groups.
Materials and Methods
Study population
A total of 474 patients with aneurysmal SAH who underwent clipping in Shiraz Nemazee Hospital (the main referral neurovascular center of Southern Iran) between September 2007 and March 2016 were included in this retrospective analysis [12,13].
All patients with the above criteria were included in the study and those who had incomplete hospital records for assessment hospital course and thromboembolic events were excluded from the study (110 individuals). Soa total of 364 patients were eligible to enter the study.
Intervention strategies
Patients were divided into two groups. Group A consisting of 117 patients taking FFP intravenously (1 unit every 8 hours), the traditional agent being used between September 2007 and September 2011 and group B with 247 patients for whom albumin infusion was administered (between October 2010 and March 2016). Post-operative VTE prophylaxis and other therapeutic measures were similar within both groups.
Route of administration
Transfusion of 1 unit (250 ml) FFP and intravenous infusion of one 100 ml vial of 20% human albumin were administered in groups A and B, respectively, every 8 hours) for 10 consecutive days.
Data gathering strategy
Data collecting forms were designed containing patients’ demographic data, aneurysm characteristics, surgical and neuro-critical events and pharmacologic agents that were used.
Outcome measures
Incidence of DVT and PTE was investigated by using ultrasonography for DVT and Spiral chest computed tomography scans for PTE, respectively, in patients who had developed sign or symptoms of venous thrombosis according to their hospital and outpatient records [14-16].
Functional outcome at 6 month were measured as modified Rankin Scale (mRS) which was obtained by patients’ outpatient records as well as phone calls. Patients’ outcomes were categorized as favorable for mRS 0 to 2 and unfavorable for mRS 3 to 6 [17].
Statistical analysis
All the statistical analyses were performed using statistical package for social sciences (SPSS Inc, Chicago, Illinois, USA) version 22.0. Data are reported as mean ± SD as appropriate. Non-parametric data were compared between the two groups using chi-square test. Logistic regression analysis was used to examine the effect of FFP vs. albumin on DVT by adjusting sex and age of the patients. A P-value less than 0.05 were considered statistically significant.
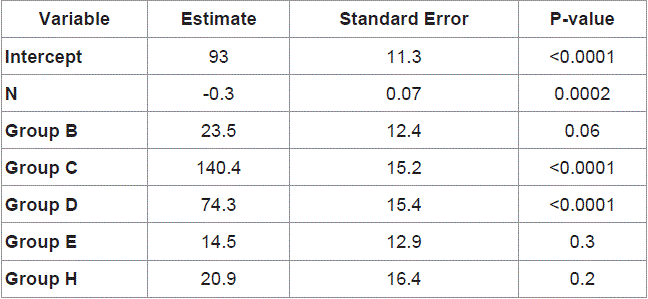
Table 2
Results
A total of 364 patients with aneurysmal SAH aged 46.8 ± 14.3 years were included in this analysis, 117(32.1%) in the FFP group and 247 (67.9%) in the albumin group. The sexual distribution of studied population was 51.4% males against 48.6% female. Chi-square test revealed that there was no gender preference in the study groups (P=0.64) and available data regarding patients’ Glasgow Coma Scale (GCS) and clinical Hunt and Hess (H&H) grade were also similar between the groups. However, comparing the mean age of patients between the two study groups using independent T-test revealed that patients in the albumin group was significantly younger than FFP group (45.3 vs. 50.1, P=0.003).
Eighteen (4.9%) of the studied patients developed DVT, 6.8% in the FFP group and 4% in the albumin group, which was not different between the two study groups. (P=0.25) Also, in the FFP group 1 patient (0.9%) was diagnosed PTE whereas in the albumin group 6 (2.4%) patients had PTE. Fisher exact test indicated that this difference was not statistically significant (P=0.44).
Functional outcome at 6 months post-operatively were surveyed by calling the patients in 277 out of 364 patients (76%) it was available to evaluate and for the other 87 (24%) outcomes couldn’t be assessed due to changes in phone number. These results indicated that favorable outcome were significantly higher in patients who received albumin instead of FFP (96.4% vs. 80.9%, P<0.001) (Table 1).
In order to assess simultaneous effect of age, gender and albumin infusion instead of FFP on DVT, multivariate logistic regression analysis was implemented and the results are summarized in Table 2. In the proposed model, age is the only variable which had a significant effect on DVT (P=0.005) so that for each year increase in age, odds of DVT in SAH patients increased by 6%. Table 2 also shows that albumin infusion instead of FFP can decrease the odds of DVT by 36%, but this effect was not significant (P=0.54).
Discussion
Cerebral vasospasm accompanied with sub-arachnoid hemorrhage is one of the commonest scenarios which have the potential to worsen their outcome. Strategies at alleviating this condition have been shown to improve survival and neurologic outcome of patients with SAH. Nimodipine and the well known triple-H therapy have been the mainstays of management of cerebral vasospasm. Triple-H therapy works through inducing hypervolemia, hypertension and hemodilution by altering the Starling forces to maintain intravascular volume to preserve cerebral perfusion pressure.
Hypervolemic therapy can be achieved by crystalline solutions, albumin infusions, blood derivatives such as FFP, etc., with each having its own pros and cons.
To evaluate the risk of thrombo-embolic events and the benefit on functional outcome in patients with SAH undergoing hypervolemic therapy, we compared the patients taking albumin with those who were transfused with FFP. Side effects of FFP, albeit rare, consist of transfusion related acute lung injury, transfusion associated circulatory overload, allergic/anaphylactic reactions, transmission of infections, febrile non-hemolytic transfusion reactions, RBC allo-immunization, and hemolytic transfusion reactions [9] which were not noticed in any of our patients. Albumin has its own side effects such as immediate allergic-type reactions which are not as frequent and serious as with FFP transfusion [10].
Not only the better side effect profile, but also better functional outcomes represents albumin as a better choice over FFP. However the best management of delayed cerebral ischemia in the setting of SAH is still a matter of debate with pros and cons for each therapeutic modality. A revised recommendation for the use of euvolemic-induced hypertension rather than triple-H therapy has also been suggested as the primary method for treatment of most patients with cerebral vasospasm, which utilizes isotonic crystalloids and avoids the adverse effects of the two aforementioned modalities.
Another point to be considered is that in neurovascular centers with limited sources FFP can be considered as a good and economic alternative to albumin as they have quite the same efficacy without the concerns of increase in thrombo-embolic events and with taking into account that acute immunologic adverse reactions occur very rarely.
To minimize the inevitable confounding bias which is typically observed in retrospective cohort studies, both groups were analytically evaluated for parameters such as primary GCS and H&H scores as well as their demographic features and medical comorbidities to assure that the two groups are similar in this regard.
However, some limitations were also faced such as incomplete hospital records which made us exclude 110 individuals and another 87 who were not reachable via phone call to determine their functional outcome. These limitations were covered by evaluation of as many as 474 patients in the author’s series between 2007 and 2016 which provides a reliable study population.
The strength of this study is the evaluation of a large number of patients operated by the same surgeon at a referral neuro-vascular center in a 9-year time frame with providing a long post-operative follow-up ranging from 6 months to almost 9 years [18].
The goal of this historical cohort is to evaluate the risk of thromboembolic events as well as functional outcome in patients receiving FFP vs. albumin. As recently revised in guidelines of a SAH management, the prophylactic use of these agents is not a common practice anymore and should be only considered in patients with angiographic-confirmed vasospasm.
Conclusion
Although better functional outcomes was noted in patients taking albumin infusion, there was no increase in thrombo-embolic events and FFP can be considered an economic viable alternative for albumin, as volume expanders in patients sustaining cerebral vasospasm after SAH. However, the use of volume expanders should only be considered in angiographic spasm and prophylactic usage is not a common practice anymore.
References
- Suarez JI, Tarr RW, Selman WR. Aneurysmal subarachnoid hemorrhage. N Engl J Med. 2006;354(4):387-96.
- Keyrouz SG, Diringer MN. Clinical review: Prevention and therapy of vasospasm in subarachnoid hemorrhage. Crit Care. 2007;11(4):220.
- Frontera JA, Fernandez A, Schmidt JM, Claassen J, Wartenberg KE, Badjatia N, et al. Defining vasospasm after subarachnoid hemorrhage: what is the most clinically relevant definition? Stroke. 2009;40(6):1963-8.
- Lee KH, Lukovits T, Friedman JA. “Triple-H” therapy for cerebral vasospasm following subarachnoid hemorrhage. Neurocrit Care. 2006;4(1):68-76.
- Treggiari MM. Hemodynamic management of subarachnoid hemorrhage. Neurocrit Care. 2011;15(2):329-35.
- Suarez JI, Martin RH, Calvillo E, Dillon C, Bershad EM, MacDonald RL, et al. The Albumin in Subarachnoid Hemorrhage (ALISAH) multicenter pilot clinical trial: safety and neurologic outcomes. Stroke. 2012;43(3):683-90.
- Suarez JI, Shannon L, Zaidat OO, Suri MF, Singh G, Lynch G, et al. Effect of human albumin administration on clinical outcome and hospital cost in patients with subarachnoid hemorrhage. J Neurosurg. 2004;100(4):585-90.
- Pandey S, Vyas GN. Adverse effects of plasma transfusion. Transfusion. 2012;52(1):65s-79s.
- Liumbruno G, Bennardello F, Lattanzio A, Piccoli P, Rossettias G. Recommendations for the use of albumin and immunoglobulins. Blood Transfus. 2009;7(3):216-34.
- Roy RR, Al Mamun A, Haque SS, Mitra A, Muinuddin G, Rahman H. Albumin versus fresh frozen plasma in managing diuretic resistant edema in children with idiopathic nephrotic syndrome. IOSR J Pharm. 2015;5(7):40-3.
- Serrone JC, Wash EM, Hartings JA, Andaluz N, Zuccarello M. Venous thromboembolism in subarachnoid hemorrhage. World Neurosurg. 2013;80(6):859-63.
- Rahmanian A, Jamali M, Razmkon A, Kivelev J, Romani R, Alibai EA, et al. Benefits of early aneurysm surgery: Southern Iran experience. Surg Neurol Int. 2012;3:156.
- Rahmanian A, Ghaffarpasand F, Derakhshan N. Surgical outcome of patients with very small intracranial aneurysms: A single-center experience from southern Iran. World Neurosurg. 2017;98(2):470-8.
- Kory PD, Pellecchia CM, Shiloh AL, Mayo PH, DiBello C, Koenig S. Accuracy of ultrasonography performed by critical care physicians for the diagnosis of DVT. Chest. 2011;139(3):538-42.
- Kim BH, Seo JB, Chae EJ, Lee HJ, Hwang HJ, Lim C. Analysis of perfusion defects by causes other than acute pulmonary thromboembolism on contrast-enhanced dual-energy CT in consecutive 537 patients. Eur J Radiol. 2012;81(4):e647-52.
- Raslan AM, Fields JD, Bhardwaj A. Prophylaxis for venous thrombo-embolism in neurocritical care: a critical appraisal. Neurocrit Care. 2010;12(2):297-309.
- Konczalla J, Platz J, Schuss P, Vatter H, Seifert V, Güresir E. Non-aneurysmal non-traumatic subarachnoid hemorrhage: patient characteristics, clinical outcome and prognostic factors based on a single-center experience in 125 patients. BMC Neurol. 2014;14(1):140.
- Rahmanian A, Derakhshan N, Mohsenian Sisakht A, Karamzade Ziarati N, Raeisi Shahraki H, Motamed S. Risk Factors for Unfavorable Outcome in Aneurysmal Subarachnoid Hemorrhage Revisited; Odds and Ends. Bull Emerg Trauma. 2018;6(2):133-140.